This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
7 Natural Treatments for Seborrheic Dermatitis
November 14, 2016

Seborrheic dermatitis, a type of skin condition that most often causes facial dryness and scalp itchiness, affects about 6 million children and adults in the U.S. It can be tricky to recognize or diagnose seborrheic dermatitis because the skin reactions it triggers mimic those caused by similar conditions like psoriasis, other forms of eczema or even allergic reactions.
Like many other conditions caused by abnormal immune responses, patients tend to experience on-and-0ff intervals of seborrheic dermatitis symptoms. This means most have episodes of skin reactions suddenly flaring up and then periods when they go away. Patients with dermatitis have reported that outbreaks are triggered by factors like: (1)
- Trauma, emotional stress or depression
- Fatigue and lack of sleep
- Exposure to damp or dry conditions in the home and/or workplace, such as excessive air-conditioning
- Systemic infections
- Use of certain medications
- Other immune-disrupting factors
Chronic skin diseases can result in a diminished quality of life and emotional distress, especially if they get out of hand. (2) If you or a loved one are struggling with this condition, read on to find out what you can do to change your situation for the better.
What Is Seborrheic Dermatitis?
Seborrheic dermatitis is defined as a chronic, recurrent, inflammatory skin condition characterized by erythema and skin flaking. It’s actually a form of eczema and is also known as seborrheic eczema. It usually causes symptoms like itching, skin dryness or oiliness, and other common changes in skin texture, such as scalp dandruff. Unlike many people assume, seborrheic dermatitis is not contagious.
In dermatology terms, patients will “develop symmetrical, well demarcated, dull or yellowish red patches and plaques with overlying adherent, yellowish greasy scales.” Symptoms most often appear on areas of the skin that normally have high concentrations of sebaceous glands (read: oily skin areas). The parts of the body most likely to develop itch and other symptoms are: (3)
- Face — dryness and redness usually form on the forehead near the skin folds, eyebrows and front hairline
- Scalp — dandruff is regarded as a mild, noninflammatory form of seborrheic dermatitis. More than half of patients with this condition develop symptoms on the scalp.
- Ears
- Upper chest
- Back
- Near the neck or collarbone
- Any body fold, such as near the groin
There is no known cure for seborrheic dermatitis to date. However, by managing the underlying causes with natural means, you may be able to reduce or reverse the symptoms permanently. However, most people do experience flare-ups throughout their lifetime.
Seborrheic Dermatitis Signs & Symptoms
Something that makes seborrheic dermatitis unique is that it can cause both extra skin dryness and oiliness. In fact, surprisingly, oily skin is one of the most frequent causes of dandruff. It sometimes also contributes to other skin irritations (like infections or acne). Seborrheic dermatitis is marked by red, greasy skin covered with flaky white or yellow scales, making it different from conditions like psoriasis.
The most common signs and symptoms of seborrheic dermatitis are: (4)
- Scaly patches and dandruff forming on the scalp. Dandruff is usually “stubborn” and doesn’t respond well even to over-the-counter products like dandruff shampoos or oily treatments. Sometimes, rash-like lesions form on the scalp that can range from mildly itchy to brownish crusts and cause the skin to stick to the hair.
- Red skin that’s sensitive and very dry. Irritated seborrheic dermatitis can cause very dry skin to become yellow or pink in certain areas.
- Extra dryness and flaking in areas of the skin that fold or that are usually oily, including the “T-zone” of the face (the area covering the nose, chin and forehead), upper chest and back.
- Skin peeling called erythema, which sometimes appears as macules (a discolored patch of skin ) or plaques with dry white or moist oily scales. Even when skin peels, papules or pustules are not very common.
- It’s possible for secondary bacterial infections to occur if bacteria proliferates inside dry patches or openings of the skin.
This condition also affects a high percentage of infants (around 70 percent) and sometimes children. In fact, cradle cap is one type of seborrheic dermatitis, which affects a baby’s scalp.Seborrheic dermatitis can also develop in the diaper area of infants and is sometimes mistaken for diaper rash. (5)
In infants, the condition generally resolves by age 3 or 4 months. But children with untreated food allergies can sometimes continue to show symptoms for years. (6)
Another time period when seborrheic dermatitis tends to develop is during puberty, when hormone shifts can affect the glands of the skin and oil production. Dermatitis prevalence increases again in adults over the age of 50.
Causes and Risk Factors of Seborrheic Dermatitis
What causes seborrheic dermatitis? Although experts still aren’t totally sure why dermatitis develops, it appears to be related to the composition of the skin’s sebaceous gland secretions, the proliferation of Malassezia yeasts that can cause negative skin responses, and abnormal immune responses. (7)
Sebum is the component of the skin’s surface that produces oils (lipids) to keep the skin adequately hydrated. It contains high amounts of squalene, wax esters and triglycerides that normally prevent dryness. Research suggests that people with dermatitis might have close-t0-normal sebaceous gland activity. However, changes in the composition of the skin’s surface — coupled with a hyperactive immune system — might trigger abnormal responses to microbes on the skin.
Immune responses increase as there’s also a higher growth rate of lipid-dependent microorganisms, including yeasts. Malassezia yeasts are normally present on the skin in sebum-rich (oily) areas of the body, such as the face, scalp, trunk and back. But in people with seborrheic dermatitis, they appear to be produced at higher levels. In the process they leave behind byproducts that cause skin irritation and inflammation.
Seborrheic dermatitis commonly occurs among patients with other health conditions that affect their immune systems and raise inflammation.
Examples of these conditions are HIV (human immunodeficiency virus), autoimmune diseases, food allergies, mood disorders, recurrent infections or neurological disorders like Parkinson’s disease. Seborrheic dermatitis is especially common in those with severely compromised immune function. In fact, it affects approximately up to 11 percent of immuno-competent adults and up to 85 percent to 95 percent of HIV patients. (8) Those with HIV usually experience more intense cases of seborrheic dermatitis and often do not respond to standard treatment as quickly as patients without immunocompromised systems. (9)
The American Academy of Dermatology (AAD) also notes that your risk for seborrheic dermatitis also increases if you are taking one of the following medications: (10)
- Interferon
- Lithium
- Psoralen
Even in people who don’t have other serious health conditions, risk factors for dermatitis include:
- Significant life stress
- Experiencing trauma
- Low exposure to sunlight (resulting in possible vitamin D deficiency)
- Hormonal changes, such as pregnancy or menopause
Conventional Treatment for Seborrheic Dermatitis
Conventional treatment options for treating symptoms of seborrheic dermatitis, especially the most common symptom, scalp dandruff, include: (11)
Medicated Shampoo
The first over-the-counter (OTC) options doctors may prescribe include a variety of different medicated shampoos. The four basic types of these shampoos are coal tar shampoo, selenium sulfide shampoo, tea tree oil shampoo and zinc pyrithione shampoo. You can use tea tree oil shampoo daily. Use the other three types twice a week.
- Coal tar shampoo is a keratolytic agent. These are meant to soften the protein keratin on the skin and allow dead skin cells to be sloughed off more easily. Keratolytic agents contain sulfur and salicylic acid. The latter is especially important in conventional skin treatment because salicylic acid is oil-soluble and reduces inflammation on the skin. That’s why it’s commonly used to treat acne. Common side effects of coal tar shampoo include contact dermatitis, folliculitis (tender, red bumps on hair follicles) and photosensitivity (allergic reaction caused by sunlight).
- Selenium sulfide shampoo is intended to help treat seborrheic dermatitis by fighting infection, relieving the itch associated with this dandruff and removing scaly particles of dandruff. Common side effects include alopecia (a hair loss disease), hair discoloration and skin irritation.
- Tea tree oil shampoo uses the antifungal and antibacterial properties of tea tree oil to treat seborrheic dermatitis and the resulting dandruff while also conditioning the skin naturally. It seems this treatment can be effective for mild-to-moderate dandruff symptoms. (12) However, people have reported side effects of allergic contact dermatitis and skin irritation.
- Zinc pyrithione shampoo is another antifungal and antibacterial agent commonly prescribed to patients with seborrheic dermatitis. It’s one of the least expensive options. The only known common side effect zinc pyrithione may cause is skin irritation.
Topical Agents
Dermatology practitioners often prescribe topical creams, shampoos and gels as medication to treat the symptoms of seborrheic dermatitis. They are broken down into categories, including:
- Antifungal shampoos (brand names Loprox and Nizoral)
- Topical corticosteroids (Luxiq, Clobex, Capex, Sylanar, Beta-Val, desonide products, fluocinolone products and hydrocortisone cream)
- Topical antifungals (Ciclodan, ketoconazole cream and Ertaczo)
- Topical calcineurin inhibitors
Calcineurin inhibitors include pimecrolimus or tacrolimus. They work by inhibiting certain immune system actions that cause inflammatory responses. (13) Unlike tacrolimus, pimecrolimus is a more targeted chemical compound that does not seem to carry the same risk for skin atrophy as its counterpart.
These agents have a number of known side effects, including stinging, cough, fever, skin atrophy, burning, heading, upper respiratory infection and flu-like symptoms (among others). Not much is known about the long-term effects of calcineurin inhibitors. Those medications come with warnings that isolated cases of skin cancer and lymphoma have occurred. Never use these medications long-term under any circumstances. (14)
7 Natural Ways to Treat Seborrheic Dermatitis
1. Treat Itchy Dandruff/Scalp Dryness
Dandruff (the shedding of excessive amounts of dead skin flakes from the scalp) is very common in both adults and children. But this doesn’t mean it’s entirely “normal.” Studies suggest that dandruff is really the overaccumulation of dead skin. Dandruff causes can include low immune function, reactions to the dry winter air, a vitamin-deficient diet and harsh chemicals found in things like chemical-heavy shampoos. Malassezia yeast lives on the scalps of most adults. In excess, it can cause more skin cells to grow and then to die and fall/flake off.
Common seborrheic dermatitis scalp treatments that you can try include:
- Applying a combination of hydrating coconut oil and essential oils to the scalp (more on this below).
- Making a DIY dry scalp shampoo or mask to cover itchy areas.
- Not shampooing too often but also making sure to clear the scalp. You may have a healthier scalp and hairline if you shampoo about every two to three days, since this can allow natural oils produced by your skin to stay at regular levels.
- Increasing intake of antioxidant-rich foods, such as berries and leafy greens.
- Using a humidifier if the air in your home is very dry (dandruff usually gets worse during the fall and winter when air is very dry).
As described above, low immune function and high inflammation levels (sometimes in combination with hormone imbalances) are at the root of most skin conditions. Skin irritations are often caused, or at least made worse, by chronic stress, depression, anxiety and fatigue. To improve overall immunity, try following these tips:
- Get seven to eight hours of sleep each night.
- Exercise regularly to control stress.
- Consider taking supplements like omega-3 fatty acids and probiotics.
- Spend at least some time outdoors in nature or the the sun each day.
- Keep up with hobbies and relationships to feel more connected and relaxed.
- Try natural stress relievers like meditation, yoga, prayer, reading, writing or volunteering.
- Consider using adaptogen herbs that help your body deal with stress and control cortisol levels.
- Consume more anti-inflammatory foods, including garlic, apple cider vinegar, banana, avocado, flaxseed, ginger and coconut oil.
3. Reduce Intake of Inflammatory and Allergen Foods
To help keep inflammation as low as possible, it’s important to keep your diet as unprocessed as possible. Focus on eating whole foods. Minimize your intake of packaged and processed foods known to worsen autoimmune reactions and allergies, including:
- Added sugar and sweetened beverages.
- Processed oils like corn, soy, canola, safflower and sunflower oil.
- Fried foods and trans fats.
- If you’re prone to allergies, foods like refined grain products made with wheat, conventional dairy, shellfish and peanuts.

Be sure to supply skin with enough hydration by drinking plenty of water throughout the day. Avoid consuming too much salty food, alcohol, caffeine or sugary drinks, which can aggravate and dry out the skin. Instead try alternatives like coconut water, green tea, and homemade smoothies or juices to increase fluid intake.
5. Use Healing Coconut and Essential Oils
Because real coconut oil contains medium-chain fatty acids, including lauric acid and capric acid, it has strong antiviral, antimicrobial and antifungal properties. Coconut oil applied to the skin has been shown to help reduce excess yeast, microbes and fungus that can lead to irritation, too much oiliness or dryness. Even better, use coconut oil on the skin along with soothing essential oils — like cedarwood oil, lemongrass, rosemary, tea tree and lavender.
To make a homemade treatment for scaling, itchy skin that you can keep at home to use several times, combine 8 drops cedarwood oil, 8 drops rosemary oil, 6 drops tea tree oil, 1 teaspoon local honey and 4 ounces coconut oil (or olive or almond oil). Massage into the affected area, including the scalp, leave on for about 15–20 minutes, and then gently rub or rinse off. These oils contain antiviral, antibacterial and antifungal properties, much like coconut oil. Plus they can reduce inflammation and treat infections.
6. Take a Zinc Supplement
It’s more common than you might think to have a zinc deficiency. Rash and skin irritation are two common signs of this deficiency. This is one reason dermatology rules sometimes suggest testing for low levels of zinc for those with these symptoms. (15)
Like I mentioned above, zinc is also included in some topical agents used to treat seborrheic dermatitis. However, more attention is now paid to the value of internal zinc supplements. For those who experience this condition related to zinc deficiency, supplementing with zinc can help to address some of the underlying problem. (16)
7. Avoid Irritating Beauty Products
Applying chemical-laden products to your skin on a regular basis is likely to make symptoms of dermatitis worse. Itching, picking and over-cleaning the skin might also make things worse. (17)
Use natural, organic products on your skin as much as possible. Be especially careful to avoid commercial shampoos with chemicals if you have dandruff. Most beauty products contain chemicals that are drying or harmful. Look for those made without ingredients like parabens, sodium laureth or lauryl sulfate. Instead, to clean, tone and hydrate the skin without irritation, turn to natural skin care products like apple cider vinegar, tea tree, witch hazel, shea butter and aloe vera gel. It’s also important to avoid other causes of contact dermatitis, including:
- Poison ivy or poison oak
- Fragrant soaps, detergents, shampoos, perfumes and lotions that might be on your clothes or household fabrics
- Latex (if you have an allergy)
- Specific natural products that might trigger an allergy, such as certain essential oils or active constituents if you’ve experienced rashes in the past
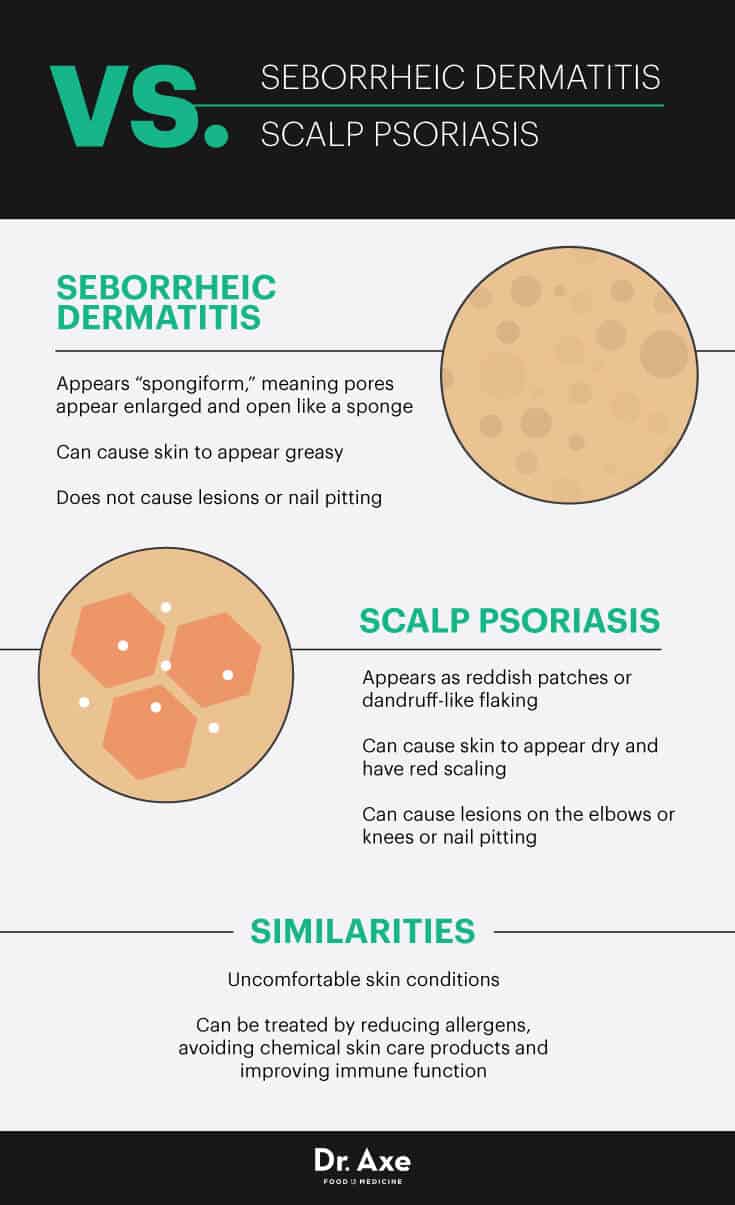
Seborrheic Dermatitis vs. Scalp Psoriasis
Seborrheic dermatitis can be accompanied by other dermatological disorders, which can make treatment difficult. The good news, however, is that many of the same treatments used for dermatitis (like reducing intake of allergens, avoiding chemical skin care products and improving immune function) also apply to treating skin conditions such as eczema and psoriasis.
Early seborrheic dermatitis can be distinguished from scalp psoriasis because it appears “spongiform,” meaning pores appear enlarged and open like a sponge.
Seborrheic dermatitis can also cause skin to appear greasy, while psoriasis usually causes more dryness and red scaling.
Patients with psoriasis who have facial or scalp flaking can also look for signs of lesions on the elbows or knees. Psoriasis also causes nail pitting, while dermatitis normally doesn’t.
It is also possible to have a condition called sebopsoriasis, which is a combination of both seborrheic dermatitis and psoriasis.
Seborrheic Dermatitis Facts and Statistics
- About 1–5 percent of the general U.S. population suffers from seborrheic dermatitis. (18, 19)
- Up to 70 percent of infants experience some type of dermatitis on their scalps (often called cradle cap) within the first three months of life. (20)
- In adults, seborrheic dermatitis symptoms most commonly start between the ages of 30–50.
- Patients with seborrheic dermatitis most often develop symptoms on the face and scalp. About 88 percent of patients have facial symptoms, 70 percent on the scalp, 27 percent on the chest and only about 1 percent to 2 percent on the arms or legs.
- Dandruff is now considered a mild, noninflammatory form of seborrheic dermatitis. Dandruff is extremely common with a prevalence as high as 50 percent of the population.
- In the U.S., approximately $230 million is spent every year treating symptoms of seborrheic dermatitis, especially those affecting the face and scalp. This can cause the largest decrease in quality of life.
- More men than women have seborrheic dermatitis. But there appears to be no preference for any racial or ethnic group.
- People with other health conditions that affect the immune system get dermatitis most often, such as those with allergies, leaky gut syndrome or autoimmune disorders.
Precautions When Treating Seborrheic Dermatitis
Experts warn that because dermatitis tends to be chronic, patients should be made aware that seborrheic dermatitis is usually recurrent and that the condition may cause outbreaks of symptoms from time to time even after successful treatment. Rather than simply assuming your symptoms indicate seborrheic dermatitis, it’s important to visit a dermatologist to get an accurate diagnosis, since this helps with treatment.
Your doctor will be able to make a differential diagnosis between seborrheic dermatitis and other conditions like psoriasis, rosacea, Demodex dermatitis, atopic eczema, pityriasis versicolor, contact dermatitis and tinea infections. Knowing the specific type of skin condition you have, as well as what the underlying causes are, will keep symptoms from worsening or causing other untreated immune reactions.
Key Points About Seborrheic Dermatitis
- Seborrheic dermatitis is a type of eczema, most often causing facial redness, skin dryness or dandruff/scalp itchiness.
- Causes of seborrheic dermatitis are related to abnormal immune responses, growth of yeast on the skin and changes in oil production.
- Factors like emotional stress or depression, fatigue, exposure to dry conditions, systemic infections, use of certain medications, and other factors that can hinder immune function can all trigger symptoms.
Natural treatments for seborrheic dermatitis include:
- Applying essential oils and coconut oil to the skin
- Reducing intake of inflammatory or allergy-causing foods
- Controlling stress
- Avoiding chemical products that can increase skin irritation


