This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
Hypoglycemia Symptoms to Look Out For & Ways to Naturally Treat Them
August 30, 2016

Uncontrolled glucose levels are one of the most common health problems in the world. Hypoglycemia symptoms frequently affect people with prediabetes or diabetes but are also linked with other health problems, including high blood pressure, high cholesterol and even arthritis. And although it’s rarely mentioned, hypoglycemia has been called “an under-appreciated problem” that’s the most common and serious side effect of glucose-lowering diabetes drugs. (1)
Those who are at risk for both hypoglycemia and hyperglycemia are not only people who are ill, overweight or inactive — anyone who consumes a poor diet and has trouble with normal glucose metabolism can develop symptoms. The standard American diet, which tends to be very high in things like refined grains and sugar but low in nutrients like healthy fats and fiber, contributes to hypoglycemia and related diseases.
What are some clues you might be experiencing hypoglycemia symptoms, and what kind of things can you do to help manage them?
Symptoms of hypoglycemia are often confused with other health conditions and can include sudden hunger, irritability, headaches, brain fog and shakiness. By managing your intake of empty calories, improving your diet, and paying attention to how meal timing and exercise affects you, you can help control low blood sugar symptoms and prevent them from returning.
What Is Hypoglycemia?
Hypoglycemia is a condition caused by low blood sugar levels, also sometimes referred to as low glucose. Glucose is mostly found in carbohydrate foods and those containing sugar and is considered to be one of the most important sources of energy for the body. (2)
Here’s an overview of how glucose works once it enters the body and the process of how our hormones regulate blood sugar levels:
- When we consume foods that contain glucose (such as fruit, vegetables, beans, grains and sugary snacks), glucose is absorbed into the bloodstream, where it’s eventually carried throughout the body into cells for energy.
- In order for our cells to use glucose, the hormone called insulin needs to be present, which is made by the pancreas in response to how much glucose we consume.
- Insulin helps our cells absorb the amount of glucose they need for energy, and then any extra glucose is sent to the liver or various muscle tissues to be stored as glycogen for later use.
- Other than storing glycogen as an energy supply that can be tapped when needed, we can also create fat cells (which form adipose tissue, or body fat) from extra glucose that we don’t need for energy.
- In healthy people, when blood glucose levels fall too low, the hormone called glucagon lets the liver know that it needs to release stored glycogen to keep blood glucose within a healthy range.
- If this process becomes impaired for any reason, blood sugar levels remain low and hypoglycemia symptoms develop.
The opposite of hypoglycemia is called hyperglycemia, which is the condition caused by high blood sugar (high glucose). Hyperglycemia commonly develops in people with prediabetes or diabetes if their condition isn’t well-controlled. Hyperglycemia causes symptoms related to diabetes, including increased thirst, urination, fatigue and dizziness.
Diabetics can also experience hypoglycemia if they suffer from drastic fluctuations in blood sugar levels due to mismanagement of insulin and glucose. In people with diabetes, hypoglycemia is often a serious side effect of taking blood-sugar-lowering medications (containing insulin) that make glucose levels drop too drastically or from not consuming a balanced, healthy diet. (3) Studies have found that repeated episodes of hypoglycemia can negatively impact someone’s defense mechanisms against falling blood glucose, resulting in significant complications, including a sixfold increase in the risk of dying from a severe episode.
Hypoglycemia Symptoms and Signs
Ever feel shaky, cranky and tired right before eating a meal? Or ever dieted and purposefully skipped eating, only to crave sugar and feel fatigued? Then you’ve experienced what it feels like to have low blood sugar.
The most common symptoms of hypoglycemia, in other words signs of low blood sugar, include: (4)
- Hunger, sometimes which can be intense and sudden
- Symptoms of anxiety, such as nervousness or shakiness
- Sweating, including night sweats that happen while sleeping (this is a sign of “nocturnal hypoglycemia”)
- Feeling dizzy or light-headed
- Becoming fatigued, tired or groggy
- Trouble sleeping and waking up feeling tired
- Feeling irritable and having mood swings
- Paleness in the face
- Headaches
- Muscle weakness
- Signs of brain fog, including feeling confused and having trouble working or concentrating
- In severe cases (including when diabetes medications are involved), seizures, coma and even death can occur. Diabetic patients are at the highest risk for severe hypoglycemia episodes, especially if they happen repeatedly over a long period of time. Severe hypoglycemic episodes in older patients with diabetes have been shown to be associated with an increased risk of dementia, heart disease, functional brain failure, nerve damage and death.
Remember that it’s possible to have symptoms of both hyperglycemia and hypoglycemia when blood sugar levels aren’t managed. Over time, these come with complications and often side effects that are indicative of prediabetes or diabetes, including fatigue, sugar cravings, changes in blood pressure, weight loss or gain, nerve damage, and nervousness.
Hypoglycemia Causes and Risk Factors
What are the underlying reasons someone develops hypoglycemia symptoms? The causes of hypoglycemia include:
Mismanagement of Insulin
Too much sugar in the blood can cause insulin to rise to high levels over and over again, which ultimately causes insulin resistance (when cells stop responding to normal amounts of insulin). This can lead to diabetes or other symptoms of metabolic syndrome in some cases but also contributes to fluctuating blood sugar levels in those who are not considered diabetic.
Poor Diet
Consuming too little food, going for long periods without enough to eat or having nutrient deficiencies can contribute to hypoglycemia. Fad-dieting/crash-dieting can also cause symptoms, since these usually involve eating small meals or skipping meals altogether. Some studies have found that, overall, insufficient food consumption was the No. 1 most common cause identified for severe hypoglycemia episodes. Referred to as “impaired counter-regulatory mechanisms,” this essentially means that not paying attention to your own signs of hunger can sometimes cause severe hypoglycemia symptoms.
Diabetes Medications
Diabetics are often treated with medications to offset their resistance to insulin’s normal effects — in other words to lower high blood sugar. Clinical trials have found that attempts to use insulin and glucose medications to achieve aggressive healthy blood sugar levels is associated with a threefold increase in the risk of hypoglycemia symptoms. This hypoglycemic effect is now considered by many experts to be a big problem, even “counter-balancing the benefits of intensive glucose control,” according to the Indian Journal of Endocrinology and Metabolism. Medications that can contribute to hypoglycemia include chlorpropamide (Diabinese), glimepiride (Amaryl), glipizide (Glucotrol, Glucotrol XL), repaglinide (Prandin), sitagliptin (Januvia) and metformin.
Medications Used to Treat Other Diseases
When some medications are combined with insulin, they can lower blood sugar too much. These include pramlintide (Symlin) and exenatide (Byetta).
Increased Physical Activity
Over-exercising and overtraining or not eating something after exercise can cause low blood sugar. Muscles use up glucose in the blood or stored glycogen to repair themselves, so it’s important to refuel after workouts in order to prevent symptoms.
Other Health Problems
Hormone imbalances, autoimmune disorders, eating disorders, organ failure or tumors that affect hormone levels can all affect the way insulin is released, glucose is taken up into cells and glycogen is stored.
Alcohol
Alcohol raises blood sugar, but afterward levels can fall too low.
Enzyme Deficiencies
Certain metabolic factors can make it hard to break down glucose properly or for the liver to release glycogen when needed.
High Levels of Stress
Stress can elevate cortisol levels, which interferes with how insulin is used.
Conventional Treatment for Hypoglycemia
According to the American Diabetes Association, conventional treatments for hypoglycemia are usually as follows:
- Making changes to your diet and lifestyle to better control blood glucose. This can include changing meal frequency or adopting a diabetic diet plan.
- Doctors often recommend consuming 15–20 grams of glucose (from carbohydrates) right away when hypoglycemia symptoms begin.
- Keep an eye on symptoms for about 15 minutes, and if you’re diabetic, check your blood sugar at this time.
- Eat at least a small snack every two to three hours to keep symptoms from returning. Snacks and meals should have at least 15 grams of carbohydrates.
- Sometimes doctor prescribe medications, including glucose tablets or gel, along with other medications to control hypoglycemia symptoms in diabetic patients. Sometimes injectable glucagon kits are used as a medication to treat someone with diabetes who has become unconscious from a severe insulin reaction.
Natural Treatments for Hypoglycemia
1. Follow a Hypoglycemia Diet
If you’ve had hypoglycemia episodes in the past, try following a balanced meal plan while keeping track of symptoms to learn how to normalize your blood sugar levels.
Foods that can be helpful for managing hypoglycemia symptoms include:
- High-fiber foods: Artichokes, green leafy vegetables, chia seeds, flaxseeds, beans, apples, pumpkin seeds, almonds, avocado and sweet potatoes are good choices.
- Healthy carbs: Carbohydrates are the main dietary source of glucose, but not all carbs are created equal. Good choices include brown or wild rice, sweet potatoes, sprouted ancient grains, legumes, and beans.
- Vegetables and whole pieces of fruit: Fruit and fresh fruit juice can be especially helpful to offset a hypoglycemic episode.
- Healthy fats: Virgin coconut oil, MCT oil, extra virgin olive oil, nuts and seeds (like almonds, chia, hemp and flax), and avocado are good sources.
- Quality protein: Wild fish, such as salmon, free-range eggs, grass-fed beef or lamb, raw dairy products (including yogurt, kefir or raw cheeses), and pasture-raised poultry are some of the best protein foods.
Foods that should be avoided include:
- Too much caffeine or alcohol
- Empty calories, including packaged goods that are highly processed
- Lots of added sugar
- Sweetened drinks
- Refined grains
- Fast food and fried foods
2. Rethink Skipping Meals or Cutting Calories Too Low
People with hypoglycemia or diabetes should eat regular meals throughout the day, have enough calories at each meal (usually including at least some healthy carbohydrates) and never skip meals altogether. Healthy snacks every few hours can also be helpful for keeping blood sugar stable and preventing dips in energy.
If you’re exercising and feel weak or dizzy, make sure you’re eating enough, take a break and consider having something small to eat beforehand. Refuel after workouts with a snack that contains a combination of protein and healthy carbs. If you notice that you have symptoms of hypoglycemia during the night while sleeping, consider having a snack before bed to prevent hypoglycemia overnight.
3. Talk to Your Doctor About Your Medications
If you take any medications that alter blood glucose or insulin levels, be very careful to monitor physical signs and symptoms carefully that might point to hypoglycemia. Research shows that symptoms of hypoglycemia can become progressively less intense over time or even diminish altogether, resulting in “hypoglycemia unawareness” in a significant proportion of patients with repeated episodes due to medications. Talk to your doctor about how you can track your blood sugar levels more accurately or if your dosage should be changed to lower symptoms.
Facts About Hypoglycemia
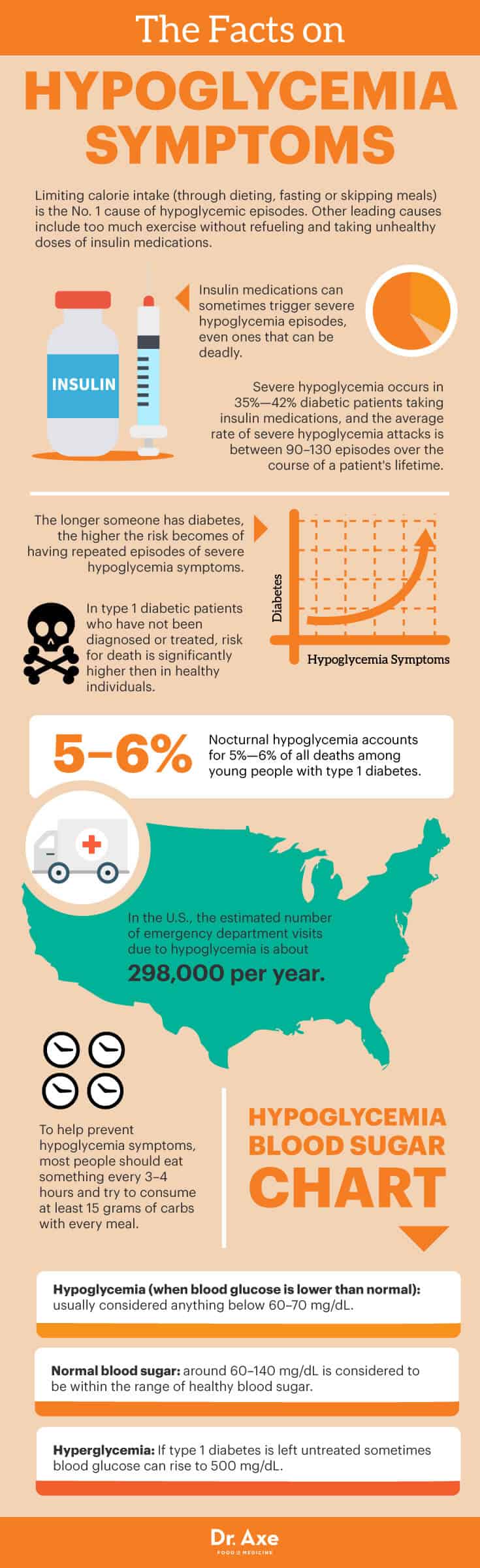
- Limiting calorie intake (through dieting, fasting or skipping meals) has been identified as the No. 1 cause of hypoglycemic episodes. Other leading causes include too much exercise without refueling and taking unhealthy doses of insulin medications.
- Insulin medications can sometimes trigger severe hypoglycemia episodes, even ones that can be deadly. Evidence from several studies suggests that severe hypoglycemia occurs in 35 percent to 42 percent of diabetic patients taking insulin medications, and the average rate of severe hypoglycemia attacks is between 90–130 episodes over the course of a patient’s lifetime.
- Studies have found that the longer someone has diabetes (for example, over 15 years), the higher their risk becomes of having repeated episodes of severe hypoglycemia symptoms.
- In type 1 diabetic patients who have not been diagnosed or treated, risk for death is significantly higher than in healthy individuals. For example, nocturnal hypoglycemia accounts for 5 percent to 6 percent of all deaths among young people with type 1 diabetes.
- In the U.S., the estimated number of emergency department visits due to hypoglycemia is about 298,000 per year. (5)
- To help prevent hypoglycemia symptoms, most people should eat something every three to four hours and try to consume at least 15 grams of carbs with every meal.
Hypoglycemia Blood Sugar Chart:
Wondering what levels of glucose in the blood are considered to be too high or too low? Generally speaking, experts agree that are no clear-cut borders between the normal range of blood sugar and high and low blood sugar levels. However, researchers and doctors often use the following blood sugar chart to categorize different conditions: (6)
Normal Blood Sugar
Around 60–140 milligrams of sugar per deciliter of blood (mg/dL) is considered to be within the range of healthy blood sugar. There is a normal “range” because even completely healthy people experience some fluctuations in blood sugar levels throughout the day depending on how they eat or their levels of activity. The international unit for categorizing healthy blood glucose is 3.3 and 7.8 millimole per liter (mmol/L).
If you’re generally healthy (you don’t have diabetes) and you haven’t eaten anything in the past eight hours (you’ve been “fasting”), it’s normal for blood sugar to be anything between 70–99 mg/dL (less than 100 mg/dL).
If you’re healthy and you’ve eaten within the past two hours, it’s normal for blood sugar to be anything less than 140 mg/dL.
Hypoglycemia
Usually considered anything below 60–70 mg/dL. If you do have a history of diabetes, fasting glucose should ideally also be below 100 mg/dL, which might need to be managed through the use of insulin. It’s also considered healthy to have levels between 70–130 prior to eating. If you have diabetes, you want to keep blood sugar between 100–140 mg/dL prior to bedtime and at least 100 mg/dL prior to exercising.
Hyperglycemia
If type 1 diabetes is left untreated, sometimes blood glucose can rise to 500 mg/dL ( 27.8 mmol/L). Levels this high are rarer in people with type 2 diabetes, especially if they take medications or use a healthy lifestyle to monitor their levels. If you have diabetes and you’ve eaten in the past two hours, the goal is to have blood sugar stay below 180 mg/dL.
Precautions Regarding Hypoglycemia
Always visit a doctor or the emergency room if you notice severe and sudden signs of hypoglycemia, including fainting. If you ever become unconsciousness or have a seizure and also take medications that might alter blood glucose, definitely mention this to your doctor.
If you’re diabetic, it’s recommended that you teach someone how to administer glucagon to treat severe hypoglycemic events and have that person call 911 if there’s an emergency right away. Don’t ignore serious signs, such as passing out, insomnia, rapid heart beats, etc., that continue over time, as this raises the risk for long-term complications.
Final Thoughts on Hypoglycemia
- Hypoglycemia is a condition characterized by abnormally low blood glucose (blood sugar) levels.
- Common symptoms of hypoglycemia include hunger pangs, shakiness, irritability, dizziness and fatigue.
- Causes of hypoglycemia include cutting calories, skipping meals, a poor diet, nutrient deficiencies and not eating after exercising.
- Severe hypoglycemia symptoms affect people with diabetes who are taking medications most often and are sometimes referred to as insulin reaction or insulin shock.
- Natural treatments for hypoglycemia symptoms include eating regularly every few hours, consuming a balanced diet, refueling after exercise and being careful not to overdue medications that interfere with blood sugar regulation.








