This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
Dry Needling for Muscle Pain & Headache Relief
Reviewed by Ron Torrance, DO, FAOASM
May 22, 2023
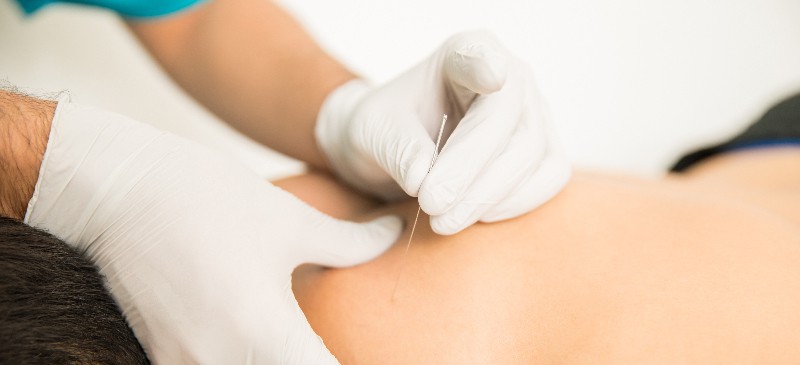
Dry needling is a form of alternative therapy is used to release tight muscle bands that are associated with trigger points — or hard “knots” within a muscle that can cause pain over a large area — with a very thin needle placed in strategic regions of the body by a trained physical therapist, physician or chiropractor.
Sometimes these trigger points (or even muscle spasms) can make it difficult to perform everyday tasks because there is pain every time the area is touched, and the pain can even radiate to nearby areas of the body.
Learn how dry needling works, how it compares to acupuncture and its many uses.
What Is Dry Needling?
Dry needling is a treatment that involves a very thin needle being pushed through the skin in order to stimulate a trigger point. Dry needling involves the insertion of a needle without the use of injection into muscles, ligaments, tendons, subcutaneous fascia and scar tissue, while wet needling involves hollow-bore hypodermic needles that deliver corticosteroids, anesthetics, sclerosants and other agents. Dry needling is also referred to as trigger point dry needling (TDN) and intramuscular manual therapy.
Dry needling is different than acupuncture, which is intended to unblock energy meridians and help create balance within the bodily system. While acupuncture focuses on addressing the flow of energy around the body and bodily organs, dry needling focuses on stimulating a specific trigger point that is leading to pain and disability.
Myofascial trigger points are a common type of pain. The word myofascial means muscle tissue (myo) and the connective tissue in and around it (fascial). These trigger points are usually the result of a muscle injury, such as common running injuries or repetitive strain. “From a pain science perspective, trigger points are constant sources of peripheral nociceptive input leading to peripheral and central sensitization,” according to a study in the Journal of Manual and Manipulative Therapy.
In other words, trigger points are painful when pressed on and can create pain in another area as well, which is called referred pain. It can even generate something called hyperalgesia, which is an increased sensitivity to pain and which is often the result of damage to nociceptors or the peripheral nerves.
For example, trigger points in the muscles of the shoulder, neck and face are a common source of headaches because the trigger point refers pain to the head. According to research published in Current Pain and Headache Reports, muscle overtraining or direct trauma to the muscle can lead to the development of trigger points.
Trigger points can develop during occupational, recreational or sports activities when muscle use exceeds muscle capacity and normal recovery is disturbed. Dry needling differs from other types of physical therapy because it focuses on stimulating these trigger points and releasing the tension in order to alleviate pain.
How Dry Needling Works
The solid filament needle used in dry needling allows the healthcare practitioner (usually a licensed physical therapist) to target tissues that are not manually palpable, such as the subscapularis, iliacus and lateral pterygoid muscles.
Here are the basic steps of deep dry needling therapy:
- When using dry needling techniques for the treatment of trigger points, the physical therapist will palpate the target muscle for a taut band (or area of tense muscles) and identify the hyperirritable spot, thereby confirming the trigger point that needs to be treated.
- The needle is typically in a tube and it is fixed with the non-needling hand against the trigger point using a pincer grip or flat palpation depending on the location and orientation of the muscle. A palpation is when the physical therapist feels with her fingers or hands to pinpoint areas of tenderness. With the needling hand, the needle is gently loosened from the tube and the top of the needle is tapped or flicked by the physical therapist, allowing the needle to penetrate the skin.
- With deep dry needling, the needle is guided toward the trigger point until the physical therapist feels resistance or notices that the patient has a local twitch response. A local twitch response is a spinal cord reflex that creates an involuntary contraction that can be triggered by a snapping palpitation or penetration with a needle. Research shows that the local twitch response is the result of an alleviation or mitigation of some sort. This can be due to a release of immune system related chemicals, inflammation or even spontaneous electrical activity. When the patient has an involuntary twitch response, that suggests that the needle has hit the right spot.
- When the needle has located the trigger point, as suggested by the local twitch response, the physical therapist will focus on this specific area or other neighboring areas by drawing the needle back toward the layer of tissue directly under the skin without taking it out of the skin.
- The needle will then be redirected toward the remaining trigger points until local twitch responses have stopped or the patient can no longer tolerate the needling at that site.
- When the needle is withdrawn from the skin, pressure is then applied directly to the skin over the insertion in order to aid in the prevention of possible swelling or soreness.
During superficial dry needling therapy, the needle is placed just slightly into a muscle in the vicinity of a trigger point, but the local twitch response is not induced. The needle will be kept in place for about 30 seconds and then withdrawn. If the trigger point still appears to be sensitive after the first round, the needle will be placed in the same area again for 2 minutes.
With superficial dry needling, the physical therapist will try to alleviate trigger point sensitivity with these shorter intervals of therapy, repeating this process until he/she notices a difference. Superficial dry needling is the chosen technique for patients who cannot tolerate deep dry needling or who cramp or become stiff easily.

Common Uses
Dry needling involves using a thin filiform needle to penetrate the skin and stimulate underlying myofascial trigger points, muscular and connective tissues in order to relieve pain and movement impairments.
Trigger points have been identified in numerous diagnoses, and dry needling has been used in the following musculoskeletal conditions and other diagnoses:
- shoulder pain (like thoracic outlet syndrome)
- rotator cuff pain
- biceps tendinitis
- iliotibial band syndrome
- Achilles tendinitis
- tendonitis
- low back pain
- tennis elbow
- whiplash or neck pain (or a stiff neck)
- headaches, including migraine and tension headaches
- muscle strains
- hip pain
- temporomandibular pain (TMJ)
- carpal tunnel
- spinal dysfunction
- pelvic pain and other urologic syndromes
- post-herpetic neuralgia
- complex regional pain syndrome
- nocturnal cramps
- phantom pain
- joint dysfunction
This alternative therapy is also used to treat dysfunctions in skeletal muscle, fascia and connective tissue. It reduces and restores impairments of body structure and function, and can lead to improved activity and participation.
Benefits
1. Reduces Pain
Several studies have demonstrated immediate or short-term improvements in pain or disability by targeting trigger points with dry needling.
In a study published in the Journal of Orthopaedic & Sports Physical Therapy, researchers analyzed the results of the best clinical studies that have been conducted thus far to determine whether or not dry needling helps to reduce neck and arm pain, both common areas for trigger point development.
The researchers found that dry needling can be an effective means of pain relief when dealing with myofascial pain syndrome, or the presence of painful trigger points and muscles. When this technique is used by a physical therapist, it serves as a beneficial treatment, especially when used in combination with other techniques such as exercise.
A study published in the American Journal of Physical Medicine and Rehabilitation suggested that dry needling significantly reduced shoulder pain by targeting a trigger point. In the study, 14 patients with bilateral shoulder pain and active myofascial trigger points in the bilateral muscles underwent dry needling therapy on one side and no therapy on the other side, which served as the control.
Dry needling physical therapy increased both active and passive range of motion of shoulder internal rotation, and the pressure pain threshold of the trigger points. Pain intensity of the treated shoulder was significantly reduced as well. The study provides evidence that dry needling a specific myofascial trigger point does reduce pain and sensitivity in that area.
In a 2016 Manual Therapy study, dry needling was used to treat the upper trapezius latent myofascial trigger point, or MTrP — pain in the upper back region — experienced by 60 females. All the participants reported a reduction in pain. As such, some therapists used it in tandem with cupping therapy for pain relief.
2. Alleviates Headache Pain
Dry needling is often used by healthcare providers to relieve symptoms in patients with certain types of headaches, including tension headaches, cervicogenic headache (which begins in the neck typically) and migraines.
A 2021 Physical Therapy study did a systematic review and meta-analysis, including of four high-quality clinical trials. It examined how dry needling affected headache pain intensity and related disability. For patients with tension-type headaches, dry needling “provided significantly greater improvement in related disability in the short term.”
Overall, the synthesis of results demonstrated that dry needling might significantly improve the following: headache frequency, health-related quality of life, trigger point tenderness, and also cervical range of motion in both tension and cervicogenic headaches. More research is needed to show that dry needling can alleviate migraine pain.
3. Improves Movement
Do patients undergoing dry needling therapy, in conjunction with movement-based therapy, experience more fluid movement?
A 2010 case report published in Acupuncture in Medicine treated four international female volleyball athletes during a month-long intense competitive phase with dry needling therapy. Range of motion, strength and pain were assessed before and after treatment and all scores were improved post treatment. The athletes were able to continue with overhead activities, which showed that dry needling did not cause functional weakness and reduced range of motion immediately after treatment.
These cases support the use of dry needling in elite athletes during a competitive phase with short-term pain relief and improved function in shoulder injuries.
4. Speeds Up the Recovery Process, Including from Whiplash
Patients who undergo dry needling therapy experience less pain quickly; in fact, most patients feel the benefits immediately after their first treatment. According to reports published by the Journal of Orthopaedic & Sports Physical Therapy, patient function is restored much more quickly when dry needling is incorporated as part of the total package.
A study conducted at the University of Queensland in Australia investigated the effectiveness of dry needling for chronic whiplash, which is associated with sensory hypersensitivity and has poor responsiveness to physical treatments such as exercise. In order to enhance the treatment outcomes of an exercise intervention, dry needling was used in conjunction with exercise to address the sensory hypersensitivity of whiplash.
Because exercise programs alone did not fully eliminate the symptoms of whiplash after three months of treatment, the physical therapists added dry needling to the treatment plan in order to speed up the healing process, reduce the economic cost of treatment and minimize pain and disability.
Precautions
Dry needling is appropriate for nearly all patients who do not have a significant needle phobia or other anxiety about being treated with needles. Like any type of therapy, dry needling may deliver unintended side effects, such as pain at the stop of needle insertion, muscle soreness, fatigue and bruising. In the hands of a skilled physical therapist, dry needling is a safe and effective treatment option and the patient will see benefits in range of motion and joint use right away.
It’s normal that it may take several dry needling therapy sessions before the muscle is fully functional again. This is because trigger points are located under deep layers of muscles, so it typically takes several sessions for the changes to take full effect. But studies indicate that patients will notice the difference right after each treatment.
Dry needling is also known to be relatively painless. Generally, the needle insertion is not felt and the local twitch response only provokes a very brief pain response, feeling more like a shock or cramping sensation. A local twitch response is a therapeutic response that serves as a sign that the needle has hit the trigger point, so it’s actually a good and desirable reaction.
Caution is warranted with younger patients; based on empirical evidence, dry needling is not recommended for children younger than 12 years of age. If a child is undergoing dry needling, parent and child’s consent is needed and the child should fully understand the procedure before treatment begins.
Final Thoughts
- Dry needling is a common treatment technique in orthopedic manual physical therapy.
- Dry needling involves a very thin needle being pushed through the skin in order to stimulate a trigger point that causes pain and disability.
- During a dry needling session, the needle penetrates the trigger point, which is known when there is a local twitch response. This response suggests that the trigger point is being stimulated and there will be a therapeutic response.
- Dry needling is a safe and effective treatment option for patients who are not afraid of needles.
- Patients who undergo dry needling will see benefits in range of motion and joint use right away. Sometimes several sessions are necessary in order to fully eliminate the trigger point.









