This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
9 Common Questions About Breast Milk
November 18, 2016
Breast milk is loaded with exactly the right nutrients in the exact amounts a new baby needs. Research shows that breast milk is not merely nutritious, but it contains a variety of factors with medicinal qualities that have profound roles in infant survival and health.
Although the industry continues to attempt to approve infant formula with the addition of compounds, such as fatty acids, oligosaccharides, nucleotides and lactoferrin, breast milk has such far-reaching effects on the infant’s immune response that optimal development depends heavily on its actions. It contains many hundreds to thousands of distinct bioactive molecules that protect against infection and inflammation and contribute to immune maturation, organ development and promotion of a healthy microbiome. (1) For this reason, all mothers should be encouraged and supported to continue breastfeeding for six months and beyond in order to promote the good health of their infants.
Of course, I know most mothers have questions regarding breast milk and breastfeeding, so below I answer nine of the most common questions I hear about breast milk.
9 Common Questions About Breast Milk
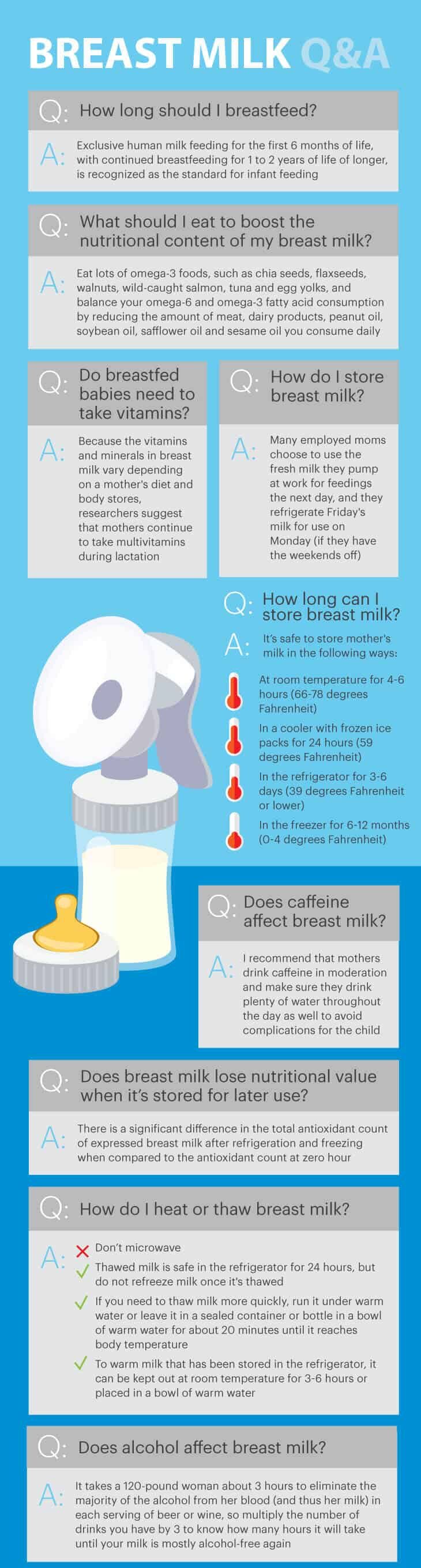
1. How long should I breastfeed?
According to research published in Pediatric Clinics in North America, exclusive human milk feeding for the first six months of life, with continued breastfeeding for one to two years of life or longer, is recognized as the standard for infant feeding.
Another study published by the American Academy of Neurology found that mothers who breastfeed longer may be at a lower risk of developing multiple sclerosis (MS). Researchers found that women who breastfed for greater than or equal to fifteen months were at a reduced risk of multiple sclerosis and its precursor, clinically isolated syndrome (CIS). (2)
2. What should I eat to boost the nutritional content of my breast milk?
Studies have found that the fatty acid profile of breast milk varies in relation to maternal diet, particularly when mothers eat too many omega-6 fatty acids and not enough omega-3 fatty acids. Eat lots of omega-3 foods, such as chia seeds, flaxseeds, walnuts, wild-caught salmon, tuna and egg yolks. Balance your omega-6 and omega-3 fatty acid consumption by reducing the amount of meat, dairy products, peanut oil, soybean oil, safflower oil and sesame oil you consume daily. (3)
3. Do breastfed babies need to take vitamins?
Vitamin K is typically given to newborns in their first days of life, and deficiencies of other vitamins (except vitamin D) are rare, especially if mothers are nourished adequately. Because the vitamins and minerals in breast milk vary depending on a mother’s diet and body stores, researchers suggest that mothers continue to take multivitamins during lactation.
Vitamin D levels are low in breast milk, particularly for moms who get little exposure to sunshine, so pediatricians recommend that breastfed infants are given a liquid vitamin D supplement in order to avoid a vitamin D deficiency. These supplements usually contain large amounts of the water-soluble and fat-soluble vitamins that meet the recommended daily allowances for your baby. (4)
4. How do I store breast milk?
Many mothers pump when they return to work and nurse at night and on the weekends; some decide to exclusively pump too. Many employed moms choose to use the fresh milk they pump at work for feedings the next day, and they refrigerate Friday’s milk for use on Monday (if they have the weekends off).
It’s normal for pumped milk to vary in color, consistency and scent depending on the mother’s diet. You may also notice that stored milk separates into layers, and the cream rises to the top. Before feeding the baby this stored milk, gently swirl the warmed bottle to mix the layers again, but do not shake the bottle.
Small amounts of cooled breast milk can be added to the same refrigerated container throughout the day, but avoid adding warm milk to already cooled milk. When you store milk in the freezer, leave room in the storage bag because liquids expand when frozen, and write the dates on the bags and use the oldest milk first.
5. How long can I store breast milk?
It’s safe to store mother’s milk in the following ways:
- At room temperature for four to six hours (66–78 degrees Fahrenheit)
- In a cooler with frozen ice packs for 24 hours (59 degrees Fahrenheit)
- In the refrigerator for three to six days (39 degrees Fahrenheit or lower)
- In the freezer for six to 12 months (0–4 degrees Fahrenheit)
Storing breast milk this way does not increase the possibility of bacterial contamination and growth of infectious pathogens in stored milk. However, the nutritional value of breast milk may be altered. (5)
Research published in the Archives of Disease in Childhood Fetal and Neonatal Edition indicates that store time should be limited to 48 hours in order to preserve the antioxidant activity of breast milk. Freezing breast milk resulted in a greater decrease of antioxidants than refrigeration. (6)
Researchers in Spain tested refrigerated and frozen breast milk over a 90-day period. They found that by three months from freezing breast milk, there’s a relevant and significant decline in the concentration of fat and energy content. The modification of total nitrogen and lactose was not constant and at lower magnitudes when breast milk was frozen. (7) Based on this research, I suggest that you use your frozen stash of breast milk for emergencies or to use when your baby begins eating solids that supply her with the nutrients she needs. When your baby begins eating a combination of foods at around six months of age, you can add frozen breast milk to smoothies or purees.
Related: The Best Postnatal Vitamins for Mom and Baby
Related: Shatavari: The Ayurvedic Wonder Herb You Need to Know About
6. Does breast milk lose nutritional value when it’s stored for later use?
According to research published in the International Breastfeeding Journal, bottle systems that are used to deliver expressed breast milk may reduce the concentration of vitamin C to less than 40 percent of the recommended daily intake for infant. The study included the analysis of four bottle systems that were sampled after 20 minutes of milk expression. (8)
Research published in the Journal of Health, Population and Nutrition suggests that there’s a significant difference in the total antioxidant count of expressed breast milk after refrigeration and freezing when compared to the antioxidant count at zero hour. This includes a decline in vitamins C, A and E. (9)
7. How do I heat or thaw breast milk?
Do not microwave breast milk. Microwaving breast milk changes its composition, and it can cause severe burns to the baby’s mouth because of hot spots that develop in the milk.
Thawed milk is safe in the refrigerator for 24 hours, but don’t refreeze milk once it’s thawed. If you need to thaw milk more quickly, run it under warm water or leave it in a sealed container or bottle in a bowl of warm water for about 20 minutes until it reaches body temperature.
To warm milk that’s been stored in the refrigerator, it can be kept out at room temperature for three to six hours or placed in a bowl of warm water.
8. Does alcohol affect breast milk?
Most mothers can drink in moderation while breastfeeding. According to La Leche League, it takes a 120-pound woman about three hours to eliminate the majority of the alcohol from her blood (and thus her milk) in each serving of beer or wine, so multiply the number of drinks you have by three to know how many hours it will take until your milk is mostly alcohol-free again. There’s no need to “pump and dump” every time you drink alcohol, as long as you’re able to wait before breastfeeding again.
9. Does caffeine affect breast milk?
A 2012 study published in Pediatrics suggests that caffeine consumption during pregnancy and by nursing mothers does not have consequences on sleep of infants at the age of 3 months. In the study, infants until 3 months of age were unable to metabolize caffeine when mothers drank about three cups of coffee per day. (10, 11) However, other studies show that some infants can be sensitive to caffeine and display increased irritability and sleep disturbances when exposed to caffeine from breast milk. (12)
I recommend that mothers drink caffeine in moderation and make sure they drink plenty of water throughout the day as well — both in order to stay hydrated and avoid caffeine overdose.
Breast Milk Nutrition
The first fluid produced by mothers after delivery is called colostrum. Colostrum is one of the most vital ingredients in breast milk, and it’s what is often referred to as “liquid gold.” It’s a thicker, yellowish breast milk that’s made in the later stages of pregnancy. Colostrum is loaded with nutrients and antibodies to give your baby exactly what she needs in her first days of life. After three days or so, the body naturally begins to make mature milk, which contains an ideal combination of protein, sugar, water and fat. (13)
Mature breast milk contains, on average, 1.1 percent protein, 4.2 percent fat and 7 percent carbohydrate; it supples 72 calories of energy per 100 grams. Fat is the most highly variable macronutrient in milk. Hindmilk, which is the last milk of a feed, may contain two to three times the concentration of milk fat found in foremilk, the initial milk of a feed. This is why mothers are commonly advised to empty an entire breast prior to feeding from the other breast. As hindmilk is more energy-dense due to its higher fat content, this recommendation ensures that the infant’s satiety and energy needs for growth are met.
Antibodies are also a vital part of the mother’s breast milk. Antibodies protect your vulnerable newborn from both viral and bacterial infections. According to a 2002 study published in Breastfeeding Review, infant formula-feeding is inferior to breastfeeding because human milk enhances the immature immunologic system of the infant and strengthens her defense mechanisms against infective and other foreign agents. Researchers indicate that there are bioactive factors in human milk, such as hormones, growth factors and colony-stimulating factors, as well as specific nutrients. Mother’s milk may also reduce the incidence of disease in infancy, and factors in breast milk promote gastrointestinal mucosal maturation, decrease the incidence of infection, alter gut microflora, and have immune-boosting and anti-inflammatory functions. (14)
Breast milk also has antioxidant properties. It contains vitamin C and E and enzymes, including superoxide dismutase, catalase and glutathione peroxidase. Research suggests that all factors, conditions and problems affecting infants, especially those born prematurely, are the outcomes of one unifying disease — oxygen radical disease. If there are too many free radicals produced and too few antioxidants, a condition of oxidative stress develops, which may cause serious damage in infancy. A need to reduce oxidative stress and boost antioxidant defenses in these vulnerable infants is essential. (15)
Breastfeeding also has benefits for mothers. A 30-year study published in 2018 found that lactation for at least six months may lower the risk of diabetes in women. The 30-year study followed 1,238 women, ages 18 to 30 years old, without diabetes who had at least one live birth after 1985–1986. The participants reported how long their lactation period was, and results indicated that women who lactated for six to twelve months or longer had half of the risk of diabetes compared to those who did not breastfeed at all. The study notes that further investigation is needed to explain the correlation of this relationship. (16, 17)
How to Increase Breast Milk Supply
Many mothers fear that they aren’t making enough breast milk for their babies and are looking for natural ways to increase breast milk supply. There are some potential causes of low milk supply that should be addressed before you stress out about taking action to increase your supply (which may already be fine). The golden rule when breastfeeding is that nursing is a supply and demand process. If you’re supplementing with formula, then you won’t make enough breast milk because your body doesn’t know that it’s needed. Scheduled feedings may also interfere with your supply and demand cycle and can lead to a reduced supply, so try to nurse your baby whenever she’s hungry.
To establish your supply when the baby is very young, nurse her about every two hours during the day and every four hours at night, and use both breasts. Frequent feedings ensure that your breasts are stimulated enough to establish a full milk supply. The more milk that’s removed from your breasts, the more milk your body will produce. Supply issues may be caused by the baby not latching properly (which can be due to sleepiness, being used to the bottle or use of nipple shields), so seek advice from a lactation counselor if you think this may be the issue.
Adding pumping sessions after nursing sessions can also be helpful, especially if your baby isn’t eating frequently enough. If you’re working and need to pump milk for your baby, plan to pump your milk two to three times while you’re away from your baby. Each day’s pumping should provide enough milk for the next day’s time at day care or with a sitter.
Galactogogues (like fenugreek, blessed thistle and alfalfa) are used to increase breast milk production, but researchers suggest that this should only be done when all non-pharmacologic recommendations are exhausted. The efficacy and safety data regarding galactogogues use is limited, and more studies are needed to evaluate the herbs’ effects on breast milk production. (18)
The folklore that alcohol consumption enhances milk supply has persisted for centuries, but studies show that this isn’t true. In fact, a study conducted at the Monell Chemical Senses Center in Philadelphia suggests that infants consumed, on average, 23 percent less milk following their mothers’ consumption of alcoholic beer relative to the nonalcoholic beer. This decrease in milk intake was not due to a decrease in the number of times the babies fed but because the babies ingested less milk during each feeding. (19)
Lastly, don’t overlook your own needs — mothers need to eat healthy and nourishing foods (like these superfoods) in order to produce enough breast milk, and they need to hydrate, relax and get enough rest (whenever possible!). Take time for yourself at some point during the day, and be confident in your body and its ability to make what your baby needs in terms of nutrition.
Related: Fenugreek Seeds for Digestion, Metabolic Syndrome & More
Final Thoughts on Breast Milk
- Breast milk is loaded with exactly the right nutrients in the exact amounts a new baby needs.
- Colostrum is loaded with nutrients and antibodies to give your baby exactly what she needs in her first days of life. After three days or so, the body naturally begins to make mature milk, which contains an ideal combination of protein, sugar, water and fat.
- Antibodies are also a vital part of the mother’s breast milk. Antibodies protect your vulnerable newborn from both viral and bacterial infections.
- Breast milk also has antioxidant properties; it contains vitamin C and E and enzymes, including superoxide dismutase, catalase and glutathione peroxidase.
- There are a number of ways to increase breast milk supply naturally, but the golden rule is that nursing is a supply and demand process.
- There are certain rules to follow when pumping and storing expressed milk to ensure that you reduce bacterial growth and maximize the nutritional content in breast milk.










