This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
Lyme Disease Symptoms & Causes to Watch Out For (Plus, Promising News About a New Lyme Test)
October 11, 2016
Lyme disease symptoms can mimic many other diseases, making a swift diagnosis difficult. That’s problematic, as rates of Lyme disease are on the rise.
That’s why news of an upcoming new test to detect the disease is such a positive development. In October 2018, researchers confirmed they developed a test that will actually detect Lyme DNA, not just antibodies associated with the disease. According to a study published in Clinical Infectious Diseases, this new testing technique will detect Lyme disease bacteria weeks sooner than current tests, allowing patients to start treatment sooner.
As it stands with current antibody-based Lyme testing, a person would have to be infected for approximately three or more weeks before the test would register as positive for Lyme disease. And not to mention these tests are often criticized for missing a significant number of cases, too.
“These direct tests are needed because you can get Lyme disease more than once, features are often non-diagnostic and the current standard FDA-approved tests cannot distinguish an active, ongoing infection from a past cured one,” Steven Schutzer, MD, a physician-scientist at Rutgers New Jersey Medical School, said in a statement. “The problem is worsening because Lyme disease has increased in numbers to 300,000 per year in the United States and is spreading across the country and world.”
The newly developed testing methods are more exact. Dr. Schutzer and his team say it would not be surprising to see these DNA-based direct tests for Lyme disease approved for use. (I’ll be sure to provide an update once these tests become mainstream and available.)
But back to Lyme disease facts. (They aren’t pretty and they’re only getting worse, thanks to climate change health threats.)
Today, Lyme disease is considered to be the most common tickborne infectious disease in the U.S. In 2013, federal health departments reported 27,203 confirmed cases and another 9,104 probable cases of Lyme disease in the U.S alone. (The real infection rate is believe to be much higher.)
Experts believe that diagnosis is more common today due to growing infection rates and greater awareness and better diagnostic tools. (1) Most people know Lyme disease as an infection or autoimmune disease that is caused by deer ticks.
That’s true, but there’s more to the story. Not all ticks are infected and not everyone who gets bitten by a tick carrying the bacteria that causes Lyme will react the same way. Research shows that tick infection rates vary from 0 to 70 percent even within the same region.
Beyond that, patients experience a wide range of symptoms once infected. This means that individual responses play an important role in the prevention as well as the natural treatment of Lyme disease. Add to that the fact that the standard test available to screen for the disease miss up to 35 percent of cases and it’s easy to see why Lyme is such a complicated topic.
What Is Lyme Disease?

Lyme disease is a chronic condition caused when someone develops an immune reaction to a type of bacteria that’s passed through tick and possibly insect bites. Deer ticks (also called Ixodes ticks) and black-legged ticks carry something called spirochete, which is a corkscrew-shaped bacterium called Borrelia burgdorferi — and these are the two types of insects that spread Lyme disease most often. (2)
In February of 2016, however, the CDC, along with the Mayo Clinic and health officials across Minnesota, Wisconsin and North Dakota, announced the discovery a new species of bacteria called Borrelia mayonii that also caused Lyme disease in people.
Additionally, deer ticks also spread the related but more severe Powassan virus. It’s not just a tickborne disease, either, as experts suspect that certain spiders, fleas and mosquitoes could also potentially carry and spread the disease. (3)
Once the tick or insect bites someone, it transmits the bacteria into the bloodstream. This usually causes a host of autoimmune-like symptoms within several months — including fatigue, fever, headaches and sometimes a rash. Early disseminated Lyme disease occurs when the bacteria that caused this condition spreads throughout the body, which can happen days, weeks or even months after the infected tick bites the individual.
In fact, the real risk associated with Lyme disease is leaving it untreated for many years, which can cause complications that affect the vital organs, blood vessels and the entire immune system.
The U.S. Centers for Disease Control and Prevention (CDC) warns that untreated Lyme disease can lead to serious infections, degeneration of the joints and symptoms of arthritis. CDC also notes left untreated, Lyme can cause heart and blood vessel complications, nerve damage and various other problems of the endocrine and central nervous systems. (4a) In other words, Lyme symptoms go far beyond achy joints.
Dr. Richard Ostfeld wrote a book in 2010 entitled “Lyme Disease: The Ecology of a Complex System,” which was the first book to challenge the idea that Lyme disease is closely linked to the abundance of deer. Rather, he uses Lyme disease as a model system for understanding many other emerging infectious diseases, such as West Nile virus, hantavirus disease and even SARS. (4b)
Lyme Disease Symptoms
The Lyme Disease Organization— a group created to support advocacy, research and education about the disease — conducted a survey looking at Lyme disease symptoms in more than 5,000 people with Lyme disease. The group found that 74 percent experienced at least one symptom they would consider to be “severe.” On average, three severe or very severe symptoms were present at any given time. (5)
Symptoms of Lyme disease are somewhat different during the early stages of the disease compared to the later stages when it is considered “chronic.” Experts created a lengthy list of common symptoms that people can use as a helpful “Lyme disease checklist” if they suspect they might have been infected.
The most common symptoms and signs of Lyme disease include:
- A characteristic “butterfly” skin rash that appears where the tick bite occurred (called erythema migrans or EM rashes). Many develop an EM rash shaped like a bull’s-eye that appears as a red ring around a clear area with a red center. This is considered characteristic of Lyme disease but often doesn’t always develop. In some cases, other rashes appear instead. Some even resemble a spider bite. A recent CDC report on Lyme disease found that about 70 percent of those infected show a visible rash, while other studies show the range to be between 30 to 80 percent.
- Flu-like symptoms, especially shortly after being infected. These include a fever, trouble sleeping, neck pain, fatigue, chills, sweats and muscle aches
- Poor sleep, chronic fatigue and lethargy
- Digestive issues including nausea and loss of appetite
- Achy joint and joint pain. The CDC found that about 30 percent of Lyme patients develop symptoms of arthritis (6)
- Long term, maybe people experience mood changes, including depression and anxiety
- Cognitive changes are also a long-term symptom and include forgetfulness, headaches, brain-fog, misplacing things and trouble concentrating.
Lyme Disease Complications
When Lyme isn’t treated early on (which happens far too often because Lyme disease symptoms mimic other conditions), or when it’s not properly managed, it can sometimes wind up causing permanent damage and complications. Like other infectious or autoimmune diseases, Lyme disease is capable of spreading to just about every part of the body.
Physicians sometimes describe patients who have symptoms for 6 months or more even after receiving treatment for Lyme disease as having “post-treatment Lyme disease syndrome,” or (PTLDS). Other people call this “chronic Lyme disease” or post Lyme disease syndrome (PLDS).
Some of these patients do not test positive for having an active infection, which leads some experts to question whether or not Lyme is truly the cause of their ongoing symptoms. Other experts believe that Lyme causes complications when the body starts attacking itself, a characteristic of an autoimmune disorder. (7)
There is still some controversy over how to best treat Lyme disease patients who don’t get better after receiving initial treatment (usually antibiotics). The CDC states that “studies do not show patients who receive prolonged courses of antibiotics do better in the long run than patients treated with placebo”. (8)
Still, many Lyme patients will tell you longer-term antibiotic treatment helped save their lives. Regardless, it’s important that patients with chronic Lyme include certain lifestyle changes as part of managing their symptoms. This includes things such as improving immunity, eating a nutrient-dense diet, staying active and limiting toxin exposure.
What Causes Lyme Disease?
Most people get Lyme disease from a tick bite, especially immature ticks (called nymphs) which are very tiny. In this stage, the tick is about the size of a poppy seed and hard to feel or see. These types of tick bites are usually painless unnoticeable, which unfortunately means that the tick can stay on the skin for hours (or even days!) without the person even realizing it. The longer a tick or insect stays attached to the skin, the more likely it will be to transmit the bacteria that causes Lyme disease. This is why it’s crucial to check your skin after you’ve spent time in high risk areas. Interestingly, putting your clothing in the washer/dryer and getting a shower immediately after spending time outside can significantly lower your risk of getting Lyme disease. (9)
Another way that people can become infected with the Borrelia burgdorferi bacteria is by inheriting it from their mother. If pregnant women are infected, they are capable of passing on Lyme disease to their unborn children. It’s still debated whether other forms of physical contact can cause human-to-human transmission, such as sex or blood exposure. It’s possible that Lyme disease can be spread in these ways just like other serious infections/viruses are, such as hepatitis or HIV/AIDS. Still, little is known for certain as of now, and so far research doesn’t show it’s likely. (10)
People living on the East Coast in American get Lyme disease more than those in the middle of the country or living on the West Coast, but this doesn’t mean they are the only ones at risk. According to the Lyme Disease Organization, Lyme disease has been transmitted all across the United States as well as in more than sixty other countries. In fact, Lyme disease has been found on every continent except Antarctica.
People who spend a lot of time outdoors or who live in coastal areas are at the greatest risk due to the higher population of bacteria-carrying insects. On the East Coast, deer ticks are more likely to infect people, while on the West Coast black-legged ticks are more often to blame. Studies have found that residents of the coastal Northeast, Northwest California and the Great Lakes region are at the highest risk. (11)
Each Person’s Reaction to Lyme Disease Is Different
Although Lyme disease is transmitted through bites, it affects each person differently depending on the state of their current health and strength of their immune system. There are thousands of people living today who have been bitten by vectors capable of causing Lyme disease, yet they show no symptoms. To some extent, every person’s body is home to viruses, bad bacteria, fungus and cancer cells. So what’s really important is building a strong immune system to keep these invaders at bay.
Someone may be more susceptible to experiencing severe symptoms of Lyme disease if they are experiencing:
- Weakened immunity
- Inhibited cellular function and protection
- Systemic bacterial infections (including tick co-infections)
- Environmental factors, including exposure to mold and parasites
Facts & Numbers About Lyme Disease
- Up to 300,000 Americans are diagnosed with Lyme disease every year, according to research from the CDC. Lyme is often under-diagnosed and under-reported, so many experts believe the number of infected is actually much higher.
- Lyme disease affects 1.5 times more people than breast cancer does each year. It also affects six times as many people in the U.S. compared to the HIV/AIDS.
- Children, adults and older people can all get Lyme disease, but it affects people with lower immune function most, especially young children between the ages of 5 and 10. About 25 percent of patients with Lyme disease are children in this age group.
- People who spend a lot of time outdoors (especially in the woods) are most likely to get infected, including firefighters, park rangers and people who regularly camp or hunt. Studies show adults between the ages of 40 and 55 are diagnosed most often, especially males in this age range (12). Still, it’s important to note you can contract Lyme disease even in your own yard.
- June, July and August are the three months when Lyme disease is believed to be transmitted most due to more people spending time outdoors (13)
- 75 percent of people with Lyme disease experience severe symptoms. On average, people experience three or more symptoms that are considered “severe”
- Tick bites that transmit Lyme disease can be very hard to catch; only about 25 percent of patients who develop Lyme disease recall getting bitten
- The risk of getting Lyme disease is often reflected in risk maps. However, only about 10 percent of reportable Lyme cases are currently captured in these maps.
- Lyme disease can cause long-term complications when untreated. Sixty to 70 percent of patients with chronic Lyme disease experience cognitive impairments, fatigue, muscle and joint pains, depression and trouble sleeping.
Conventional Medicine vs. Natural Treatment for Lyme Disease
How Is Lyme Disease Diagnosed?
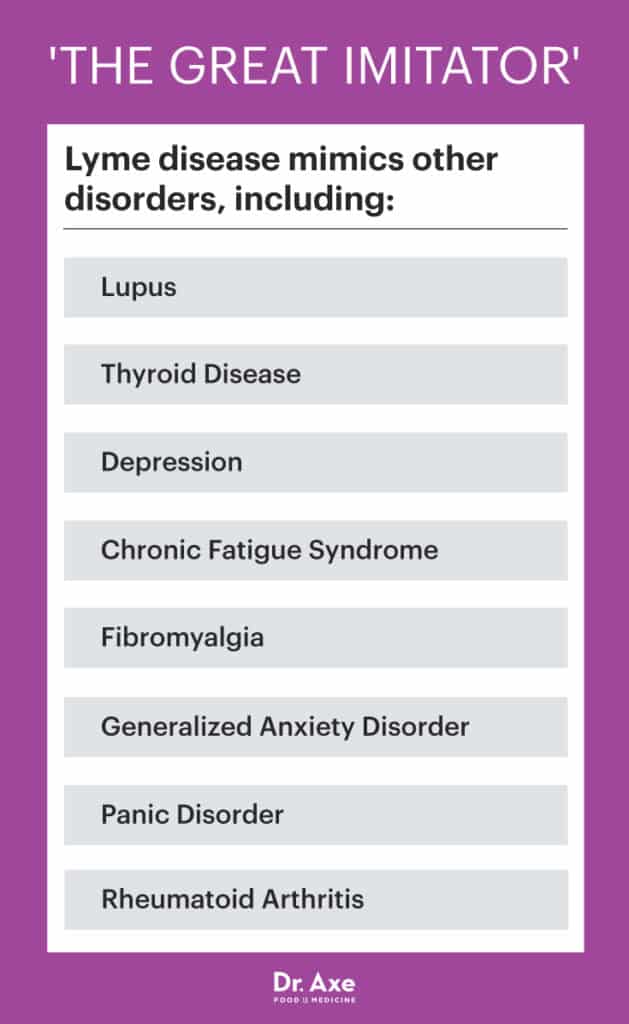
Lyme disease can be difficult to properly diagnose since many of its symptoms closely mimic other health problems and common autoimmune disorders, including thyroid disorders, fibromyalgia, depression, lupus or rheumatoid arthritis. In fact, Lyme is called “The Great Imitator” for this reason. Doctors often rely on a blood test and/or the appearance of a skin rash to make a diagnoses of Lyme disease, which is why many cases are initially missed. Laboratory testing misses a large percentage of Lyme cases, so groups like the International Lyme and Associated Diseases Society recommends other diagnostic and treatment guidelines.
Conventional Medicine for Lyme Disease
Doctors most often treat Lyme disease by giving patients antibiotics which are taken over the course of several weeks. Depending on someone’s symptoms, other medications like NSAIDs, corticosteroids and painkillers might be used to control pain and inflammation. The CDC reports that: “Patients treated with appropriate antibiotics in the early stages of Lyme disease usually recover rapidly and completely. Antibiotics commonly used for oral treatment include doxycycline, amoxicillin, or cefuroxime axetil. Patients with certain neurological or cardiac forms of illness may require intravenous treatment with drugs such as ceftriaxone or penicillin.”
Although these medications can help many people to overcome Lyme disease, these prescriptions don’t always work. Long-term antibiotic treatments for Lyme disease have reportedly helped many people recover, but they have also been associated with serious complications and don’t always seem to resolve symptoms better then placebo. That’s why I’m a strong supporter of focusing on completely improving your immune system when it comes to taking on Lyme disease. Side effects of common Lyme disease medications may include:
- digestive issues and appetite loss
- seizures
- dangerous blood pressure drops
- chronic symptoms of mental fogginess, poor memory
- chronic fatigue
- body numbness and pain
- even death in rare cases (14)
Natural Treatment of Lyme Disease
When it comes to managing Lyme disease, first and foremost prevention is very important. Steps you can take to to prevent getting Lyme disease include:
- Using a natural bug spray or insect repellent
- Performing daily tick checks. Ticks attach anywhere but particularly like spots like the back of your knee, around waistbands, under armpits or any other constricted place. Anytime after you have been in tick habitat you should thoroughly check your entire body and remove attached ticks immediately. Once attached, ticks do not wash off in the shower, the University of Rhode Island TickEncounter Resource Center notes. (15)
- After spending time outside, particularly in areas with high grass, around wood piles or in the woods, throw your clothing into the washer/dryer immediately. (The dryer actually kills ticks by drying them out.) Getting out of your clothing quickly and performing a tick check is a great way to avoid tick attachment.
- Improving overall immune strength so that if you do get bit, you have the best chance of having a minimal reaction.
Globally, experts are also trying to prevent Lyme disease infections from increasing by reducing tick habitats and coming up with more effective ways to stop the bacteria from spreading. This is especially important considering the fact that research shows ticks and mosquitoes can also transmit other harmful diseases besides Lyme disease.
The Importance of Improving Immune Function
As mentioned above, maintaining a strong immune system is critical for overcoming Lyme disease. Many symptoms of Lyme are caused by an immune response in the body, which means the state of your immune system determines how intense symptoms will be.
Some of the ways you can naturally help to prevent and treat Lyme disease by improving your overall immunity and health include:
- Treating allergies or other illnesses that might be contributing to your symptoms: It’s possible that Lyme disease is not the only thing affecting your health.
- Tracking your symptoms: Get to know the things causing symptom flair-ups. These can include a lack of sleep, infections, stressful events and eating a poor diet.
- Eating an anti-inflammatory diet. Foods that can help keep inflammation down and boost immune function include fresh vegetables and fruits, bone broth, wild-caught fish and other “clean” sources of protein, probiotic foods and healthy fats like coconut oil, nuts, seeds and avocado.
- Taking supplements: Immune-boosting mushrooms including cordycep, reishi and maitake mushrooms have been proven to activate your immune response; vitamin D is important for immune health; omega-3 fish oils lower inflammation and adaptogen herbs can help you deal with stress.
- Getting plenty of rest: Lyme can contribute to fatigue and require that you get extra sleep, so balance activity with rest.
- Reducing emotional stress: Stress weakens the immune system and makes complications more likely. Reach out to family and friends for support and practice stress-relieving techniques regularly like deep breathing, meditation, journaling, reading and exercising.
Final Thoughts on Lyme Disease Symptoms & Causes:
- Lyme disease is caused by an immune reaction following a certain type of tick or insect bite.
- Not every person reacts to Lyme disease the same way; each individual’s immune response determines how severe their symptoms are and how long they last.
- Lyme disease symptoms include fatigue, muscle aches, joint pains, digestive issues and skin rashes, among many other things.
- Lyme disease is often treated with antibiotics, however natural treatments and lifestyle changes such as eating an anti-inflammatory diet, limiting toxin exposure and boosting immunity can all greatly help and should be part of any treatment program.
