This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
Milk Allergy Symptoms & 7 Natural Ways to Manage
January 5, 2023

Did you know that milk is one of the most common food allergens in existence? It’s estimated that between 2–3 percent of children under the age of 3 have a milk allergy. Experts used to think that these were just temporary baby allergies or infant allergies and kids would outgrow their dairy allergy once they were 3 years old. But research has shown this isn’t necessarily the case.
In fact, at least one study has demonstrated that less than 20 percent of children outgrew their milk allergy by time they turned 4 years old. While 80 percent may outgrow it by the age of 16, that’s still leaving a whole lot of adults who are dealing with a milk allergy for the rest of their lives.
The good news is that there are a lot of natural ways to deal with this common food allergy.
What Is a Milk Allergy?
Before we define a milk allergy, which is also known as a dairy allergy, let’s talk about just what is milk? Milk can be defined as a white liquid secreted by the mammary glands of female mammals, which typically nourishes infant mammals for a period of time starting immediately after birth.
The majority of the milk and milk products consumed in Western countries, including the United States, come from cows.
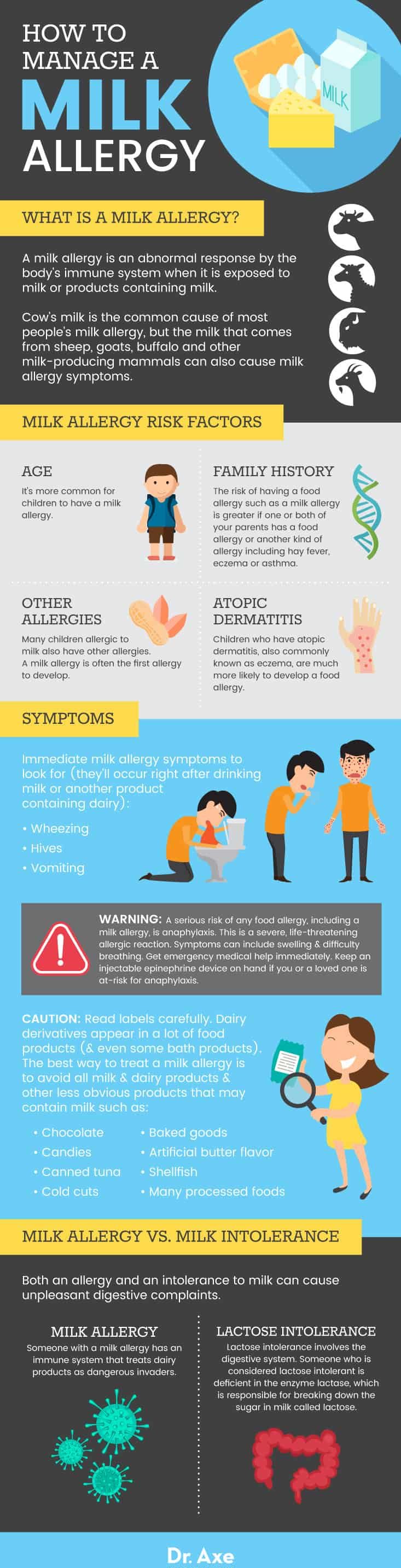
A milk allergy is an abnormal response by the body’s immune system when it is exposed to milk or products containing milk. Someone who is allergic to cow’s milk is reacting badly to one or more of the proteins in it. The offending milk protein can be casein (a casein allergy) or whey (a whey protein allergy). Some people with milk allergies are allergic to both casein and whey.
Cow’s milk is the common cause of most people’s milk allergy, but the milk that comes from sheep, goats, buffalo and other milk-producing mammals can also cause milk allergy symptoms. Whenever someone with a milk allergy consumes milk or milk products, the body sees the protein(s) as dangerous intruders.
The immune system then goes into overdrive trying to fend off the “intruder.” This is what causes the allergic reaction and unpleasant allergy symptoms as chemicals like histamine are released into the body. An allergic reaction to milk usually occurs within minutes to hours after consuming milk or products that contain milk.
Immunoglobulin E, or IgE, is an antibody normally found in humans that causes allergy symptoms. An allergen-specific immunoglobulin E (IgE) blood test can be conducted to determine if a child or adult is allergic to a particular substance such as milk.
Milk Allergy Vs. Milk Intolerance
Both an allergy and an intolerance to milk can cause unpleasant digestive complaints. How do you know if you are truly allergic to milk and dairy or if you are just intolerant or sensitive?
Typically, a food allergy comes on suddenly and can be much more dangerous and even fatal. With a milk allergy, consuming just a little bit of dairy can trigger a reaction while an intolerance can require eating a lot of dairy.
So it’s possible not to be allergic to milk but to either have a milk protein intolerance or lactose intolerance. Symptoms of a lactose intolerance or a milk protein intolerance can include the following digestive complains after consuming milk or products containing milk: bloating, gas or diarrhea.
All milk from mammals is naturally lactose milk, meaning it contains the milk sugar lactose. People with lactose intolerance often consume lactose-free milks. People with a milk allergy cannot even tolerate lactose-free milk.
Someone with a milk allergy has an immune system that treats dairy products as dangerous invaders. Meanwhile, lactose intolerance involves the digestive system. Someone who is considered lactose intolerant is deficient in the enzyme lactase, which is responsible for breaking down the sugar in milk called lactose. An individual with a milk protein sensitivity or intolerance has trouble breaking down the protein in milk called casein.
Symptoms
When you have a a milk allergy, you may notice unpleasant symptoms within just a few minutes after having dairy. Or it could take up to a few hours. An allergic response to dairy can vary by individual.
Either way, symptoms of dairy allergy are not pleasant. People with a cow’s milk allergy may also be allergic to the milk of other domesticated mammals such as goat’s milk or sheep’s milk.
Immediate milk allergy symptoms to look for (they’ll occur right after drinking milk or another product containing dairy):
- Wheezing
- Hives
- Vomiting
Some symptoms of milk allergy aren’t immediate and take time to appear. These later-onset dairy allergy symptoms can include:
- Abdominal cramps
- Loose stools, which may contain blood
- Diarrhea
- Coughing or wheezing
- Runny nose
- Watery eyes
- Itchy milk allergy rash on the skin, commonly found around the mouth
- Colic (in babies)
Causes
So what exactly causes a milk allergy? A milk allergy, like all food allergies, is caused by the malfunctioning of the body’s immune system. With a milk allergy, the immune system views milk proteins as hazardous invaders. Once a milk product is consumed, the immune system triggers the release of IgE antibodies with the goal of counteracting the allergens, which in this case would be the milk proteins.
Cow’s milk contains two proteins that are involved in a milk allergy, which are casein and whey. When you have a milk allergy you can be allergic to just one or both of these milk proteins. Casein is the curd or solid part of milk while whey is the liquid part of milk that remains after milk has been curdled and strained.
Certain factors may increase the risk of developing a milk allergy including: (10)
- Age: It’s more common for children to have a milk allergy.
- Family history: The risk of having a food allergy such as a milk allergy is greater if one or both of your parents have a food allergy or another kind of allergy including hay fever, eczema or asthma.
- Other allergies: Many children allergic to milk also have other allergies. Milk allergy is often the first to develop.
- Atopic dermatitis: Children who have atopic dermatitis, also commonly known as eczema, are much more likely to develop a food allergy.
Conventional Treatment
There is currently no cure for milk allergy. Allergen immunotherapies for treating food allergies are in the works, but oral immunotherapy has not been approved for any food allergy in the U.S. to date. Researchers have already experimented with some success on how oral immunotherapy may be able to help treat a milk allergy.
It’s recommended that you speak with your doctor about how bad your milk allergy is and what foods you should avoid. Conventional medical resources will also tell you that the only way to prevent an allergic reaction to milk is to avoid milk products in the first place. So to avoid the cause of the allergy is the best treatment.
The severity of a milk allergy can also vary from person to person. For example, some milk allergy sufferers can tolerate milk in certain forms such as yogurt or the heated milk in baked foods. If you or your child has a milk allergy, antihistamines are conventionally recommend for mild milk allergy symptoms in the case of accidental milk consumption.
For babies, the best cow’s milk allergy formula alternative is always breast milk but conventional doctors may recommend vitamin and mineral enriched soy-based formulas.
How to Manage a Milk Allergy
1. Follow a Dairy-Free Diet
Following a truly dairy-free diet is the surest way to avoid milk allergy symptoms. According to the American College of Allergy, Asthma & Immunology, “Avoidance of milk or items containing milk products is the only way to manage a milk allergy.” (14)
So the best way to deal with a milk allergy from both a conventional and natural perspective is to avoid dairy products and also any other products that contain milk protein. Looking at a list of dairy products can be helpful if you’re not sure what to avoid. It’s always key to read food labels, even of dairy-free foods because not all of them are truly dairy-free!
2. Know the Obvious Things to Avoid
You can’t follow a dairy-free diet if you don’t educate yourself on what you need to avoid. If you have a milk allergy, it’s not just milk you have to abstain from. For example, is butter dairy? Yes, it is.
There are a lot of products that you may or may not expect to be on the list of foods that contain dairy. You also need to avoid products that contain milk or any of the ingredients below if you want to steer clear of an allergic reaction.
If you have a milk allergy, you should avoid foods that contain milk or any of these ingredients:
- Butter, butter fat, butter oil, butter acid, butter ester(s)
- Buttermilk
- Casein
- Casein hydrolysate
- Caseinates (in all forms)
- Cheese
- Cottage cheese
- Cream
- Curds
- Custard
- Diacetyl
- Ghee
- Half and half
- Lactalbumin
- Lactalbumin phosphate
- Lactoferrin
- Lactose
- Lactulose
- Milk (in all forms including condensed, derivative, dry, evaporated, cow’s milk and milk from other animals, low-fat, malted, milkfat, non-fat, powder, protein, skimmed, solids, whole)
- Milk protein hydrolysate
- Rennet casein
- Sour cream
- Whey (in all forms)
- Yogurt
This is not a complete dairy products list, but it includes a lot of common offending milk products and milk-based ingredients.
3. Know the Less Obvious Things to Avoid
There are other less obvious sources of milk such as chocolate, baked goods, candies and artificial butter flavor, for example. Then there are some really unexpected products that may contain milk, like canned tuna (some brands contain casein), shellfish (can be dipped in milk to reduce fishy odors) and processed meat products like cold cuts are known to contain the milk protein casein as a binder.
Is potassium lactate dairy? Potassium lactate is the potassium salt of lactic acid. According to the FDA, it is added to foods as a flavor enhancer or flavor agent. ]
4. Beware of Seemingly Safe “Dairy-free” Foods
“Dairy-free” products may still contain milk derivatives, which are problematic for people with a milk allergy. A milk derivative is defined as a substance that can be made or obtained from milk. These “dairy-free” products are meant for people with lactose intolerance rather than people with an actual milk allergy.
Examples of milk derivatives include things like casein and whey, which are known for being at the root of a milk allergy. If you have a milk allergy, then it’s really important that you fully read labels. Even if something claims to be “dairy-free” or “non-dairy,” neither label has a regulatory definition in the U.S. For example, coffee creamers labeled “non-dairy” are commonly made from caseinate, a milk protein.
5. Use Truly Dairy-Free Milk Alternatives
There a lot of alternatives to animal-derived milk these days. Some of my favorite dairy-free milk options include coconut milk and almond milk. Just make sure that you opt for unsweetened versions of these milks so you don’t overdo it on sugar. Store-bought almond milk typically includes significant amounts of vitamin E, vitamin D and calcium.
Coconut milk is another tasty dairy-free milk option that is loaded with healthy fats. It also contains important nutrients like manganese, iron, phosphorus, potassium, selenium, copper, magnesium and more in each serving.
6. Breast-Feeding for Babies
According to Mayo Clinic, “Breast-feeding is the best source of nutrition for your child. Breast-feeding for at least the first four to six months of life if possible is recommended, especially if your infant is at high risk of developing a milk allergy.”
Dr. Axe highly recommends skipping soy-based formulas and breast-feeding if you can.
7. Cook at Home with Whole Foods
One of the best ways to steer clear of milk is to make more of what you eat at home and use whole foods. This way you not only know what is going into your meals, but you also can pretty much know exactly what the ingredients you are using truly contain. Using whole food ingredients avoids the ambiguity of food labels and manufacturers of processed foods.
Precautions and Possible Complications
If you or a loved one has a milk allergy then it is essential to always read the entire ingredient label of foods and beverages before consumption. Sometimes milk or milk-derived ingredients are within the list of the ingredients. Other times, milk may be listed in a “Contains: Milk” statement located underneath the regular list of ingredients.
It’s also important to note that food manufacturers voluntarily choose whether or not to include advisory statements such as “may contain milk” or “made in a facility with milk.” Ask your health professional if it is safe for you to eat products with such warnings, which are not currently required by federal labeling law. In general, speak with your health professional if you’re ever feeling unsure about whether or not a certain food item is problematic.
If you or your child experiences anaphylaxis (a severe, potentially life-threatening allergic reaction) to milk, use an epinephrine injection and get emergency medical care immediately. If you know that you or your child have the risk of experiencing anaphylaxis, then your doctor will probably recommend having injectable epinephrine, such as EpiPen, on hand at all times.
Children with a milk allergy are also more likely to develop hay fever as well as allergies to other foods such as peanuts, soy, eggs or even beef.
Final Thoughts
- It’s not fun dealing with a food allergy, especially when it’s something found in so many foods, but try not to be discouraged. Thankfully, there are now so many delicious and healthy alternatives to cow’s milk.
- There are also a lot of food manufacturers and restaurants that are being a lot more thoughtful when it comes to people’s food allergies, and it’s easier to find dairy-free options these days.
- In general, the best natural and conventional way to treat a milk allergy is to avoid milk and other dairy products in the first place. This is the only sure way to avoid an allergic reaction.




