This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
Diagnosing & Effectively Treating Body Dysmorphic Disorder
August 1, 2018
Having a “positive body image” generally means that someone has comprised a sense of self-acceptance, is realistic about the goals concerning appearance, and feels comfortable in their own skin. People with a positive body image can accurately depict how others see their body — and although they might make ongoing efforts to eat well, exercise and take care of themselves — their control over their appearance is not the most important aspect of their sense-of-self.
On the other hand, those with a “negative body image” — including people with body dysmorphic disorder (BDD) and other eating/body image disorders, such as anorexia or binge eating disorder — tend to place greater emphasis on how they look. Most people without any body distortions have have a body image that fall somewhere in between these two descriptions, and one that also might change frequently depending on their circumstances.
However, people with BDD tend to be very fixated on their shortcomings, unhappy with what they see in the mirror no matter what, and very susceptible to influence from peers, the media, critical family members and others who contribute to low self-esteem.
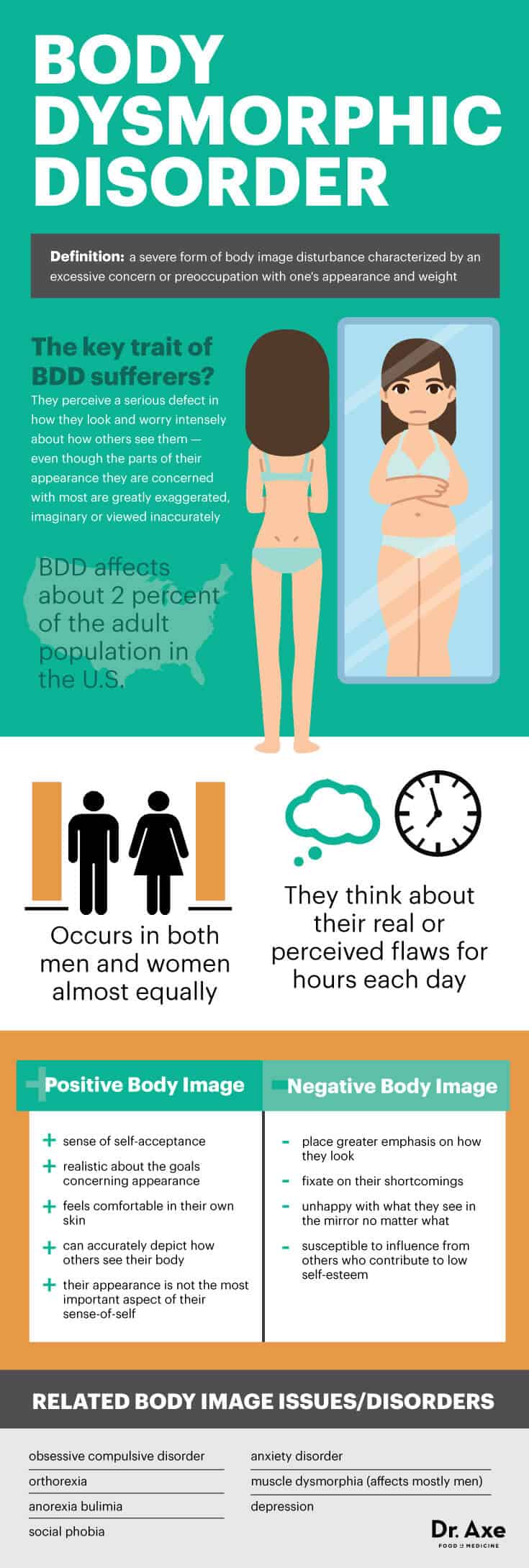
According to the Anxiety and Depression Association of America, “people who have body dysmorphic disorder think about their real or perceived flaws for hours each day.” (1) BDD affects about 2 percent of the adult population in the U.S., and somewhat surprisingly tends to occur in both men and women almost equally. Some of the most promising ways to treat BDD include CBT therapy, meditation, stress reduction, and support from family and friends.
What Is Body Dysmorphic Disorder?
Body Dysmorphic Disorder (BDD) is defined as a severe form of body image disturbance characterized by an excessive concern or preoccupation with one’s appearance and weight. People who struggle with BDD perceive a serious defect in how they look and worry intensely about how others see them — even though the parts of their appearance they are concerned with most are greatly exaggerated, imaginary or viewed inaccurately.
Although most people associate eating disorders and body image issues as typically being “women’s problems,” symptoms of BDD affect both men and women. Men who struggle with BDD typically have “muscle dysmorphia” and worry about things like their muscle mass, height and masculinity.
BDD has many things in common with obsessive compulsive disorder and even orthorexia, or obsessed with eating the right foods. The Body Dysmorphic Foundation lists hallmark symptoms of BDD to include intense anxiety and feelings of distress over “problematic” body parts, social isolation, obsessive thinking, and exhibiting very controlling behaviors. (2) Experts believe that body dysmorphic disorder is one of the most common psychiatric illnesses that overlaps with other psychological disorders, especially eating disorders including anorexia nervosa and bulimia. BDD often “coexists” with anorexia, has many of the same underlying causes, and contributes to the same behaviors and medically related symptoms.
BDD is also considered to be a type of social phobia and anxiety disorder, since it revolves around consistent, out-of-control fear in regards to being judged badly by others. Those with BDD greatly try to avoid being criticized, scrutinized, feeling vulnerable, or being embarrassed and humiliated in social situations. Because fear over weight gain or other body changes is the underlying cause of distress associated with BDD, it’s common for people with BDD to withdraw socially, avoid situations that are unfamiliar or feel out of control, and respond very emotionally to any sense of social criticism.
Signs and Symptoms
People with body dysmorphia, also sometimes called body distortion, typically place great importance on their looks but have less appreciation for other aspects of their lives including their personality, talents, abilities, relationships and strengths. Most have a negative view of themselves and struggle to let their guard down. They often have a strong misconception about their shape and size, and see their flaws as threats standing in the way of forming meaningful relationships with others.
Common signs and symptoms of body dysmorphic disorder include:
- Having intense, recoccuring thoughts and impulses regarding one’s body appearance, or certain features of one’s body or face
- Seeing certain body parts as being disproportionate and inadequate (for example, the stomach or thighs as being big, or muscles being too small in men)
- Overly focusing on any perceived flaw in one’s facial features, skin, height, hair or clothing (for example, having intense anxiety over acne, wrinkles, thinning hair, scars or facial asymmetry)
- Missing work or school and other social situations out of fear others will notice one’s flaws
- Feeling anxious over one’s food choices, exercise routine and surroundings. This can include excessive exercise for weight loss or for muscle gains
- Increased irritability and judgement of others
- Experiencing relationship problems, jealousy, greatly seeking approval from others and needing reassurance
- Social withdrawal and increased time spent alone
- Symptoms of social phobia, or social anxiety, including severe blushing, sweating, shuddering, shyness, trembling or nausea when around others
- Behaviors associated with binge eating and yo-yo dieting, including changes in eating patterns or frequently dieting and even entering into starvation mode
- Symptoms of Obsessive Compulsive Disorder (OCD) including following strict rituals, feeling scared over changing repetitive behaviors (including eating or exercise behaviors), and feeling distressed over a lack or control or when one’s schedule is changed
- Obsessively checking one self in the mirror, applying makeup, grooming and trying to alter one’s appearance, often with with cosmetic/plastic surgeries (3)
- Symptoms of depression, including fatigue, lack of pleasure, reduced motivation, insomnia or sleeping excessively, and suicidal thoughts
- Other physical symptoms of anxiety, including lightheadedness, dizziness, trouble sleeping, digestive problems, shortness of breath and panic attacks, hyperactivity, and impulsivity
Causes
Like other body image issues, forms of social phobia and eating disorders, there isn’t just one single cause of BDD. Genetic factors, someone’s upbringing, the media, bullying from peers or family, and coexisting mental disorders all contribute to body distortion.
Research shows that neurobiological factors — such as malfunctioning of serotonin in the brain, personality traits and traumatic life experiences — can all be causal factors.
Who’s at risk for BDD the most?
- Those with any form of eating disorder, especially anorexia, which causes an intense fear over weight gain. (4) Bulimia is also likely to coexist with BDD, and the frequent use of “purging behaviors” associated with bulimia nervosa, such as using laxatives or vomiting can contribute to water retention and food cravings that spark even more anxiety over body image.
- Adolescents are the most likely to develop BDD, but middle-aged adults also suffer.
- Those with other psychiatric illnesses, including anxiety, depression, bipolar disorder, avoidant personality disorder and obsessive compulsive disorder.
- People who tend to have personalities that are very rigid, pervasive, controlling, inflexible and critical. These types of character traits can contribute to harsh self-criticism, social withdrawal and negative changes in thoughts/behaviors/interactions that cause relationship problems with others.
- People who weight themselves often or who are exposed to frequent “weigh-ins,” especially those done in public settings, such as in gym class or by team coaches.
- Anyone who has experienced sexual abuse, physical abuse, recent trauma or suffers from post-traumatic stress disorder (PTSD). (5) PTSD is a severe form of anxiety that develops after a very traumatic emotional event which can cause social withdrawal, depression, shame, insecurity, mood swings and trouble relating to others.
- Those who have substance abuse problems, including alcohol, marijuana, prescriptions or other illegal drugs.
- People who abuse “weight loss drugs,” herbs, laxatives, teas or medications in hopes of quickly losing weight.
- People with attention deficit hyperactivity disorder (ADHD). ADHD can increase social anxiety and restlessness, and recent research has shown that girls with ADHD are 2.7 times more likely to develop eating disorders than girls without. (6)
- There are even certain medical disorders that might seem unrelated to body issue concerns, but can raise the risk for BDD and other body image issues. These include diabetes, Irritable Bowel Disease, Irritable Bowel Syndrome (IBS) and thyroid disorders. The reason these have some overlap with BDD is that they tend to cause increased focus on body weight changes and often require strict dietary changes, which can increase anxiety over food choices and potential weight gain.
Natural Treatments
1. Identify Co-Existing Disorders
BDD is considered to be a severe disorder, and professional treatment is always recommended. There is plenty that someone struggling with BDD can do on their own to improve recovery and manage symptoms, but seeing a therapist is still encouraged.
Because body dysmorphic disorder coexists with many other psychiatric illnesses and sometimes even other medical problems, so it’s important to visit a professional for a physical exam and psychiatric evaluation. More often than not, other abnormal behaviors can be identified by a therapist or doctor, including anxiety, depression, substance abuse, excessive exercise and insomnia. Determining what other disorders accompany BDD is the first step to treating its underlying causes and establishing priorities for treatment to reduce symptoms.
2. Become Educated on Early Warning Sides & Symptoms
Recognizing when healthy eating, self-improvement, and exercise patterns start to turn into obsessions is an important step for anyone with a history of body image issues, plus their family members and close friends. Strict rituals around weight and appearance usually take form gradually, so intercepting them early on when they start to cause anxiety is the best way to prevent them from worsening.
Family and friends should be cognizant of signs of body dysmorphic disorder, which typically emerge in the early teenage years. BDD affects both males and females, but sometimes in different ways. Women are more likely to obsess over their weight, skin, hair, clothing and facial features, while men might develop an obsession that their build is too small or not muscular enough (muscle dysmorphia). (7)

3. Cognitive Behavioral Therapy (CBT) & Other Forms of Therapy
According to a 2004 report in the Official Journal of The World Psychiatric Association, “The psychosocial treatment of choice [for BDD] is cognitive behavioral therapy, consisting of elements such as exposure, response prevention, behavioral experiments, and cognitive restructuring”. (8) CBT is a form of psychotherapy that emphasizes the importance of underlying thoughts in determining how we feel and act.
Through working with a CBT therapist, someone with BDD can uncover thought/behavior patterns that make anxiety, self-criticism and social withdrawal worse. CBT is also used in the treatment of body image issues to reduce repetitive behaviors (such as mirror checking and excessive grooming).
One study done by Massachusetts General Hospital found that after patients received four weeks of daily individual 90-minute CBT sessions (20 total sessions), BDD symptom severity significantly decreased (9). In another small study, patients who received thirty 90-minute sessions, plus six months of relapse prevention, showed significant improvements in quality of life that was maintained for at least two years (10).
4. Reduce Stress & Try Mindfulness Meditation
High amounts of stress and anxiety can be trigger for body image issues and body distortion. Meditation and other “mind-body” practices can help increase self-esteem, self-worth and self-compassion, which are important for preventing body image issues and anxiety.
Mindfulness works similarly to CBT in that it helps increase self-awareness and identify underlying thoughts and limiting self-beliefs that might be contributing to BDD. Certain studies have found evidence supporting the effectiveness of mindful eating programs and mindfulness-based interventions for the treatment of various eating disorders, symptoms of body dissatisfaction and social anxiety. (11, 12)
Other effective ways to relieve stress and social anxiety include:
- Doing something creative and fun for a period of time each day
- Joining a support group online or in person
- Trying yoga, Tai Chi or other mind-body exercises
- Branching out to try new activities, join a team or volunteer
- Writing in a journal. This can include making a “values list” of traits that are important for well-being beyond appearance
- Spending more time outdoors in nature, including earthing
- Regularly exercising
- Practicing deep breathing
- Practicing prayer and other forms of spirituality that can increase a sense of connectedness and purpose
- Fostering relationships with supportive people (studies find our relationships are one of the things that make us happiest)
5. Stick to a Balanced, Nourishing Diet
For people with BDD whose symptoms are mostly related to their body weight, it’s crucial to learn to set realistic goals for what it means to eat a healthy diet and maintain a healthy BMI. A nutritionist and/or therapist can help someone with BDD to create a balanced dietary plan that includes enough energy (calories), nutrients and meets their needs overall while considering their unique body shape and size.
Learning “intuitive eating” or mindful eating are two approaches to achieving sustainable healthy eating and body acceptance. Intuitive eaters believe that blame over flaws regarding someone’s appearance shouldn’t be put on person suffering, but instead on the flawed process of achieving perfection portrayed by the media and of dieting.
The goal is to maintain a way of eating that supports a healthier relationship with food and focuses on health holistically, both physically and mentally. Studies show that intuitive eating/mindful eating offer a “realistic alternative to address overweight and obesity than conventional weight-loss treatments”. (13)
Things That Can Make It Worse
According to an article published by The Guardian, some behaviors that have been shown to make BDD and body image issues worse include: (14)
- Comparing your appearance to others
- Yo-yo, crash dieting or fad-dieting
- N0t having strong social support
- Over-exercising, or feeling pressure from a coach or team to weigh a certain amount
- Bullying from peers or bullying via social media
- Feeling anxious over changes experienced during puberty or college (such as gaining “the freshman 15”)
- Having poor social skills and coping abilities during stressful times
- Teasing over body and appearance in school and from siblings
- Coming from a family with a history of obesity, which can increase anxiety over weight
- Coming from a family with a history of eating disorders or body image issues
If you’re helping a friend or family member to overcome body dysmorphic disorder or another type of body image issues, keep in mind that some behaviors and comments might actually make things worse. Criticizing someone’s diet, exercise, appearance, facial features or clothing can increase anxiety over their appearance.
Parents that encourage fad-dieting, compare their children’s appearance to others, emphasize the importance of accomplishments, and show a lot of interest in celebrities and the media might all contribute to BDD thoughts and behaviors.
Things that parents or family members can do to help someone deal with BDD include:
- Avoiding critical body talk and teasing
- Setting good examples of what it means to eat and exercise healthfully
- Having open communication about tough feelings and stressful events
- Encouraging healthy socializing and teaching appropriate social skills
- Expressing gratitude
- Acknowledging accomplishments that have nothing to do with appearance
- Giving family members privacy, teaching self-trust and respecting boundaries
Facts and Statistics
- Surveys show that around 43 percent of men and 56 percent of women experience dissatisfaction with their overall appearance. Studies show that severe appearance/body dissatisfaction, enough to be diagnosed as BDD, affects between 1.5–4 percent of the total population. (15)
- Around 13 percent of people being treated for other eating disorders report having BDD symptoms.
- BDD usually emerges during adolescents; research shows that around 70 percent of cases begin before the age of 18.
- BDD has been to be more than twice as common as OCD and more common than many other mental disorders, including social phobia, simple phobia, generalized anxiety disorder and bulimia nervosa. (16)
- It’s believed that between 8–37 percent of patients with OCD, 13 percent of those with social phobia, and up to 40 percent percent of those with major depression have BDD.
- A high proportion of people with BDD tend to seek “non-psychiatric medical or surgical treatments” to improve their appearance. In a study of 250 individuals with BDD, 76 percent had sought and 66 percent had received dermatologic treatment and plastic surgery for correcting perceived flaws. In dermatology settings, around 12 percent of all patients screened positive for BDD, and in cosmetic surgery settings, up to 15 percent have reported BDD symptoms.
- In 83 percent of BDD patients who had procedures to change their appearance, the treatment had no positive effects on BDD symptoms or made symptoms worse. Twenty-six percent report having multiple procedures and 76 percent are strongly dissatisfied with their results.
Final Thoughts
- Body dysmorphic disorder (BDD) is a form of body image distortion that causes anxiety over how a person appears to others
- Coexisting disorders include social anxiety, eating disorders, depression, PTSD, substance abuse and OCD
- Symptoms of BDD include frequent body checking or weighing, dieting, ritualistic behaviors, cosmetic or plastic surgeries, social isolation and problems maintaining relationships
5 Treatments for BDD
- Professional therapy (CBT)
- Stress reduction
- Mindfulness meditation
- Getting social support
- Working with a dietitian to establish a healthy eating plan
Read Next: Eating Too Little & Exercising Too Much? Risks of Female Athlete Triad



