This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
Pellagra (+ 5 Natural Ways to Treat Niacin Deficiency)
May 21, 2018
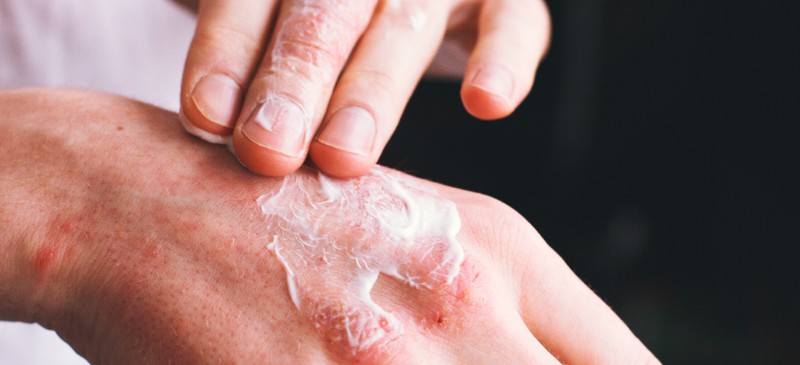
Pellagra is niacin deficiency. This means your body doesn’t have enough niacin or is unable to use the niacin it does have. Niacin is a B vitamin that is essential for your health. Pellagra may also develop if you do not have enough tryptophan in the diet.
In most cases, pellagra is easily reversed with a simple dietary supplement. Left untreated, however, the deficiency can be deadly. Read on to find out the key symptoms of pellagra as well as multiple ways to naturally treat niacin deficiency and its symptoms.
What Is Pellagra?
Pellagra is a condition that develops when the body doesn’t have enough niacin (a B vitamin) or tryptophan. Tryptophan helps the body process and use niacin.
- In some cases, the deficiency develops because someone doesn’t have enough niacin or tryptophan in their diet. This is called primary pellagra.
- In other cases, pellagra occurs when there may be enough niacin in the diet but the body cannot use it for some reason. This is called secondary pellagra.
Although niacin deficiency may start with subtle symptoms that can be easily confused with many other disorders, it can progress to very noticeable and even deadly symptoms. The most visible sign of pellagra is its characteristic dermatitis.
Most cases of pellagra can be cured with proper treatment of the deficiency and any related problems causing the condition. However, some people have lasting problems from the deficiency, including de-pigmented skin or neurological problems.
Pellagra is mostly found in adults. It is rare in children and infants, even in developing countries. The condition is quite rare among people of any age in the United States. As a deficiency, it is not contagious. The deficiency can usually be diagnosed through blood or urine tests and a physical exam.
In most cases, pellagra can be prevented by a well-balanced diet with sufficient calories, a diet high in protein or taking niacin supplements. For people with secondary pellagra, prevention can usually be managed by taking supplements or getting proper treatment for the underlying condition to prevent the body from being unable to process niacin.
Signs & Symptoms
The classic collection of pellagra symptoms is known as the “3 Ds,” and they usually happen in this order: diarrhea, dermatitis and dementia. If left untreated, a fourth “D” can occur: death.
More broadly, signs and symptoms of pellagra may include: (1, 2, 3)
- Gastrointestinal issues
- Diarrhea
- Poor appetite
- Pain in the belly
- Nausea or vomiting
- Trouble eating or drinking
- Malnutrition
- Indigestion
- Skin problems
- Reddened or brownish-red skin
- Scaly or flaky skin in areas exposed to sun, heat or friction, as with a bad sunburn
- Rash with a clear edge
- Symmetrical rash or markings on each side of the body
- Itching or burning
- Thick, hard, cracked or bleeding skin after time
- Rash anywhere on the body but often the hands, arms, fee and lower legs, face and neck
- Sore or inflamed mucous membranes (lips, tongue and gums)
- Canker sores
- Swollen mouth
- Bright red tongue
- Neurological changes
- Confusion or disorientation
- Apathy
- Depression (usually mild) or anxiety
- Irritability
- Headache
- Memory loss
- Restlessness
- Tremors
- Delusions or psychosis
- Stupor, coma or death (in severe, untreated cases)
Do not attempt to self-diagnose pellagra. The gastrointestinal symptoms of niacin deficiency can be easily confused or co-occurring with those of Crohn’s disease and ulcerative colitis, especially since these conditions have related issues with absorbing nutrients. In addition, pellagra rash can easily be confused with other kinds and causes of skin problems, such as eczema.

Causes & Risk Factors
The cause of pellagra depends on what type you have.
For people with primary pellagra, the cause is a lack of niacin (also called vitamin B3 or nicotinic acid) or tryptophan in the diet. Risk factors include:
- A diet low in niacin and/or tryptophan
- Anorexia and malnutrition
- Living in a developing country
- A diet heavy in corn that is not treated with lime water
Secondary pellagra is caused by problems that prevent the body from absorbing or using niacin. Causes include: (1, 4)
- Alcoholism
- Cirrhosis of the liver
- Chronic diarrhea
- Gastrointestinal diseases such as Crohn’s disease, ulcerative colitis and GI tuberculosis
- Problems metabolizing tryptophan, such as Hartnup syndrome
- Carcinoid tumors
- Certain medications, including azathioprine and isoniazid
Risk factors for secondary pellagra include: (4)
- Long-term alcoholism
- Following food fads or dramatically restricting calories
- Dependency on illegal drugs
- Malabsorption problems caused by other diseases
- Poor diet
- A diet heavy in corn that is not treated with limewater
Conventional Treatment
Pellagra treatment typically includes correcting the deficiency. Most often, treatments include:
- Niacin or nicotinamide taken as oral supplements or into the vein (IV)
- A high-protein diet plus supplement prescriptions to correct other deficiencies
- B vitamins with high amounts of niacin
- Thiamine and pyridoxine plus niacin for people with chronic alcoholism (which can mean a thiamine deficiency)
- Bed rest for severe cases
You may also receive treatment for related symptoms or for conditions causing secondary pellagra. Treatments will depend on your symptoms and underlying conditions and may include:
- Skin lotions, creams or oils
- Antimicrobial ointments to help fight skin infection
- Sunscreen and sun protection
- Canker sore ointment
- A change in medications for health problems such as HIV
- Assistance quitting drug or alcohol dependency
- Referral to a psychologist or neurologist for other complications
- Liquid or semisolid diet for people with difficulty eating due to mucous membrane irritation
Natural Remedies
Cases of primary pellagra can usually be treated with simple and natural therapies. Cases of secondary pellagra should be carefully monitored by a health care professional due to the involvement of other health conditions. In either case, do not attempt to treat pellagra at home without first getting a formal diagnosis and consultation with a medical professional.
Natural treatment options include:
1. Take a niacin supplement
Treatment of primary pellagra usually requires just a niacin supplement. In many cases, secondary pellagra is also treated with a niacin supplement, but you may also require treatment for the condition causing your deficiency.
Most adults require only 14 to 16 milligrams of niacin per day. Pregnant or breastfeeding women may need 17 to 18 milligrams daily. Supplements for treatment often range from about 20 to 30 milligrams per day. The Mayo Clinic considers niacin supplements a generally safe natural therapy. (5, 6)
Although your doctor should recommend the proper dose, you can expect to take less than 2,000 milligrams per day. Even at levels of 100 milligrams per day, your doctor may recommend periodic tests to check liver function.
You may notice skin flushing or a rash on your face or upper body shortly after taking your supplement. This is called “niacin flush” and is usually harmless and temporary. In many cases, you will stop getting the flush after taking niacin on a regular basis. You can also ask about a flush-free form of nicotinic acid or nicotinamide if you are bothered by the flushing.
Do not take more than 2,000 milligrams per day unless advised by your doctor, since that level of niacin can cause side effects in many people. Talk with a health care professional about the proper level of supplement to treat your pellagra, particularly if you have any of the following health conditions: (5)
- Liver disease
- Severe low blood pressure
- Peptic ulcer disease
- Allergies
- A thyroid disorder
- Gallbladder disease
- Diabetes
- Arthritis gout
You can also ask your doctor whether you should take tryptophan and niacinamide, a related nutrient.
2. Eat a diet rich in niacin and tryptophan
Most people, particularly in developed countries, can get enough niacin and tryptophan from a healthy diet. Pellagra prevention — whether you are trying to avoid it in the first place or want to avoid getting it again — is as easy as following a high-protein diet or taking B vitamin supplements for most people.
To get niacin in your diet, eat plenty of niacin-rich foods, including: (5, 7)
- Milk
- Eggs
- Mushrooms
- Liver
- Peas
- Sunflower seeds
- Avocado
- Rice
- Enriched grains, including bread and cereal
- Legumes
- Peanuts
- Fish
- Poultry
- Lean meat
- Leafy greens
- Brewer’s yeast
You can also make sure you’re getting plenty of tryptophan in your diet without taking a supplement, in most cases. There are many opportunities to get great doses of niacin and tryptophan in the same foods (seeds, meats, fish, eggs and cheeses in particular).
Foods high in tryptophan include: (8)
- Seeds and nuts (particularly pumpkin and squash seeds, chia seeds and sesame or sunflower seeds)
- Cheeses, such as parmesan, cheddar, mozzarella and Romano
- Rabbit, lean beef or pork, goat and veal
- Chicken and turkey
- Halibut, salmon, rockfish, trout, tuna and other fish
- Shellfish
- Uncooked oats, buckwheat and wheat bran
- Beans and lentils
- Eggs
3. Curb diarrhea
If you have diarrhea related to your pellagra, you’re not alone. About half of all people with niacin deficiency develop this unpleasant symptom. Natural ways you can try to stop diarrhea include:
- Stay hydrated. Drink water, tea and coconut water to replace the fluid you are losing and to replace electrolytes
- Follow the BRAT diet for a day or two: Bananas, rice, applesauce and toast
- Move on to other bland, easy-to-digest foods for the next few days
- Gradually add in a greater amount of fiber from whole grains, fruit and vegetables. These should help bulk up your stool
- Avoid foods that may make diarrhea worse for some people (particularly if you have Crohn’s disease or another gastrointestinal condition with diarrhea triggers). Triggers may include:
- Dairy
- Processed fats and oils
- Added sugars or sweeteners
- Caffeine
- Carbonated or sugary drinks
- Alcohol

4. Protect your skin
Once you are receiving niacin or nicotinamide supplements, you should start to feel better within a few days. However, it may take several months for your skin to fully heal, and some people may have permanent pigment (color) loss in their affected skin. While your skin is affected and recovering, take care to protect it with some of these tips: (9)
- Use sunscreen when you go outdoors. You can try spray sunscreens if it is painful or difficult to apply to flaky rashes.
- Wear hats and clothing that protect your skin from the sun.
- Avoid sun exposure while pellagra is at its worst (before treatment begins to improve symptoms).
- Apply moisturizers at least once a day to all affected skin.
- Rich creams and body lotions intended to retain moisture for 24 hours may help you avoid constant reapplication.
- Avoid moisturizers, soaps, sunscreens and other skin care products with harsh chemicals or irritating additives.
- If you have broken skin, try using an ointment that can provide a good moisture barrier and also keep out germs, without irritating your wound.
- Petroleum jelly and similar mild ointments can help you protect broken skin until it heals enough to use regular moisturizer.
- Avoid other things that can irritate damaged or painful skin, such as hot showers or baths, hot tubs, too much time in the shower, swimming in chlorinated water, makeup with irritating chemicals, perfumes or deodorants on affected skin, etc.
- Watch for signs of infection. Contact your health care provider if you think you have a skin infection.
5. Manage other symptoms
Although some people have virtually no symptoms of pellagra, many people have some symptoms beyond the 3 Ds. Mild depression, anxiety, headaches, fatigue and indigestion are some symptoms that may respond to natural therapies once your niacin deficiency is being treated.
Please note: If you have secondary pellagra caused by something other than a lack of niacin, you may require other treatments for the underlying problem. Similarly, your symptoms may be a result of another condition, rather than the deficiency itself. Seek care from a medical professional to understand what symptoms you have due to pellagra and how best to treat yourself to avoid symptoms and progression.
Consider these ways to treat common symptoms of niacin deficiency:
- Rest. Right when you start receiving treatment, you may still feel the fatigue that niacin deficiency can cause. Rest to give your body time to start recovering. This can also give your brain a rest from some of the neurological symptoms that may happen when you have pellagra, such as anxiety and confusion.
- Try yoga. Once you feel physically well enough for activity, consider trying yoga. It is a gentle form of exercise that may also ease depression and anxiety. (10, 11)
- Meditate. Meditation can help relieve pain, depression, anxiety and stress. (12) Try free meditation videos on YouTube or read Dr. Axe’s approach for effective guided meditation.
- Talk with someone. Having a condition that affects your energy levels, appearance and mental and physical health can take its toll. Talk to someone you feel comfortable with — a family member, a friend, a health care provider, a counselor, a spiritual leader — to help yourself cope. Not only can formal therapy benefit you by reducing anxiety and depression, but you may also be able to snag a few protein-rich recipes to try out from your friends or family!
- Keep a food journal. If you have diarrhea, indigestion, nausea or other gastrointestinal issues related to your pellagra, a food journal may help. This allows you to track what you eat and how you feel throughout the day. In time, you may notice patterns. For example, you may find that every time you have French fries, you feel bloated and nauseous. Journals help identify triggers that you can avoid until your health improves.
- Ease your headaches. With niacin supplementation, your headaches should quickly go away. Until then, consider taking an overall B vitamin supplement. Check that any niacin in the supplement doesn’t put you beyond what your doctor recommends for your treatment, or ask if an overall B vitamin supplement can replace a niacin-only supplement. You should also stay hydrated, get enough rest and avoid triggers (which may include sunlight, loud noises and more). Aromatherapy and other herbs may also provide relief, and are described in Dr. Axe’s post on natural headache remedies.

Precautions
- Do not attempt to self-diagnose pellagra. This condition shares signs and symptoms with many other health conditions. If not properly treated, niacin deficiency can cause dementia, permanent skin changes, lasting nerve damage and death.
- Do not treat diagnosed pellagra without the guidance of a physician. You may need liver function tests or other therapy to address the root cause of your condition.
- Do not take niacin supplement doses of 2,000 milligrams or greater without the guidance of a physician, since it can cause serious side effects and drug interactions.
- Do not take niacin supplements with: (6)
- Alcohol
- Gout medications
- Blood pressure drugs or related herbs and supplements
- Drugs for diabetes or cholesterol
- Zinc or chromium
- Any drugs, herbs or supplements that are processed by the liver or that can cause liver damage (hepatotoxicity)
- Don’t take prescription-strength niacin if you are pregnant.
- If you have pellagra caused by another condition, such as alcoholism or a metabolic problem, it is essential to seek care for your health problem. Without proper care you are at risk for long-term complications of pellagra (including death) and other health risks associated with your main health issue.
Final Thoughts
- Pellagra is niacin deficiency and is rare in developed countries.
- Pellagra can cause diarrhea, dermatitis, dementia and even death (known as pellagra’s four Ds).
- When treated early, most people experience a full cure.
- In most cases, it can be treated with a niacin or nicotinamide supplement of 20 to 30 milligrams per day. However, some people have health conditions that cause the deficiency. Those people may need other treatments for the deficiency to resolve.
- Preventing pellagra is usually as simple as maintaining a well-balanced diet that is rich in protein. If you have secondary pellagra, you may also require treatment of the condition causing the niacin or tryptophan deficiency in order to avoid getting it again.
5 Natural ways to help treat pellagra and its associated symptoms include:
- Take a niacin supplement
- Eat a diet rich in niacin and tryptophan
- Curb diarrhea
- Protect your skin
- Manage other symptoms









