This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
Gut Bacteria Benefits: What Gut Bacteria Are & How They Improve Your Health
April 4, 2026
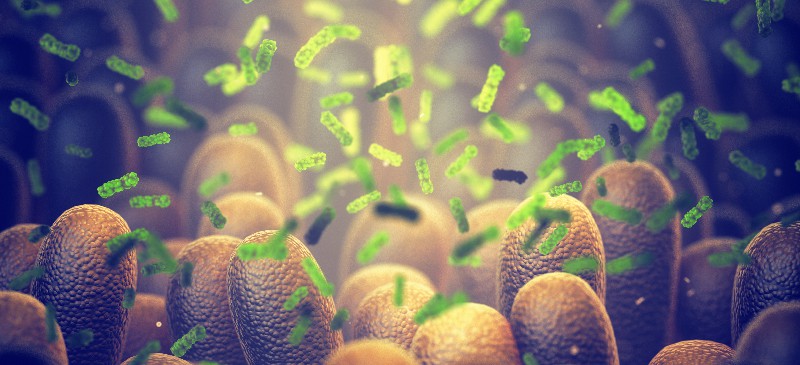
Gut bacteria are trillions of microorganisms living in your digestive tract that play a critical role in digestion, immune function, metabolism and even mental health. Understanding gut bacteria benefits can help you improve everything from nutrient absorption to inflammation and disease risk.
The gut microbiome is made up of both beneficial and harmful bacteria, and maintaining the right balance is essential for optimal health. When gut bacteria become imbalanced (a condition called dysbiosis), it can contribute to digestive issues, immune dysfunction and chronic disease.
What are gut bacteria?
Gut bacteria, also known as the gut microbiome, are trillions of microorganisms that live primarily in your intestines. These beneficial bacteria help regulate many key bodily functions and are essential for maintaining overall health.
Your gut microbiome contains trillions of bacteria that influence digestion, immunity and overall health.
Key roles of gut bacteria include:
- Digesting food and breaking down nutrients
- Producing essential vitamins, like B12 and K2
- Supporting immune system function
- Regulating inflammation
What is the role of bacteria in your gut?
A lot of someone’s health can be traced to the gut, specifically gut bacteria.
In the 1670s, scientist Antony van Leeuwenhoek first discovered the complex world of bacteria. At the time, he defined it as “free-living and parasitic microscopic protists, sperm cells, blood cells, microscopic nematodes and rotifers,” according to the University of California Museum of Paleontology.
Fast-forward to today (some 350-plus years later), and bacterial microbes are still at the forefront of medical research. That includes the trillions that live inside our guts and communicate directly with neurons in our brains.
This incredible finding is known as the gut-brain connection.
The human microbiome, or microbiota, is essentially the bacterial ecosystem living within our bodies, mostly within our guts. The intestinal microbiota is made up of trillions of microorganisms, most of which are bacterial and not harmful to our health.
Scientists have recognized for more than 100 years that bacteria in the gut are constantly communicating with neurons in the brain, earning the microbiome the nickname “the second brain.”
Not only do most gut bacteria not sicken us, but they are actually beneficial, vital to our health and play numerous roles.
Factors such as genetics, age, sex and diet continually influence the composition and profile of an individual’s microbiota. That means no two people’s gut bacteria are quite the same.
What do our gut bacteria do exactly, and how? Roles of gut bacteria include:
- Helping produce hormones, like serotonin
- Aiding in the extraction of energy (calories) and nutrients, including vitamins, minerals, amino acids, fatty acids and antioxidants
- Managing appetite and body weight
- Digesting fiber, which helps form stool
- Controlling our moods, motivation and cognitive health
- Preventing us from catching colds and viruses
- Helping repair damaged tissues and injuries
- Much, much more
One of the most important things that “good bacteria” (also known as probiotics) living in the microbiota do is contribute to our immune systems. This protects us against pathogen colonization and invasion of harmful microbes that enter the body every single day.
So where do things go wrong? Alterations in the microbiota (often called dysbiosis) can result for many reasons. Some of the most common are:
- exposure to various environmental pollutants and toxins
- consuming a poor diet lacking anti-inflammatory foods
- using toxic medications and over-the-counter drugs
- smoking cigarettes
- high amounts of stress
- exposure to harmful pathogens from other people who are sick
What are the effects of gut bacteria?
“Poor gut health” might bring to mind intestinal and digestive disorders, including inflammatory bowel disease, irritable bowel syndrome (IBS) and celiac disease, but these are far from the only problems tied to dysbiosis. Studies have shown that dysbiosis of the gut microbiota is associated with numerous disorders that affect us internally.
Some of these include altered hormone production, which might not always be obvious, and external issues (affecting us in more apparent ways, such as changing the appearance of our skin and body weight).
A lack of healthy gut bacteria is now tied to the onset of conditions like:
- Food allergies
- Asthma
- Diabetes
- Arthritis
- Fibromyalgia
- Eczema and psoriasis
- Poor recovery from seizures, spinal cord injuries or a stroke
- Metabolic syndrome and cardiovascular diseases
1. Autoimmune diseases
Recently much more has been uncovered about how bacterial species residing within the mucus layer of the colon have the ability to directly communicate with host cells in the immune system. This relationship can influence whether or not the immune system remains at homeostasis or triggers inflammatory mechanisms that destroy the body’s own healthy tissue and cells.
Autoimmune disease symptoms, including diseases like multiple sclerosis, type 1 diabetes and rheumatoid arthritis, all have links to dysbiosis. In fact, we now know that pathogens entering the body through toxins and a poor diet have the potential to cause microbial disruption. This can trigger both local and systemic inflammation.
This inflammation then creates a vicious cycle because it alters the composition of the gut/microbiota, reduces the barrier that the gut naturally has with the rest of the body, decreases nutrient absorption, increases permeability (also called leaky gut) and causes numerous symptoms tied to autoimmunity. These symptoms can include skin reactions, indigestion, mood-related problems, joint pain and fatigue.
Although we have more to learn about probiotics’ effects on autoimmunity, research has suggested that acquiring bacterial strains, including Lactobacillus casei shirota, can have positive effects on controlling inflammatory reactions.
2. Depression
Our brains contain billions of neurons, and these have a close working relationship with the trillions of “good” and “bad” bacteria alive in the gut. Bacteria seem to be instrumental in how our brains develop, how we behave, our capabilities for handling stress and how we respond to treatments for mood-related issues, like depression and anxiety.
It’s been found that in stressful situations, the microbiota profile may actually change itself, shifting how different bacteria interact with one another. The gut-brain relationship basically comes down to how the immune system alters the nervous system.
Unsurprisingly, when your gut bacteria are healthy and operating properly, such as by ingesting probiotics and prebiotics, you can help manage and reduce symptoms of depression and anxiety.
3. Obesity and weight gain
Each year, the U.S. population spends more money on diets than the amount needed to feed all the hungry people in the rest of the world. We’ve all gotten the message by now that we should be eating less and moving more.
Less talked about? The need to take care of our gut health in order to manage our appetites, hormones and energy expenditure.
What does gut bacteria have to do with obesity, you might be wondering? Although the underlying mechanisms are still not entirely clear, obesity is known to be associated with chronic low-grade inflammation and hormonal changes that lead us to overeat:
Research has suggested overeating and obesity might be tied to reductions in certain beneficial bacteria that populate a healthy microbiome. Certain studies have found that some obese individuals have higher levels of two major classes of bacteria: bacteroides and firmicutes. These can cause increases in inflammatory metabolic endotoxins, plus decreased mucus lining the intestinal wall and therefore more gut permeability.
The gut microbiota also contributes to retention of fat mass, and certain bacterial gut changes have been shown to reduce leptin sensitivity (meaning we feel satisfied less easily).
A study published in Endocrinology also showed that dysbiosis might result in reduced expression of obesity-suppressing neuropeptides proglucagons in the brainstem.
4. Irritable bowel disease (IBD)
IBD is a term used to describe hard-to-treat disorders that cause bloody diarrhea, abdominal pain, cramping, and sometimes malnutrition and weight loss. Although treating IBD can be complicated and sometimes require various types of intervention, probiotics seem to help manage IBD symptoms (especially severe diarrhea) in many patients and can help with reversal of inflammation in the digestive tract.
Studies have suggested that bacterial strains and a combination formula might be most effective in IBD treatment. If you haven’t been diagnosed with IBD but still have occasional digestive problems, such as diarrhea, bacterial strains including Saccharomyces boulardii and Lactobacillus GG can likely help.
What are the top gut bacteria benefits?
1. Gut bacteria improve digestion
One of the most important gut bacteria benefits is improved digestion. Beneficial gut bacteria help break down complex carbohydrates, fiber and proteins, making nutrients easier for your body to absorb.
2. Gut bacteria support immune function
Gut bacteria play a critical role in immune health. More than 70 percent of the immune system is connected to the gut, and beneficial bacteria help protect against harmful pathogens.
3. Gut bacteria produce essential nutrients
Gut bacteria help produce important nutrients such as vitamin B12, vitamin K2 and short-chain fatty acids like butyrate, which support colon health.
4. Gut bacteria regulate inflammation
Healthy gut bacteria help regulate inflammation in the body. When gut bacteria are balanced, they can help reduce chronic inflammation, which is linked to many diseases.
5. Gut bacteria influence mental health
Gut bacteria are closely connected to the brain through the gut-brain axis. This means gut bacteria can influence mood, stress levels and cognitive function.
Signs of unhealthy gut bacteria
An imbalance in gut bacteria (dysbiosis) can negatively affect digestion and immune health.
What are common signs of gut bacteria imbalance? These can include:
- Frequent digestive issues, like bloating, gas, acid reflux, constipation and diarrhea (especially if stool ever appears bloody or causes unexplained weight loss)
- Skin issues like acne, mild skin rashes and other signs of skin inflammation
- Frequently getting colds, viruses and other “common” illnesses
- Stuffy nose, respiratory infections and trouble breathing
- Low energy levels and fatigue
- Achy joints and muscular pains
- Sugar cravings
- Frequent illness
How to improve gut bacteria
Even if you don’t necessarily suffer from one of the disorders or diseases mentioned above, you can still benefit from improving gut health. Considering the average person eating a “Westernized/American diet” doesn’t ordinarily consume many probiotic foods (plus likely lacks at least several nutrients key to gut health, including prebiotics and fiber), most of us can afford to make some dietary and lifestyle changes.
Here are simple steps you can take now to start improving gut bacteria:
- Consume probiotic foods, such as yogurt, kefir, cultured veggies and kombucha. Also consider taking a high-quality probiotic supplement.
- Avoid common allergen foods, which can make poor gut health even worse. These include conventional dairy, shellfish, peanuts, soy and gluten products. Processed/packaged foods, fried foods and too much added sugar might also worsen gut health (not to mention cause other issues), so work on reducing these as well.
- Eat plenty of fiber and prebiotics, which help probiotics in the gut thrive.
- Quit smoking, and reduce alcohol intake to moderate levels.
- To avoid the potential dangers of antibiotics, only take them when absolutely necessary. Antibiotics can wipe out both good and bad bacteria in the gut.
- Vary your protein intake. It’s been found that high consumption of animal products and very high-protein diets might contribute to carcinogenic metabolites forming in the microbiota that alter immunity. Rather than making meat, eggs or cheese the center of all your meals, try to focus on variety and eating more plant foods for protein, like soaked beans, nuts, seeds and legumes.
- Reduce toxin exposure in your home by using natural cleaning products. The same goes for beauty or skin care products. Try switching to natural skin care ingredients like coconut oil, which don’t contain harsh chemicals. Avoid antibacterial soaps, too.
- Exercise and manage stress to keep inflammation levels low.
- Introduce traditional gut-friendly foods into your diet, like bone broth, a great source of collagen, which helps rebuild the gut lining and prevent permeability.
Frequently asked questions
What are gut bacteria?
Gut bacteria are microorganisms that live in your digestive tract and help regulate digestion, immunity and overall health.
What are the main gut bacteria benefits?
The main gut bacteria benefits include improved digestion, stronger immune function, nutrient production, reduced inflammation and better mental health.
How do you increase good gut bacteria?
You can increase good gut bacteria by eating probiotic and prebiotic foods, reducing sugar intake, and managing stress.
What kills good gut bacteria?
Antibiotics, poor diet, high sugar intake and chronic stress can kill or reduce beneficial gut bacteria.
Can gut bacteria affect mental health?
Yes, gut bacteria influence the brain through the gut-brain axis and can impact mood, stress and cognitive function.
What naturally kills bad bacteria in the gut?
- Probiotics: Foods like yogurt, kefir and fermented vegetables contain probiotics that promote good bacteria, which can outcompete bad bacteria.
- Antimicrobial herbs: Garlic, oregano and thyme have natural antibacterial properties.
- Polyphenol-rich foods: Green tea, cranberries and dark chocolate contain polyphenols that inhibit harmful bacteria.
- Fiber-rich foods: Soluble fiber feeds good bacteria, improving gut health and indirectly reducing bad bacteria.
How do you starve bad gut bacteria?
- Reduce sugar and refined carbs: Bad bacteria thrive on sugar and processed carbohydrates.
- Avoid artificial sweeteners: Some sweeteners, like sucralose, can alter gut bacteria and promote harmful strains.
- Consume more prebiotics: Foods like garlic, onions and bananas feed good bacteria, helping them outcompete bad bacteria.
- Limit ultra-processed foods: These often lack fiber and contain additives that can disrupt gut bacteria.
How do you increase good bacteria in the gut naturally?
- Eat fermented foods: Sauerkraut, kimchi, miso and kombucha are rich in probiotics.
- Consume prebiotic foods: Asparagus, chicory root and oats feed beneficial bacteria.
- Include diverse plants in your diet: A varied diet with many fruits, vegetables and whole grains fosters a diverse microbiome.
- Stay hydrated: Proper hydration supports mucosal lining health, creating a favorable environment for good bacteria.
- Reduce stress and sleep well: Chronic stress and poor sleep can harm gut bacteria.
How do I correct my gut bacteria?
- Adopt a balanced diet: Focus on whole, unprocessed foods rich in fiber and low in added sugars.
- Take a quality probiotic supplement: Consult a healthcare provider to find a strain suited to your needs.
- Exercise regularly: Physical activity promotes bacterial diversity.
- Avoid unnecessary antibiotics: They can disrupt the balance of gut bacteria.
- Get enough sleep: Poor sleep patterns can negatively affect gut health.
What are the symptoms of gut bacteria?
- Digestive issues: Bloating, constipation, diarrhea and heartburn.
- Food intolerances: Difficulty digesting certain foods.
- Fatigue: Low energy levels.
- Skin problems: Acne, eczema or rashes.
- Mood changes: Anxiety, depression or irritability due to the gut-brain axis.
- Weakened immunity: Frequent colds or infections.
What are the 4 types of gut bacteria?
The human gut primarily consists of the following bacterial phyla:
- Firmicutes: Aid in energy absorption and nutrient metabolism.
- Bacteroidetes: Help digest carbohydrates and regulate fat storage.
- Actinobacteria: Include beneficial species like Bifidobacteria, which produce vitamins and protect against pathogens.
- Proteobacteria: Some species can become opportunistic pathogens if overgrown.
What destroys gut bacteria?
- Antibiotics: Can kill both good and bad bacteria.
- Poor diet: High sugar, processed foods and low-fiber diets harm gut health.
- Stress: Chronic stress alters gut microbiota composition.
- Lack of sleep: Reduces microbial diversity.
- Alcohol: Excessive consumption harms gut lining and bacteria.
- Infections or illnesses: Can disrupt the microbiome.
- Environmental toxins: Pesticides, heavy metals and pollution can negatively impact gut bacteria.
Conclusion
- Understanding gut bacteria benefits is essential for improving your overall health.
- By supporting your gut microbiome through diet and lifestyle, you can enhance digestion, strengthen immunity and reduce inflammation.