This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
4 Ways to Get Rid of Tonsillitis
June 18, 2018
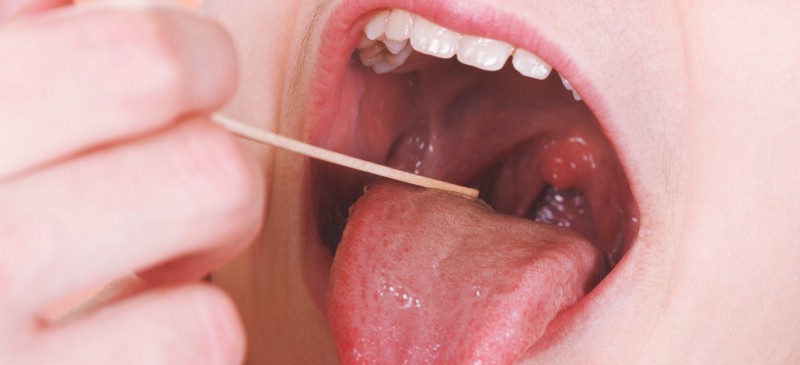
When most people think of tonsillitis, they envision a child with swollen glands who has to get his or her tonsils removed. From there, it’s all visions of ice cream and jello and a reason to miss school while eating dessert for a meal.
The fact is that tonsillitis affects more than just children — and surgery is not (!) always the best course of treatment. This may be a bummer to school kids everywhere looking for an extreme reason to miss school and enjoy their favorite frozen treat, but there are safer, more natural ways to treat tonsillitis.
As with most maladies today, it begins with your diet, along with your lifestyle choices. So what are the symptoms and causes of tonsillitis, and what are the best tonsillitis natural remedies? Let’s dig in!
What Is Tonsillitis?
Acute tonsillitis is an inflammation of the tonsils caused by a virus or bacterial infection. The tonsils are two small, oval-shaped pads located in your throat, which have the important job of blocking bacteria and pathogens from invading the body once they enter through the mouth. Surgery to remove at least part of the tonsils (called a tonsillectomy) is one of the most common procedures during childhood. (1) While tonsillitis and other short-term infections of the tonsils occur most often in children, anyone can be affected by viruses or bacterial infections within the tonsils no matter his or her age.
Tonsillitis can be caused by both viruses and infections that are “bacterial” in nature. The majority of tonsillitis cases are caused by Streptococcus pyogenes, a type of bacterial pathogen. (2) For decades, treatment for sore throats and tonsillitis centered around antibiotics, including penicillin. However, this approach doesn’t always work longterm to solve the underlying problem — especially if the cause is viral — and can also come with some unwanted side effects.
There are all types of bacteria, viruses and fungi present within the throat, including within the tonsils, which belong to the healthy microflora that live within the body. Billions of bacteria populate every part of the body, especially the gut, but normally these bacteria don’t cause any harm. In fact, we need certain types of microbes to help with things like immune responses, digestion, nutrient absorption, weight control and hormonal balance (the kind of bacteria we often call probiotics).
The body doesn’t even respond negatively to all potentially harmful bacteria that are present, as long as they don’t begin rapidly reproducing. For example, studies show that around 10 percent of healthy children have Strepptococcus pyogenes bacteria present within their tonsils at all times but still suffer no health consequences. (3) The trouble begins when “bad bacteria” start to multiply and outnumber beneficial bacteria, leading to infections that can cause pain, swelling and disease-causing inflammation.
The best approach to treating tonsillitis is preventing the inflammation from occurring in the first place or getting worse, while also increasing your immune function through a healthy diet, taking antiviral herbs and avoiding anything that puts extra stress your body. One of the biggest reasons to avoid a tonsillectomy is because your tonsils are key players in keeping you from getting sick; removing the tissue within the throat that captures pathogens means more are likely to make their way further into your system.
Symptoms
Common signs and symptoms of tonsillitis include: (4)
- painful swollen tonsils
- sore throat
- difficulty swallowing normally
- tender lymph nodes on the sides of the throat and neck (which you can usually feel if you apply pressure to this area)
- redness surrounding the tonsils and throat
- fever or chills
- white or yellow coating on the tonsils
- painful blisters or ulcers on the throat
- changes in the ability to talk, loss of voice
- headaches
- loss of appetite, nausea or vomiting
- pain in the ears and neck
- bad breath

Diagnosis
Diagnosis of acute tonsillitis has to come from a doctor, who will likely observe the tonsils and do a swab test (also called a rapid strep test) to look for the presence of bacteria. Tonsillitis can be hard to distinguish from other viral or bacterial infections within the throat, such as a cold or flu, so don’t assume that tonsillitis is the cause of pain right away.
The good news is that tonsillitis is usually obvious, and simply having swollen tonsils that aren’t painful or don’t cause other problems doesn’t mean you need to be treated. This can commonly go away on its own as your body fights off any presence of increased bacteria. (5)
Most cases of swollen tonsils don’t require antibiotics and can clear up if you give it time. One of the problems with diagnosing tonsillitis is that bacteria isn’t always the cause, and viral infections won’t show up on a swab test. If the swab test for bacteria comes up negative but all symptoms of tonsillitis are present, your physician will still likely diagnose tonsillitis. The next step is to appropriately treat the condition — for example, not prescribing antibiotics if a virus is to blame, since antibiotics don’t kill viral infections!
If the infection is viral in nature, you need to fight it off naturally, and even if bacteria is to blame, you can treat it without the inference of antibiotics. (6) You can naturally improve recovery time and help prevent future infections by following the immune-boosting tips below.
Natural Remedies
1. Get Plenty of Rest
When your body’s under stress, you need plenty of downtime to help speed up healing. Prioritize getting good sleep (at least seven to nine hours a night), give yourself a break from the gym or your usual exercise routine for a few days, and do what you can to reduce stress. Any unwanted stress takes away your body’s limited energy, which you want to put toward getting better fast.
2. Naturally Treat Painful Symptoms of the Throat
A swollen, sore throat is very common in people with tonsillitis, so ease the pain by doing what you can at home before turning to prescriptions or even over-the-counter painkillers. Try drinking warm water to help ease discomfort in the throat. Some people also prefer sucking on ice or drinking very cold fluids to soothe swelling, so this is a matter of preference.
Since you’ll likely have trouble swallowing, try eating soft and smooth foods like vegetable juices, fruit smoothies, apple sauce or mashed potatoes, soup (if it’s not too irritating), and yogurt, for example. Drink plenty of fluids to flush out the system and keep hydrated, but be careful of anything irritating like very hot fluids, sugary or acidic drinks, or carbonated beverages.
It also helps to gargle with warm salt water or suck on soothing lozenges, such as natural ones that contain numbing ingredients like fennel/licorice. Licorice root has been used to help treat inflamed or sore throats for centuries, and studies show it’s effective for lowering pain when added to a gargle solution with water. (7)
Gargling often with warm salt water is a good option for anyone who’s 8 or older. You can make your own simple mixture at home by combining on teaspoon (five grams) salt with eight fluid ounces (240 milliliters) of warm water.
Finally, don’t forget that raw honey is an age-old effective treatment for sore throat problems. Raw honey can be mixed with cinnamon or ginger and water, or stirred into soothing herbal tea. Some studies have found that honey has natural inhibitory effects on around 60 different species of bacteria, some species of fungi and viruses too! It can help treat pain and other infection symptoms within the respiratory tract as well as work as a cough medication. (8) Raw honey is also great for speeding up healing since it naturally contains antibacterial and antiviral properties.
If you’re still in a lot of pain, be careful if you choose to take over-the-counter pain relievers, such as acetaminophen or ibuprofen, which can help you sleep and control excess swelling. Many aren’t safe for young children and contain active or extra ingredients that aren’t going to help solve the problem. Don’t use antiseptic mouthwashes, decongestants and antihistamines, which don’t fight the causes of tonsillitis and might even wind up adding more pain.
3. Try Using a Vaporizer or Humidifier
Vaporizers and humidifiers help moisten indoor dry air, which can relieve discomfort and pain in the mouth and throat caused by constantly breathing in treated indoor air. This is especially true in the winter months when we don’t get to spend as much time outdoors, where we’re exposed to fresh air. The cleaner the air you breath, the less swollen your air passages should feel and the quicker your body can recover from infection.
4. Help Your Immune System Become Stronger
The better you take care of yourself in general, the less likely you are to suffer from infections of any kind. One of the best ways to prevent infections and inflammation from occurring anywhere in the body is to eat a nutrient-dense diet that promotes a strong immune system. An anti-inflammatory food-based diet helps keep circulation flowing, allowing the immune system to respond effectively to perceived threats and carry bacteria or viruses from the body more quickly.
Focus on eating a nutrient-dense diet, which means less toxins and chemicals enter your body and put pressure on your lymphatic system. Foods to avoid for optimal immunity include any that upset your digestive, circulatory and immune systems, such as:
- common allergens, like dairy products, gluten, soy, shellfish or nightshades
- low-quality animal products
- crops heavily sprayed with pesticides
- refined vegetable oils
- processed foods that contain chemical toxins, preservatives and artificial ingredients
- high-sugar packaged snacks made with refined and bleached grains
Supply your body with much-needed nutrients and antioxidants, including:
- green leafy vegetables (and other colorful produce)
- cruciferous veggies (broccoli, cabbage, cauliflower, etc.)
- berries
- omega-3 foods, like salmon and wild seafood
- nuts and seeds (chia, flax, hemp, pumpkin, etc.)
- unrefined oils (like extra virgin olive oil and coconut oil)
- herbs and spices (raw honey, ginger, turmeric, garlic, for example)
Certain supplements and essential oils can also be beneficial for reducing swelling in lymph nodes, including the tonsils. These include lemon, myrrh, oregano, cypress and frankincense essential oils, which can be massaged into the throat area when combined with a carrier oil.
Slippery elm, licorice root, marshmallow root, burdock root, sage and echinacea are all natural herbs used for increased wound healing, lowering inflammation, and relieving coughs, sore throats and pain. Slippery elm and marshmallow root, for example, become gel-like when mixed with water and coat the throat to ease discomfort.
These herbal remedies can be found in teas, liquid tinctures or capsules. Try drinking several cups of tea daily or making your own mixture containing 30 to 40 drops of tincture mixed with water.

Causes
The tonsils are considered “guardians” since they’re a part of the immune system, specifically the lymphatic system, and are made up of tissue that acts as a natural germ filter. The tonsils are one of our first lines of defense, since they normally trap germs (bacteria, fungi, viruses, etc.) that make their way into the mouth or nose and threaten the immune system.
They’re responsible for tackling threatening pathogens soon after they enter the body, stopping them from potentially traveling further into the body and causing infections. (9) The production of germ-fighting antibodies is one of the most important roles for the tonsils, since these white blood cells attack bacteria that are deemed dangerous.
Only a portion of the tonsils can be seen when someone opens her mouth, but other parts are situated above the roof of the throat and as far back as the base of the tongue. Together, the different parts of the tonsils form a ring where the mouth and nasal cavity meet the throat (the tonsillar ring), which is located at the perfect spot to intercept viruses or bacteria. Because they always come into contact with outside particles, the tonsils are often inflamed and enlarged, but this doesn’t always signify a problem.
However, when there’s an influx of bacteria or other germs, the tonsils become overworked, very inflamed and infected themselves. This is what causes tonsillitis, which is accompanied by swelling, pain, tenderness and other symptoms common with infections.
Surgery/Antibiotics: Safe or Even Necessary for Tonsillitis?
For years, the first line of defense against tonsillitis (and many other infections, for that matter, such as ear infections like “swimmer’s ear”) was to prescribe antibiotics. However, today we know that frequent use of antibiotics, especially over long periods, increases the risk for antibiotic resistance as well as allergies and other problems.
It’s alarming how many children receive multiple courses of antibiotics before making it to their teenage years, which can unfortunately change the bacterial environment within the gut. Every time you take antibiotics, you essentially kill off “good,” sensitive bacteria in the body in addition to bad bacteria causing infections.
Good bacteria have the important role of reducing and balancing all types of harmful pathogens in the body, so we suffer when populations of these “good bugs” are greatly reduced. If even a small percentage of bad bacteria remain, they can multiply and spread without enough good bacteria present to combat them.
Some experts feel that antibiotics for tonsillitis aren’t appropriate and are overprescribed. According to the Department of Head and Neck Surgery at the University of Munich, “microbiological screening tests in children without symptoms are senseless and do not justify an antibiotic treatment.” Many doctors now encourage patients to think twice about asking for prescription antibiotics since sore throats and other infections are commonly viral in nature (not bacterial infections), which aren’t helped by antibiotics. (10)
Before starting any antibiotic treatment, you want confirmation from your physician that bacterial tonsillitis is definitely the cause of your condition, which can be determined pretty effectively using swabs. Be careful that if a swab test comes back negative, you don’t immediately begin taking antibiotics anyway. In some cases, doctors automatically prescribe antibiotics based on physical symptoms alone and no presence of bacteria, but there’s no guarantee that this even works. (11)
And even when antibiotics are needed to treat acute tonsillitis after trying short-term steroid treatments or over-the-counter painkillers first, antibiotic therapy should only last for as little time as possible, which is just as effective as traditional 10-day therapies. Antibiotics can be given in a single shot or taken for up to 10–20 days by mouth (split into two treatments to kill off the infection), so always take the minimum dose needed.
When it comes to surgery, experts warn that a tonsillectomy (to remove either a part of the tonsils or the whole thing) should be a last-resort treatment option. This is especially true for young children under 6 years old, who should only have a tonsillectomy if they experience reoccurring bacterial tonsillitis that doesn’t respond to other natural or prescription treatments.
Removal of the tonsils — usually done with a scalpel but now also commonly performed with targeted lasers, radio waves, ultrasonic energy or electrocautery to cut, burn or evaporate away parts of the tonsils — can be painful and risky, since it removes lymphatic tissue that is normally protective. Tonsillectomy is a surgery (usually taking about 45 minutes and performed in an outpatient setting) and therefore involves anesthesia, risk for infection, scar-tissue formation or fever, and at least seven to 10 days to rest and recover.
In fact, results of a recent study published in the JAMA: Otolaryngology-Head & Neck Surgery demonstrate that removing the tonsils and/or adenoids can lead to other health problems later in life. In a population-based cohort study of 1,189,061 children born in Denmark between 1979 and 1999, researchers followed the outcomes of children with initial overall similar health who received these surgeries and a control group of children who did not receive the surgeries. The study participants were followed for at least 10 years of their life and up to 30 years, depending on when they joined the study. (12)
Of the participants, 1,157,684 children were in the control group, meaning they did not have any of the surgeries. The remaining children were broken out as follows: 17,460 received an adenoidectomy; 11,830 received a tonsillectomy; and 31,377 received an adenotonsillectomy (both adenoids and tonsils were removed). The researchers found that the participants who had received these surgeries as children experienced a “2- to 3-fold increase in diseases of the upper respiratory tract” and also an increase in “infectious and allergic diseases.” The researchers concluded that these surgeries result in long-term health risks that it’s important to consider this when deciding whether or not to go through with one of these procedures. (12)
The 2011 American Academy of Otolaryngology-Head & Neck Surgery’s “Clinical Practice Guideline: Tonsillectomy in Children” currently recommends diagnosis of recurrent tonsillitis only if seven or more clinical episodes of throat infection occur in the preceding year or 10 or more occur in the two preceding years. However, these guidelines are under review and expected to update in Fall 2018. In all other cases, it’s best to try to solve the problem as naturally as possible before considering even partial removal of the tonsils (called partial tonsillectomy), which has lower risks for side effects and requires less recovery time than full removal. (13, 14)
Final Thoughts
- Acute tonsillitis is an inflammation of the tonsils that may be caused by harmful bacteria or a virus.
- Diagnosis of acute tonsillitis has to come from a doctor, who will likely observe the tonsils and do a swab test (also called a rapid strep test) to look for the presence of bacteria.
- The tonsils are considered “guardians” since they’re a part of the immune system, specifically the lymphatic system, and are made up of tissue that acts as a natural germ filter.
- Experts warn that a tonsillectomy (to remove either a part of the tonsils or the whole thing) should be a last-resort treatment option.
4 Natural Remedies for Tonsillitis
- Get plenty of rest.
- Help treat painful sore throat symptoms by drinking warm water, gargling with warm salt water.
- Use a vaporizer or humidifier.
- Boost your immune system by eating a nutrient-dense diet.
Read Next: Strep Throat Symptoms, Causes & Treatments


