This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
What Is Jaundice? Get the Facts on Neonatal vs. Adult Jaundice
November 2, 2016
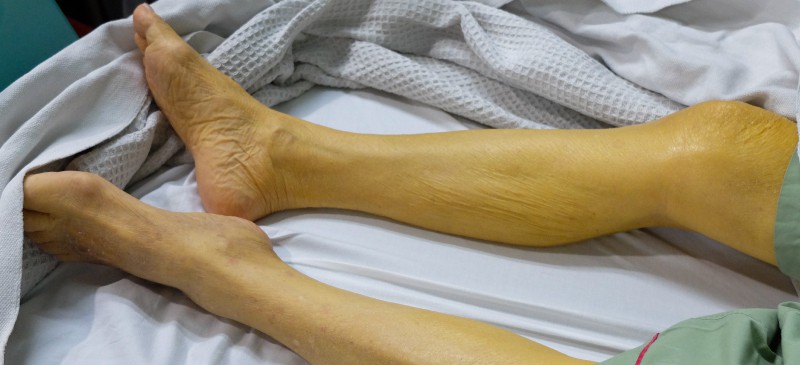
The term jaundice is derived from the French word “jaune,” meaning yellow, which make sense because that’s exactly what jaundice does — it causes the skin and eyes to have a yellow discoloration.
Neonatal jaundice is one of the most common conditions requiring medical attention in newborn babies. Approximately 60 percent of term and 80 percent of preterm babies develop this condition in the first week of life, which is why the American Academy of Pediatrics recommends that every newborn be examined for jaundice during routine medical checks after birth. (1) Adult jaundice is not as common, but it serves as a sign of a more serious underlying condition.
Jaundice has to be taken seriously because if it lasts for more than a few weeks and it goes untreated, it can lead to serious health problems. There are warning signs, most notably the obvious skin discoloration, and natural ways to avoid increasing your (or your baby’s) risk of developing this discoloration condition.
What Is Jaundice?
Jaundice (also known as icterus) is a condition in which the skin and whites of the eyes become yellow, urine darkens and the color of stool becomes lighter than normal. This results from the accumulation of bilirubin in the skin and mucous membranes, a condition known as hyperbilirubinemia. Experts say that jaundice can be recognized when the serum bilirubin rises to 2–2.5 milligrams per deciliter, but sometimes yellow skin coloration isn’t noticeable until the serum bilirubin is at least 7–8 milligrams per deciliter. (2)
Bilirubin is a yellow chemical in hemoglobin, the substance that carries oxygen to the blood and serves as a breakdown product of the red cells in blood. As red blood cells break down, our bodies build new cells to replace them, and the old ones are processed through the liver for further metabolism and excretion.
There are two types of bilirubin: unconjugated bilirubin and conjugated bilirubin. Unconjugated bilirubin is insoluble in water and is the term used before the bilirubin has been processed by the liver. Once it is processed by the liver, the bilirubin is then conjugated, which means it is more water-soluble, and it then travels to the gallbladder where it’s stored. Finally, the bilirubin makes its way into the intestines, where a portion is excreted in stool and some is metabolized by the intestinal bacteria and excreted in urine.
When the liver cannot metabolize the blood cells as they break down, or the bilirubin is not properly excreted from the body, there’s a buildup of bilirubin, which is why the skin may appear to be yellow. Cholestatic jaundice occurs when the bile stops flowing from the liver to the small intestines.
Neonatal jaundice is when newborn babies have a yellow coloration of the skin and the whites of the eyes. This is usually harmless and disappears on its own within two to three weeks.
Adults can also develop jaundice, and it may be caused by a variety of medical conditions, some of which are serious and potentially life-threatening. Adults who develop it need to have a medical examination in order to determine the cause.
Jaundice Causes
Neonatal (Newborn Jaundice)
Jaundice is common among newborns because the metabolism, circulation and excretion of bilirubin are slower than in adults. Newborn babies’ red blood cells have shorter life spans than those of adults, and the concentration of red blood cells in newborns is also higher. Usually, hyperbilirubinemia is harmless in newborn babies, and it only develops because the baby’s liver isn’t mature enough to get rid of all the bilirubin in the bloodstream. In fact, a study published in Archives of Disease in Childhood found that of the 20 percent of newborn babies who are jaundiced, only 2.5 percent of them need treatment. (3) But sometimes, the discoloration is caused by an underlying disease or babies are at risk of developing high levels of bilirubin that can become dangerous.
Neonatal jaundice is the term for the common, usually harmless form of jaundice that’s seen in many newborn babies in the first weeks of life. This is usually labeled a harmless condition, and it improves without any serious issues. However, it’s still important to see your pediatrician because occasionally a rare kind of brain damage known as kernicterus can occur if bilirubin levels are elevated for too long.
Adult Jaundice
Jaundice in adults (or jaundice that isn’t simply physiological) can be caused by a wide variety of harmless or life-threatening disorders that affect the normal metabolism or excretion of bilirubin. There are three phases in adults: pre-hepatic jaundice (before transportation of blood to the liver), hepatic jaundice(when the blood has reached the liver) and post-hepatic jaundice(when blood has left the liver and will be excreted from the body).
Jaundice caused during the pre-hepatic phase is due to the excessive destruction of red blood cells, which can be due to various conditions, such as sickle cell disease, malaria, thalassemia (a blood disorder), drug reactions, toxin reactions or autoimmune diseases. The increase in bilirubin levels that are present in the bloodstream overwhelm the liver’s ability to properly metabolize the bilirubin fast enough. (4)
During the hepatic liver phase, when the blood has reached the liver, jaundice may be caused by conditions such as viral hepatitis, cirrhosis, crigler-najjar syndrome, Gilbert’s syndrome, liver disease, liver cancer and autoimmune disorders. During the post-hepatic phase, it occurs because of an obstruction in the excretion of drainage of the bilirubin in the liver. The obstruction can be caused by certain types of cancer (pancreatic, gallbladder and bile duct cancers), gallstones, pancreatitis, restriction of the bile ducts, cholangitis (a bacterial infection) and parasites. (5) It’s possible your doctor may advise you to have a procedure known as a endoscopic retrograde cholangiopancreatography (ERCP) in order to determine what is causing the obstruction.

Jaundice Symptoms and Warning Signs
Neonatal
The most common symptom or warning sign of jaundice is yellowing of the skin and the whites of the eyes. To check an infant for jaundice, press gently on the baby’s forehead or nose; if the skin where you pressed looks yellow, that’s a sign. Every infant should be examined for jaundice between the third and seventh day after birth because that’s when bilirubin levels usually peak.
Symptoms or warning signs of severe jaundice include the following:
- Skin becomes more yellow and it’s noticeable on the abdomen, arms or legs
- Baby isn’t gaining weight
- Baby is feeding poorly
- Baby acts sick or is difficult to awaken
- Baby makes high-pitched cries
Adult
Adults with jaundice will have a yellow discoloration of the skin and may also have yellowing of the whites of the eyes or mucous membranes. The discoloration may be barely noticeable in some adults and very obvious in others. Other symptoms in adults vary, but individuals may experience:
- Abdominal pain
- Fever
- Arthritis
- Headache
- Weight loss
- Swelling in legs or abdomen
- Rectal bleeding
- Nausea, vomiting and diarrhea
- Pale-colored stools
- Dark-colored urine
- Weakness (6)
Jaundice Risk Factors
Neonatal
Premature Birth
According to research published in Pediatric Nursing, around 80 percent of preterm infants (born before 38 weeks) develop jaundice. This is most likely because the infant’s liver is not mature enough to get rid of the bilirubin in the bloodstream. (7)
Delivery by Vacuum Extractor
A 2001 study published in Pediatrics evaluated 2,174 infants during their first days of life and indicated that significant hyperbilirubinemia was strongly associated with delivery by vacuum extractor. (8)
Breast-Feeding
Breast-fed babies are more likely to develop jaundice than bottle-fed babies; this is known as breastmilk jaundice. One reason this develops is because a factor in human milk increases the circulation of bilirubin. Another cause may be that the baby isn’t consuming enough calories as a result of breast-feeding difficulty; this may increase bilirubin concentrations. Research shows that optimal breast-feeding practices, which result in minimal initial weight loss and early onset of weight gain, are associated with reduced breastfeeding jaundice. (9)
Poor Weight Recovery
Research has found that newborns born at very low weights are more at risk of developing neonatal jaundice. A study published in the Indian Journal of Pediatrics evaluated very low-birth-weight infants born between 1995 and 1998. The incidence of significant neonatal jaundice among these infants was 76 percent, and 37 percent required an exchange transfusion. (10)
Blood Type
When the mother and baby are different blood types, and the baby receives antibodies from her mother’s blood through the placenta, the baby’s blood cells may break down more quickly. This creates a sudden buildup of bilirubin in the baby’s blood. This is called incompatibility jaundice, but today it can be prevented by giving the mother Rh immune-globulin injections. (11)
Adult
Although the risk factors for developing adult jaundice vary, some more common examples include:
Hereditary Conditions
Individuals with certain hereditary conditions are at a greater risk of developing it. Some conditions include Gilbert’s syndrome, thalassemia, hemolytic anemia and hereditary spherocytosis.
Excessive Alcohol Consumption
According to research published in Gastroenterology & Hepatology, the hallmark of alcoholic hepatitis is jaundice. Alcoholic hepatitis is an inflammatory condition of the liver that’s caused by excessive alcohol consumption over a long period of time. Severe alcoholic hepatitis is marked by bilirubin levels over 10–15 milligrams per deciliter. (12)
Exposure to Viral Infections
Exposure to viral hepatitis B, C and E, among other types of viral infections, can increase the disk of development. (13)
Conventional Treatment for Jaundice
Neonatal
Light Therapy
Light therapy, or phototherapy, changes the shape and structure of bilirubin molecules so they can be excreted in the urine and stool. The baby is placed under special lighting that does not emit ultraviolet light. This is a relatively common form of therapy for jaundice, and proper nursing care enhances the effectiveness while minimizing complications. The baby wears a diaper and soft eye patches in order to protect her eyes from the light. Parents may notice that the baby may have frequent or loose bowel movements that are greenish in color; this is the body removing bilirubin through stool, and it should only be temporary. (14)
Intravenous Immunoglobulin
If jaundice is caused by a blood type difference between the mother and baby, intravenous immunoglobulin is used to reduce the level of antibodies that the baby is carrying from the mother. This may decrease jaundice because the mother’s antibodies were contributing to the breakdown of blood cells in the baby. Studies show that IV immunoglobulin effectively reduces serum bilirubin levels and the need for a blood exchange transfusion, a procedure that has potential complications and carries a risk of mortality. (15)
Exchange Transfusion
An exchange transfusion serves as an emergency rescue procedure for severe neonatal hyperbilirubinemia, especially in underdeveloped regions of the world. This treatment involves repeatedly withdrawing small amounts of blood, diluting the bilirubin and mother’s antibodies, then transferring the blood back into the baby. An exchange transfusion can be a life-saving intervention in the face of rare but critical jaundice. (16)
Adult
For adult jaundice cases, the treatment plan depends entirely on the underlying cause. This is not a disease that develops on its own in adults; it’s the result of an already existing condition. For example, in order to treat jaundice caused by alcoholic hepatitis, the individual must first stop drinking alcohol. Jaundice caused by medications or drugs requires the individual to stop using these products. If the adult with jaundice has an infection, he may be treated with antibiotics; if he has an autoimmune disease, he may be treated with steroids. If the cause is unclear, the individual receives a laboratory workup that measures blood counts and tests for liver function and infectious hepatitis. If the cause remains unclear, doctors use abdominal imaging by ultrasonography or computed tomographic scanning. (17)
Natural Treatment & Prevention of Jaundice
Neonatal
More frequent feedings helps infants pass the the excess bilirubin in their stool. For mothers who are breast-feeding and have a low supply, supplementing with formula may be beneficial until the jaundice is treated. Symptoms should disappear within one to two weeks, but if they don’t, the infant must see her pediatrician.
According to research published in Pediatrics Clinic of North America, excessive frequency of exaggerated jaundice in a hospital or community population of breast-fed infants may be a warning that breast-feeding policies and support are not ideal for the establishment of good breast-feeding practices. Mothers who are breast-feeding need support from hospital staff or lactation consultants, especially in the first few days of an infant’s life. This ensures that the infant is eating enough and able to excrete bilirubin properly. (18)
Adult
In order to avoid the development of jaundice, adults should minimize their alcohol consumption, maintain a healthy weight, engage in physical exercise, manage their cholesterol and avoid hepatitis infections. Research shows that alcohol, for example, has been shown to affect bile acid uptake and secretion, resulting in the reduction of bile flow. Chronic alcohol use may damage the biliary system and result in result in fatty liver, hepatitis and cirrhosis, all varying levels of jaundice. (19)
Many drugs have been shown to play a role in the development of this condition as well. Certain drugs should be avoided because they’re classically identified with drug-induced liver disease. These include acetaminophen, penicillins, oral contraceptives, chlorpromazine (Thorazine), and estrogenic or anabolic steroids.
Key Points About Jaundice
- Jaundice is a condition in which the skin and whites of the eyes become yellow, urine darkens, and the color of stool becomes lighter than normal. This results from the accumulation of bilirubin in the skin and mucous membranes
- Neonatal jaundice occurs in infants who are just days old, and it typically disappears within one to two weeks. It’s more common in breast-fed babies than in formula-fed babies, and it’s more likely to develop in preterm infants or infants who are underweight.
- Adult jaundice occurs as a result of a condition or disease that impacts the bilirubin level. If the underlying cause is not discovered and treated, there can be serious or even life-threatening consequences.
- To treat neonatal jaundice, light therapy (or phototherapy) is commonly used in hospitals. More serious and invasive treatments include IV immunoglobulin and exchange transfusion. To treat infant jaundice naturally, mothers should feed their babies more frequently in order to increase the excretion of bilirubin.
- The treatment plan for adult jaundice depends entirely on the underlying cause. Adults can limit alcohol consumption, maintain a healthy weight and limit the drug of medications that may lead to liver issues.








