This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
GERD Symptoms & Causes + 5 Natural Treatments
February 16, 2017

Between 20-44 percent of the total population of those living in Western, industrialized nations suffers from GERD. Many experts believe that the alarmingly high prevalence of GERD is a direct result of eating a modern, highly-processed diet. Up to 40 percent of Americans experience GERD-related symptoms at least monthly. Around 10-20 percent experience GERD symptoms almost daily. Worse still, up to 15 percent of GERD patients may wind up developing Barrett’s esophagus syndrome. Severe tissue damage and scarring of the esophagus causes Barrett’s esophagus syndrome. (1) Not surprisingly, studies show that GERD prevalence is much higher in the Western world compared to in Asian countries. Prevalence there is less than 5 percent. (2)
According to recent research, so many people develop GERD likely not just because they have left acid reflux symptoms untreated. For nearly the last 80 years, acid reflux was considered the early stage of GERD. Today experts are turning their attention towards another contributing factor: chronically high inflammation as the actual culprit behind GERD. Inflammation not only contributes to tissue damage in the esophagus. It’s also tied to many other forms of digestive distress.
While this finding is important and changing the way we think about GERD, maybe we shouldn’t be all that surprised. After all, inflammation is at the root of most diseases.
How is GERD treated? The World Journal of Gastrointestinal Pharmacology & Therapeutics states that “Management of GERD may involve lifestyle modification, medical therapy and surgical therapy.” (3) If you’re one of many adults suffering from GERD symptoms (or acid reflux symptoms) like difficulty swallowing, digesting or breathing, you’ll be happy to know there are many effective natural remedies available. These include eating a GERD-healing diet, limiting stress and exercising. These can help bring you relief without the risks associated with long-term medication use.
What Is GERD?
The most common health problems that affect the esophagus are belching (also called eructation), heartburn and conditions related to gastric reflux, including GERD. GERD is short for gastroesophageal reflux disease. It’s commonly called heartburn and it affects the esophagus. Up to 1 in 5 American adult experiences GERD. In severe cases, it can lead to bleeding ulcers in the esophagus. It can also lead to a dangerous condition called Barrett’s esophagus. Barrett’s esophagus is sometimes tied to the formation of cancer in the esophagus.
Experts define gastroesophageal reflux disease (GERD) as “Symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus or beyond, into the oral cavity (including larynx) or lungs.” GERD can be classified as non-erosive reflux disease (NERD) or erosive reflux disease (ERD). Whether or not esophageal mucosal damage is present determines these classifications.
In patients with GERD or acid reflux, usually it’s not that too much stomach acid is causing symptoms. Rather, the acid is in the wrong place. In fact, acid production might be even lower than in healthier people. In healthy adults the part of the esophagus called the esophageal sphincter keeps stomach acid in its proper place. When this “valve” stops working properly (usually because it “relaxes” too much or loses its strength), stomach acid can creep up into the esophagus. The most common GERD or acid reflux symptoms that develop as a result are chest pains, burning sensations and difficulty swallowing.
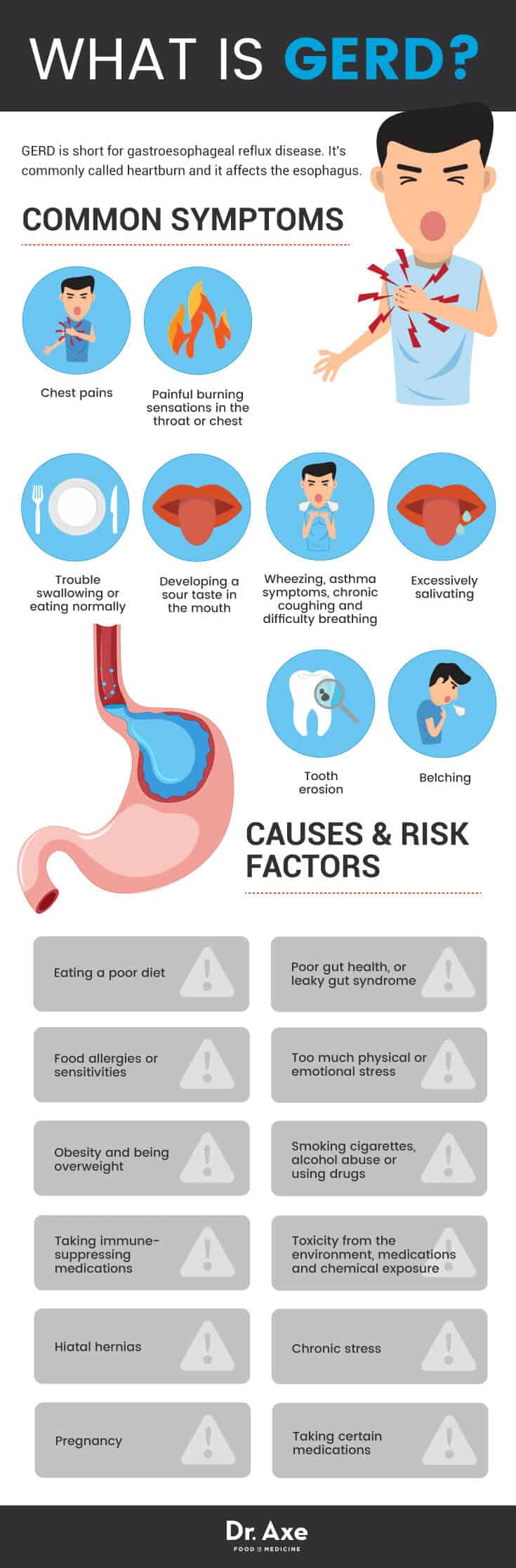
Common Symptoms of GERD
The most common symptoms of GERD include:
- Chest pains
- Painful burning sensations in the throat or chest
- Wheezing, symptoms of asthma, chronic coughing and difficulty breathing (especially during exercise, when sleeping or if you’re also sick)
- Trouble swallowing or eating normally
- Developing a sour taste in the mouth
- Belching, a sometimes painful symptom caused by gas trapped in the upper part of the digestive tract.
- Excessively salivating
- Tooth erosion
Gastroenterologists classify GERD symptoms as either typical or atypical. Most symptoms are strongest after eating. Bigger, fattier meals that consist of processed or acidic foods especially cause symptoms. Typical symptoms include heartburn and acid regurgitation. Atypical symptoms include epigastric pain, dyspepsia, nausea, bloating, and belching. Many secondary symptoms related to GERD can also cause pain or dysfunction in the throat and esophagus. Examples include coughing and asthma. These secondary symptoms seem to affect those with esophageal damage because there are shared nerves that control the cough reflex and esophagus. These shared nerves can become inflamed and damaged over time. Esophageal acid exposure and mucosal damage can trigger reflexes that cause someone to gasp for air, have trouble breathing and other respiratory issues. (4)
If left untreated, GERD can also lead to serious health problems in some cases. Complications include Barrett’s esophagus, an increased risk of esophageal cancer, worsening asthma, ulcers in the esophagus and severe tissue scarring. Experts found that persistent GERD symptoms can take a toll on someone’s quality of life, including both physical and mental health. A high percentage of those with GERD report reduced mental health. This lowered mental health also seems to decrease how well they respond to medications. (5)
GERD vs. Acid Reflux
- Stomach acid creeping up into the esophagus causes acid reflux. Symptoms of acid reflux usually include chest pains, heartburn, a bad taste in the mouth, stomach bloating, gassiness, and difficulty digesting and swallowing properly.
- Acid reflux and GERD have in common many risk factors, including: pregnancy, history of hiatal hernias, obesity, eating an unhealthy diet, older age and an imbalance of stomach acid.
- If you have very frequent or severe heartburn and acid reflux, you have a higher chance of developing GERD
- Natural remedies for acid reflux usually also help lower symptoms of GERD. These include improving your diet, avoiding certain problem foods, reaching a healthier weight, taking helpful supplements and eating smaller, more balanced meals.
So does acid reflux necessarily cause GERD, and if not, then what does? For decades, researchers and doctors have believed that stomach acid traveling up from the stomach and into the esophagus was the cause for burning sensations in the chest and other acid reflux symptoms that led to GERD. Esophageal 24-hour pH monitoring tests have been used to diagnose GERD. These tests determine the total acid contact time in the esophagus, along with measurements of symptoms. The idea is that acid reflux erodes the tissue in the esophagus for a long time before GERD, the more severe condition, develops.
But according to a 2016 study published in the Journal of the American Medical Association, “Studies in animals have challenged the traditional notion that reflux esophagitis develops when esophageal surface epithelial cells are exposed to lethal chemical injury from refluxed acid.” (6) While acid reflux (regurgitation of acid into the esophagus) likely contributes to GERD symptoms, new findings suggest that the root causes of GERD are actually tied to abnormal inflammatory responses. Inflammation develops in the digestive system, including the esophagus, through secretion of proteins such as cytokines, which damage esophagus tissue cells.
There’s also evidence that some patients with GERD don’t experience much acid reflux or even have high levels of acid production. The opposite can be true in some cases; GERD can be present in patients with low acid. One study investigated the cause of GERD symptoms in more than 900 people. Researchers found that in patients with very low total acid levels, only 12 percent of symptoms were associated with acid reflux. Most of the patients with GERD who had low acid levels were female and younger, compared to GERD patients with higher acid levels. (7)
Causes of GERD & Risk Factors
Scientists involved in the JAMA study mentioned above found that when patients with acid reflux discontinue taking their standard proton pump inhibitors treatments, or PPIs, many develop changes in the esophagus. Increased inflammation causes these changes, not just scarring or burns that would be expected from stomach acid. Two weeks after stopping PPI medication, in many patients esophageal acid exposure increased, mucosal impedance decreased and all patients had evidence of esophagitis (caused by inflammation). Stopping PPI medication use was associated with T-lymphocyte inflammation and basal cell and papillary hyperplasia. This suggests that more than simply erosion of the esophagus due to the presence of stomach acid was taking place.
What types of things cause inflammation in the first place? Risk factors for developing high levels of inflammation that can damage the esophagus include:
- Eating a poor diet
- Poor gut health, or leaky gut syndrome
- Food allergies or sensitivities
- Too much physical or emotional stress
- A sedentary lifestyle
- Smoking cigarettes, alcohol abuse or using drugs
- Taking immune-suppressing medications
- Toxicity from the environment, medications and chemical exposure
Other causes and contributing factors of GERD symptoms can include:
- Hiatal hernias. these develop when a portion of the stomach pushes through the diaphragm and into the thoracic cavity, triggering heartburn. It’s believed that around 20 percent of all adults have hiatal hernias, but not all experience symptoms.
- Chronic stress. Stress is believed to play a huge role in GERD. It’s also tied to higher inflammation levels in general.
- Pregnancy. Acid reflux and GERD are more common among pregnant women, since their expanding belly can press against the stomach triggering pain
- Taking certain medications. These include NSAID pain killers, aspirin, steroids, birth control pills or other hormone replacement drugs, nicotine and numerous courses of antibiotics
- Obesity and being overweight
The Trouble With Conventional Treatments For GERD
The majority of healthcare providers typically prescribe several categories of GERD medications to ease patients’ symptoms. Most work by decreasing hydrochloric acid levels, which blocks the effects of acid erosion in the esophagus, but this doesn’t mean they fix the root problem causing symptoms (inflammation, a poor diet, etc.). GERD medications include:
- Antacids, such as the brand Tums, Maalox, Mylanta and Rolaids
- H2 acid blockers, such as Tagamet, Pepcid, Axid and Zantac
- Proton pump inhibitors (PPIs), such as Prilosec, Prevacid and Nexium.
- Athough rarely needed, sometimes anti-reflux surgery is performed.
Once you begin using medications to treat GERD, such as PPIs, chances are your doctor will recommend staying on them for many years. Unfortunately, chronic use of PPIs can disrupt a person’s microbiome. This causes poor gut health, alters the immune system and increases the risk of serious infections like Clostridium difficile. Long-term use of PPIs may even change the pH level in your stomach. These changes may block some of your body’s natural ability to absorb key nutrients and altering the acid/alkaline ratio.

Natural Treatment of GERD Symptoms
1. Follow A GERD Diet
Luckily, many people have success treating GERD through a healthier diet. I recommend everyone with GERD first avoid inflammatory foods. Adopt a diet rich in inflammation-fighting foods before taking prescriptions, especially long-term.
Sensitivities to certain foods — such as dairy, gluten and many synthetic ingredients found in processed foods — can trigger GERD symptoms and inflammation in some patients. There are a number of foods that are likely to make the pain worse. These include: caffeine, chocolate, alcohol, high-sodium foods, very fatty foods, citrus fruits and refined grains. Sometimes spicy foods or food products made with tomatoes, garlic, onions or mint can make pain worse, too. Instead, focus on eating a GERD-friendly diet. Fill up on foods like all sorts of fresh veggies, grass-fed lean meats, healthy fats, like olive or coconut oil, apples, pears, berries, bone broth, nuts, seeds and potentially yogurt, if it doesn’t worsen symptoms.
Other diet-related tips for reducing GERD symptoms include:
- Limit carbonated drinks. These are often sweetened and also contain air, which can make belching or gas pains worse. Some people also feel worse pain when consuming egg whites or whipped cream.
- Eat smaller meals, spread throughout the day
- Slow down when you drink or eat. Chew your food more thoroughly, and drink beverages more slowly. Gulping drinks (especially when carbonated) can make pain worse.
- Don’t chew gum, smoke or use straws. These habits can cause air to be swallowed. The air then enters the digestive system, and often exacerbates symptoms.
- Avoid wearing tight-fitting clothes after eating, which can add pressure to your sensitive digestive system
- Try to give yourself several hours between finishing your last meal and going to sleep for the night. Lying down after eating, or bending over such as to exercise, can worsen GERD symptoms.
- Drink more water. Many find that this helps lower symptoms, especially when water replaces too much caffeine, sugary drinks or alcohol.
2. Manage Stress & Get Enough Rest
Figure out a way you can get a better handle on stress. Try changing your routine in order to feel more relaxed, exercise, meditate or get more rest.
3. Quit Smoking
Smokers have a much higher risk for developing GERD and other inflammatory conditions compared to non-smokers.
4. Get Regular Exercise & Maintain A Healthier Weight
Research suggests there’s a link between obesity and GERD. Inflammation levels are a bigger problem in those who live a sedentary lifestyle, especially if they consume a poor diet. If you’re overweight, work on making lifestyle changes. Try switching your diet to one focused on whole foods. Also try getting more exercise, limiting stress and balancing hormones in other ways.
5. Talk To Your Doctor About Your Medications
Stopping the use of certain medications, such as NSAIDs if taken in high amounts, or hormone replacement drugs, may help. Speak with your doctor about whether any medications or even over-the-counter drugs might be making your symptoms worse. Also, discuss options about what to do instead.
Precautions When Treating GERD
Monitor your symptoms carefully to determine which factors might be triggering your pain and discomfort. If symptoms interfere with your lifestyle or daily activity, and last for more than two weeks, definitely consider visiting a doctor. See a doctor even if you choose to make lifestyle changes. Other reasons to get a professional opinion on treatment options include: severe hoarseness; worsening of asthma after meals; pain that’s persistent when lying down and interferes with sleep; pain following exercise; difficulty breathing that occurs mainly at night; and trouble swallowing for more than one to two days. You also may want to get tested for H. pylori infection. You also may want to discuss various causes of inflammation or sensitivities with your doctor to determine if these are further triggering your symptoms.
Final Thoughts On Treating GERD Symptoms
- GERD is a common digestive problem that causes damage to the esophagus and symptoms such as heartburn or chest pains. Complications are also possible, including scarring in the esophagus and even cancer in some cases.
- Adopting a GERD diet and making lifestyle changes such as eating anti-inflammatory foods, losing weight and quitting smoking can go a long way in easing GERD symptoms.
- Although PPI drugs do work well for people with GERD, they do come with potential side effects. These include an increased risk of heart disease and digestive infections.
