This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
Ease Lichen Planus Discomfort: 9 Natural Treatments
February 6, 2018

If you have a rash with red, purple or bluish lesions that itches and spreads, you may have lichen planus. This disease is triggered by the immune system in response to stress, allergens or a viral infection. It may affect the skin, scalp and nails, as well as the mouth and the genitals. Discomfort can range from mild to severe, and effective lichen planus treatments help to relieve the symptoms and facilitate healing. (1)
As stated by the American Academy of Dermatology (AAD), while the rash is unsightly and uncomfortable, this condition is not considered serious, nor is it contagious. It can develop in one or more locations on the body. (2) The medical community estimates it affects 0.1 percent to 4 percent of the general population, primarily between the ages of 30 and 60. As a matter of fact, lichen planus affects both men and women, but it most often occurs in women during perimenopause. (3)
What Is Lichen Planus?
There is widespread disagreement whether lichen planus is an autoimmune disease or the body’s natural reaction to an allergen. Regardless of how it is classified, the result is an aggressive and uncomfortable rash that can affect virtually every part of the body. Lichen planus that affects the skin is also known as cutaneous lichen planus. However, some individuals may only experience oral lichen planus. (4) It’s important to see your health care professional for a proper diagnosis since there are a few different types, plus sometimes lichen planus may resemble other conditions such as pityriasis lichenoides.
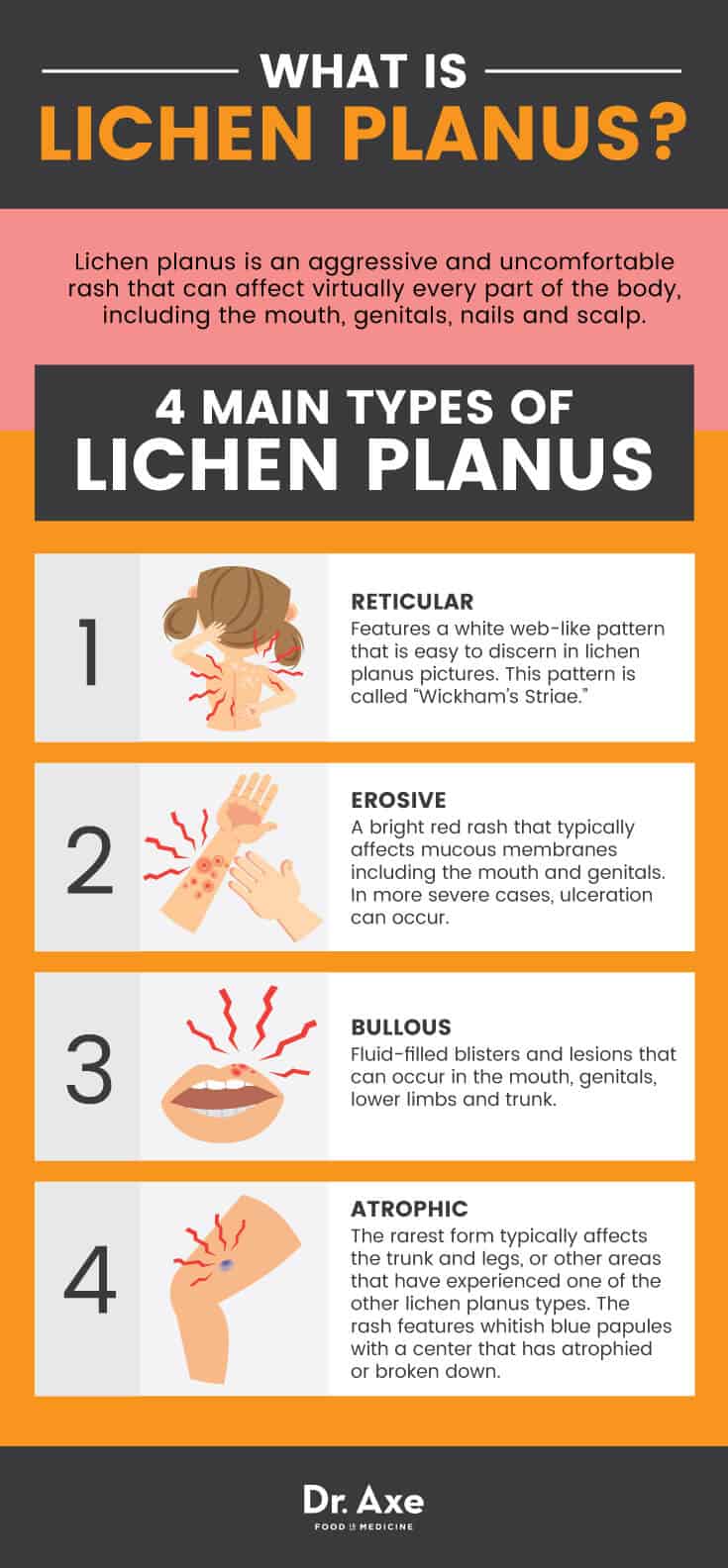
4 Main Types of Lichen Planus
- Reticular: Features a white web-like pattern that is easy to discern in lichen planus pictures. This pattern is called “Wickham’s Striae.”
- Erosive: A bright red rash that typically affects mucous membranes including the mouth and genitals. In more severe cases, ulceration can occur.
- Bullous: Fluid-filled blisters and lesions that can occur in the mouth, genitals, lower limbs and trunk.
- Atrophic: The rarest form typically affects the trunk and legs, or other areas that have experienced one of the other lichen planus types. The rash features whitish blue papules with a center that has atrophied or broken down. (5)
If the rash is bright red and affects the gums, cheek or tongue, then it is erosive lichen planus. With erosive lichen planus, most people experience moderate to severe discomfort while eating and drinking. Common irritants include acidic and spicy foods, and both extreme hot and extreme cold can worsen the pain.
A bullous lichen planus outbreak is identified by fluid-filled blisters and lesions that can appear in the mouth, on the scalp, in and around the genitals, and on the skin and nails. They are most common in the lower limbs and mouth.
Atrophic lichen planus is the rarest form of lichen planus. In this type of cutaneous lichen planus, papules most commonly appear on the trunk or legs. It can also affect other areas that have had previous lichen planus outbreaks. The hallmark of this type is that the rash features tissue that has atrophied or broken down in the center of whitish blue papules.
Oral Lichen Planus
When lichen planus develops in the mouth, expect moderate to severe discomfort. Spicy foods and acidic foods may worsen the discomfort and some individuals may find that icy foods or drinks or extremely hot foods or drinks may cause further distress. In more severe cases of oral lichen planus, the discomfort may be constant and unrelenting.
Reticular is the most common type to appear in the mouth; however erosive, bullous and atrophic types can also appear. With reticular, the inside of the cheeks will have the iconic white web-like pattern while with erosive lichen planus, the gums, cheeks or tongue will appear bright red and inflamed. (6) Also, fluid-filled lesions and blisters of bullous lichen planus can appear on the cheeks, tongue, roof of the mouth and gums.
Lichen Planus of the Genitals
In fact, the four types of lichen planus described above do commonly develop in and around the genitals. In men, rashes appear around the glands of the penis, or the shaft. For women, it can affect the skin around the genitals, as well as the vulva and vagina. Some studies indicate that up to 50 percent of women with oral lichen planus also have it in the genital region, yet it remains undiagnosed. (7)
Lichen Planus of the Nails and Scalp
Lichen planus can also appear on both fingernails and toenails. For some individuals, it may only involve one or two nails. For others, it may affect all of the nails, causing temporary or permanent damage to the nail. When a rash appears on the scalp (known as lichen planopilaris), it may cause permanent scarring leading to alopecia or hair loss. (8)
Signs & Symptoms
Many physicians use the six “Ps” to describe lichen planus shape and characteristics:
- Planar (flat-topped)
- Purple
- Polygonal
- Pruritic
- Papules
- Plaques
The first sign may be the appearance of a reticular rash on the wrist, trunk, or legs. However, it can begin anywhere on the body. Other indications of this condition include:
- The appearance of purplish-colored lesions or bumps
- The appearance of whitish-blue colored fluid-filled blisters or lesions that burst and scab over
- Thin white lines that create a web-like look that appear over a red rash of small lesions
- Moderate to severe itching on skin rashes
- The appearance of Wickham’s Striae in the mouth accompanied by a burning sensation and changes in taste
- Nails that have a white chalky appearance, ridges, grooving or are splitting
- Itching and pain on the scalp when accompanied by a rash
- An odd odor coming from a rash, even after cleansing
- Vaginal discharge, burning, itching and painful intercourse
- Lesions or blisters on the penis or shaft, chronic itching and painful intercourse
Lichen Planus Risk Factors
While no single, definitive cause has been determined, many medical conditions and environmental factors are believed to play a role.
- Genetics: Your risk for developing lichen planus is greater if a member of your immediate family has been diagnosed.
- Hepatitis C: Research has found a statistically significant association between hepatitis C and lichen planus as well as with a rarer form known as lichen planus pigmentosus. (9, 10)
- Allergens: Exposure to allergens including certain artificial dyes and chemicals may cause an outbreak.
- Medications: Certain medications containing arsenic, bismuth, gold or quinidine, including antibiotics, diuretics, medications for diabetes, malaria, high blood pressure and heart disease. (11, 12) A drug that causes a lichen planus eruption is known as a lichenoid drug.
- Bone marrow transplant recipient (13)
- Age: It is most common in middle-aged adults; perimenopausal women seem to be at a greater risk than other healthy members of the population.
- Amalgam Fillings: Fillings may act as an allergen leading to the development of oral lichen planus.
Conventional Treatment
If you believe you have lichen planus of any type, consult with your physician immediately, as it may be a sign of a more serious underlying condition. If you have oral lichen planus, your doctor or dentist may biopsy certain areas of the rash, take cultures, test you for hepatitis C, and conduct allergy tests to narrow down the lichen planus causes.
In cases where it is caused by certain medications, your physician may take you off the medication, and often symptoms will go away. The same is true when a filling causes oral lichen planus; when the fillings are removed, often the painful rash will go away on its own.
While there is no cure, common conventional treatments include (14):
- Corticosteroids (topical, oral, or injection) to reduce inflammation.
- Antihistamines to reduce itching, inflammation, and general discomfort.
- Prescription medications to suppress the immune system.
- Retinoid drugs commonly used for acne.
- Photo chemotherapy light treatment (PUVA).
- Mouthwashes containing lidocaine.
- Pain medications.
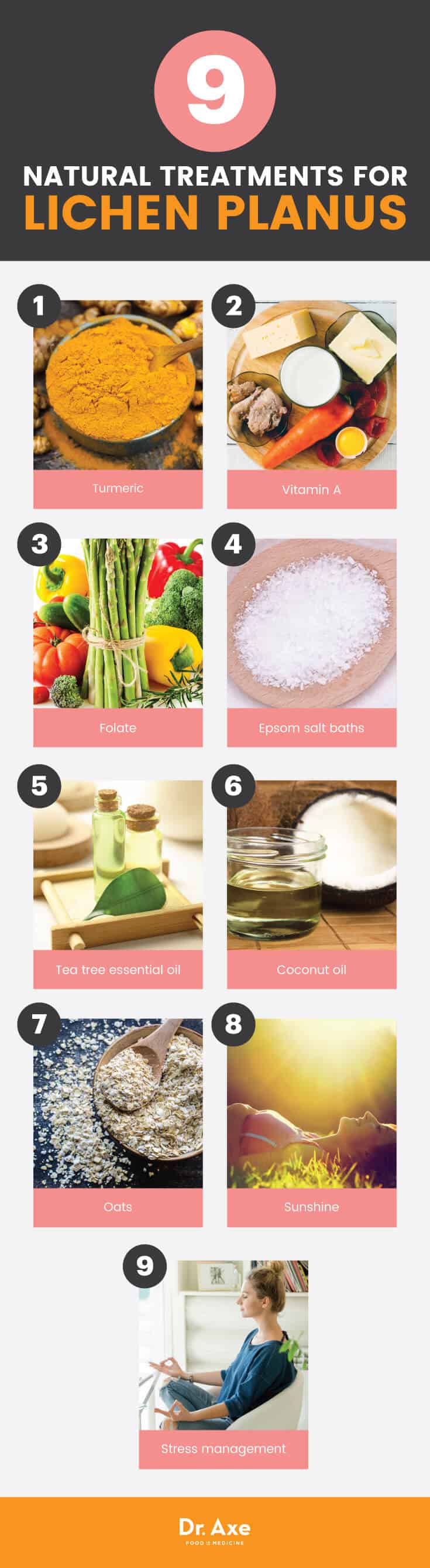
9 Natural Treatments for Lichen Planus
1. Turmeric
A turmeric ointment may be beneficial in changing the appearance and discomfort in oral lichen planus, according to a study published in the National Journal of Maxillofacial Surgery. While this pilot study was small, the researchers believe that the anti-inflammatory, antiviral and antibacterial properties of curcumin can also help to inhibit the growth of squamous cell carcinoma of the head and neck, a recognized risk of oral lichen planus. (15)
Turmeric’s benefits are well-documented and research has shown its ability to control inflammation and reduce pain, two of the symptoms that are conventionally treated with corticosteroids, antihistamines, and prescription pain medications. When taking a supplement, be sure to select one that contains piperine, as it dramatically improves the absorption of turmeric.
To soothe the itching and discomfort on your skin, try a turmeric face mask, but please be careful as it will stain your clothing and skin if left on too long. Turmeric tea may help to promote healing while soothing the pain and discomfort.
2. Vitamin A
As noted above, conventional treatments often include the use of retinoid-based drugs to help relieve many of the symptoms. In addition, according to the University of Maryland Medical Center, vitamin A helps keep skin and mucous membranes healthy. (16) As lichen planus targets these two systems, increasing your intake of vitamin A may help.
During an outbreak, eat more vitamin A rich foods including beef liver from grass-fed cows, raw carrots, sweet potatoes, kale, spinach and winter squash. In addition to treating the rash, vitamin A supports the immune system and fights inflammation, two of the pieces of the puzzle to fight lichen planus.
3. Folate
Researchers from the Department of Oral Medicine, Chulalongkorn University in Thailand found that 44 percent of the patients in the study who had oral lichen planus were folate deficient. The researchers recommended daily supplements. Interestingly, the same group had normal levels of B12 in their system. (17)
People at risk for folate deficiency include those with liver disease and people on certain medications, including diuretics and those used to treat diabetes. As mentioned above, liver disease, diuretics and diabetes medications can increase your risk of developing this disease. A treatment plan should include folate rich foods from the legumes family including garbanzo beans, pinto beans and lentils, as well as beets, asparagus, avocados and beef liver.
4. Epsom Salt Baths
Used for generations to relieve sore muscles and detox the body, Epsom salt can provide relief. It is known for helping to reduce stress, eliminate toxins and reduce pain and inflammation. Prepare a warm bath, and add 2 cups of Epsom salt, stirring it around with your arm. Soak at least 30 minutes for best results. Also, the addition of your favorite essential oils can provide additional relief.
5. Tea Tree Oil
Tea tree oil’s benefits are well known. When treating lichen planus on the scalp, my recipe for itchy scalp shampoo may provide some relief. In fact, the central ingredients of tea tree oil, coconut oil, aloe vera, apple cider vinegar and raw honey have antibacterial, antifungal and antiviral properties. Plus, they work to relieve the itching commonly associated with this condition.
If you have oral lichen planus, a tea tree oil based mouthwash may aid in the healing, particularly with erosive and bullous types. However, for some, it may further irritate the mouth, and cause greater pain; discontinue use immediately if you experience discomfort.
6. Coconut Oil
For oral lichen planus, coconut pulling twice a day may improve the symptoms and provide relief. The process helps to detoxify your mouth by literally sucking out the toxins. Benefits include killing bad breath, soothing a dry mouth, reducing inflammation, and boosting the immune system.
When lichen planus is present on the skin, applying coconut oil to affected areas can help minimize the itching, burning sensation, and pain. Apply several times a day, or as desired.
7. Oats
Natural beauty treatments often include oats as a gentle exfoliator and skin soother. As the lesions and blisters transform through the course of the disease, sloughing off the dead skin can relieve itching, and improve the appearance. Mix one part oats to one part raw yogurt and let stand at room temperature for 20 minutes and then mix in a quarter part raw honey. Spread liberally over affected areas, and allow to set for 10 to 15 minutes. Rinse thoroughly with warm water, and pat dry.
8. Sunshine
One of the conventional treatments mentioned above — photochemotherapy light treatment — is effective in treating this condition. However, side effects can occur, and the ongoing treatments can be challenging to keep up with. (18)
In addition to treating a vitamin D deficiency, getting direct, unprotected sun exposure, can speed healing and provide relief. Make it a priority while you have lichen planus to spend at least 15 minutes each day, in direct sunlight — without sunscreen. Optimal exposure times are in the middle of the day. So when possible, roll up your sleeves or pant legs, and expose the affected area during this period.
9. Manage Stress
According to the Mayo Clinic, stress complicates the symptoms associated with this disease and can trigger recurrences. (19) To help ease stress, do activities that soothe your mind and your spirit. For example, guided meditation, yoga and other natural stress relievers can all be incorporated into your daily routine.
Precautions
While lichen planus is not considered a “serious” disease, it is linked to several types of cancer. For example, women who have lichen planus in the vulva or vagina have an increased risk of developing vulvar cancer, a cancer that typically presents no symptoms. That is why it is essential that women who are diagnosed with lichen planus of the vagina or vulva get examined twice a year. (20, 21)
Lichen planus also increases your risk of developing squamous cell carcinoma, which can be mistaken for bullous lichen planus by the untrained eye. Have your physician evaluate ANY changes in the appearance or texture of a lichen planus rash immediately. Left untreated, squamous cell carcinoma can spread causing serious and potentially life-threatening complications. (22, 23, 24)
The World Health Organization actually defines oral lichen planus as a “precancerous condition” because it is associated with an increased risk of oral cancer. (25) According to researchers, years after the signs and symptoms have gone away, cancer can still appear. As with vulvar cancer, the symptoms of oral cancer can be mistaken for a new outbreak of lichen planus; this is why it is essential that after diagnosis you have regular checkups with your dentist.
Key Points
- Many health care professionals do not consider Lichen planus a serious disease; however, the World Health Organization’s definition should stress that proper treatment and ongoing care is vital.
- Lichen planus complications include oral cancer, vulvar cancer, squamous cell carcinoma and penile cancer.
- Women diagnosed with oral lichen planus must schedule a vaginal examination as 50 percent of women also have the rash near their genitals as well, increasing the risk for vulvar cancer.
- Stress is not believed to cause lichen planus. However, it can cause a recurrence and make the symptoms worse.
- There is no cure; treatments focus on relieving the discomfort, and for some people, the rash will disappear on its own after months or even years.
- If a medication is causing it, cease the medication immediately.
- Because smoking and drinking create a greater risk for developing oral cancer, quit smoking immediately and limit alcohol consumption.
- If an allergen is causing it, avoid the allergen.
- ANY changes in the color or texture of the lesions or blisters, as well as spreading to another part of the body, should be evaluated by a physician immediately.
9 Natural Treatments to Help Ease Lichen Planus Symptoms
- Turmeric ointment
- Vitamin A-rich foods
- Folate-rich foods and supplements
- Epsom salt baths
- Tea tree oil
- Coconut oil pulling for oral lichen planus and coconut oil treatments for lichen planus of the skin
- Oats, used in natural skin treatments
- Vitamin D supplements or exposure to 15 minutes of sunlight each day (with no sunscreen)
- Stress management



