This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
Kidney Failure Symptoms & Natural Ways to Prevent
October 3, 2023
When kidneys work the way they should, they play an important role in keeping the whole body clean, strong, well-fueled and functioning properly. Conversely, kidney failure puts the body at risk, allowing waste to accumulate and wreak havoc, which is why it’s a good idea to do a kidney cleanse from time to time.
Healthy people normally have two kidneys, which are both about the size of a fist and located near the waste at either side of the spine. The kidneys sit just below the rib cage and have the primary role of helping the body with detoxification by getting rid of waste products.
Waste products that the kidneys filter include extra fluids, particles left behind in the digestive system, sodium/salt or other electrolytes, and various other substances found in the blood. Not only do the kidneys pass waste out from the body in the form of urine, but they also help control blood pressure, remove drugs or toxins, regulate hormones, and maintain a strong skeletal system (strong bones). Kidney failure, therefore, can be a very serious condition — requiring a high level of intervention, including dialysis treatments in order to do the filtering work the kidneys are no longer able to.
Waste product and fluid buildup, nausea or feeling sick to your stomach, trouble thinking clearly, and blood pressure changes are all symptoms of kidney failure. Kidney failure risk factors include having a history of diabetes and high blood pressure, in addition to consuming an unhealthy diet and having high levels of inflammation.
Steps you can take to lower your odds of developing kidney problems include consuming plenty of electrolytes (especially potassium and calcium) from whole foods, avoiding exposure to certain toxins or chemicals, and maintaining a healthy weight.
What Is Kidney Failure?
Kidney failure occurs when the kidneys stop working well enough to keep someone alive. Acute kidney injury (also called acute renal kidney failure) is the term commonly used to describe patients whose kidneys suddenly stop functioning as they normally should. This is characterized as “sudden loss of the ability of the kidneys to excrete wastes, concentrate urine, conserve electrolytes, and maintain fluid balance.”
There is no permanent treatment for kidney failure, only ways to help manage symptoms caused by failing kidneys and to keep a person as healthy as possible.
When the kidneys become severely damaged or “fail,” several types of ongoing treatments are used to clean the blood, prevent dehydration or fluid retention/swelling, remove waste products from the digestive tract, and ultimately replace the kidneys. Standard treatments for kidney failure usually include hemodialysis or peritoneal dialysis. Sometimes a complete kidney transplantation is also needed for certain patients with kidney failure or chosen out of preference in some cases when it’s a possible option.
Because acute kidney failure is a very serious matter, patients with this condition usually work with a team of medical professionals to monitor their symptoms, receive ongoing (sometimes lifelong) treatments and manage their overall health. Typically a patient’s treatment team includes seeing a combination of doctors who specialize in the kidneys (called nephrologists), nurses who administer dialysis treatments on average several times weekly, a dietician to help the patient get enough vital nutrients from the diet, and sometimes technicians or social workers to help improve quality of life in other ways.
Kidney failure facts and figures:
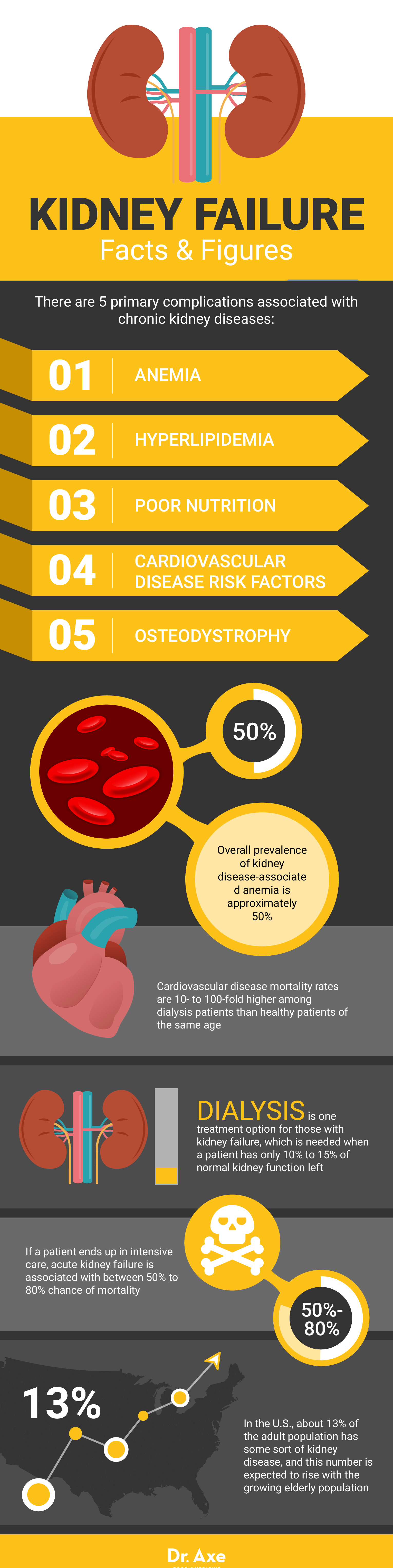
- Experts report that there are five primary complications associated with chronic kidney diseases and damage: anemia, hyperlipidemia, poor nutrition, cardiovascular disease risk factors and osteodystrophy (abnormal growth of bone mass associated with disturbances in calcium and phosphorus metabolism).
- Patients with chronic kidney problems and high risk for kidney failure experience much higher rates of the diseases mentioned above, especially heart complications and anemia. For example, the overall prevalence of kidney disease-associated anemia is approximately 50 percent, and cardiovascular disease mortality rates are 10- to 100-fold higher among dialysis patients than healthy patients of the same age.
- Many patients with kidney failure visit a hospital due to sudden symptoms, and this is where their diagnoses take place. If a patient ends up in intensive care, acute kidney failure is associated with between 50 percent to 80 percent chance of mortality.
- Chronic kidney disease is recognized as a major risk factor for kidney failure, and currently a significant global health problem. In the U.S., about 14 percent of the adult population has some sort of chronic kidney disease, and this number is expected to rise with the growing elderly population.
- Dialysis is one treatment option for those with kidney failure, which is needed when a patient has only 10 percent to 15 percent of normal kidney function left.
Symptoms
Because the kidneys are needed to properly balance ratios of water, salt and other minerals (called electrolytes) in the blood, kidney failure symptoms are very dangerous and often even life-threatening. However, it’s not always obvious to patients that kidney damage is contributing to their health problems — since the underlying reasons that the kidneys fail can cause all sorts of symptoms.
For some patients with unhealthy kidneys, no obvious symptoms are felt at all. Only suddenly “failure” of the kidneys occurs and then causes an emergency situation.
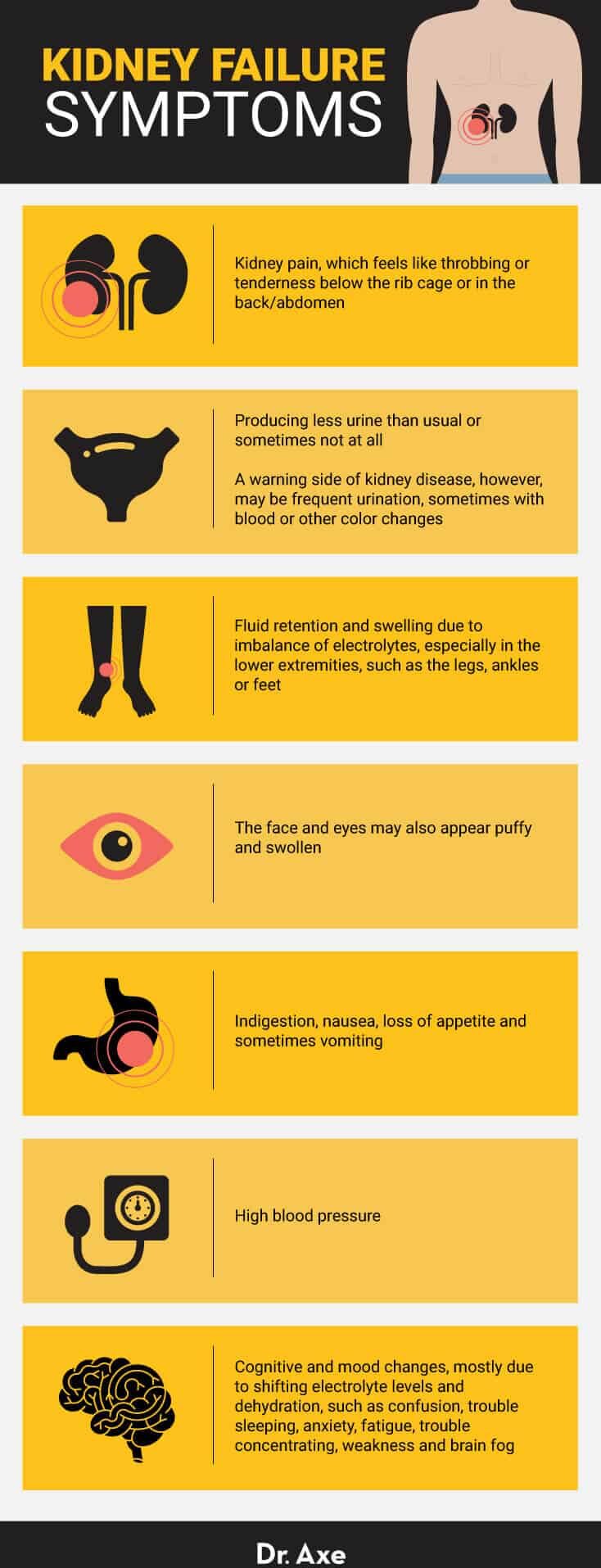
Kidney failure symptoms normally include:
- Kidney pain, which feels like throbbing or tenderness below the rib cage or in the back/abdomen (sometimes called “flank pain”)
- Producing less urine than usual or sometimes not at all. A warning side of kidney disease, however, may be frequent urination, sometimes with blood or other color changes.
- Fluid retention and swelling due to imbalance of electrolytes, especially in the lower extremities, such as the legs, ankles or feet. The face and eyes may also appear puffy and swollen.
- Indigestion, nausea, loss of appetite and sometimes vomiting
- High blood pressure
- Cognitive and mood changes, mostly due to shifting electrolyte levels and dehydration. These can include confusion, trouble sleeping, anxiety, fatigue, trouble concentrating, weakness and brain fog.
- Rhabdomyolysis, which is a apid breakdown of skeletal muscle that causes muscle proteins and other muscle constituents to leak outside of cells and into the bloodstream.
While kidney failure is very serious, it doesn’t always mean that someone needs to be put on dialysis forever or they’re necessary at risk of dying. Depending on the state of someone’s overall health — along with age and how many risk factors the person is up against — it’s possible to live a fulfilling life even with severely damaged/failed kidneys.
Sometimes severe kidney injuries can be resolved by treating the underlying problem causing the patient’s symptoms, but other times this unfortunately isn’t the case. Permanent kidney damage and chronic kidney disease cause a low percentage of patients to need ongoing dialysis treatments for the reminder of their lives, and with elderly patients this often shortens their life expectancy. For patients who wind up in the intensive care unit due to emergency kidney failure, it’s estimated that the risk of mortality is between 50 percent and 80 percent.
Risk Factors and Causes
The kidneys can fail for a few different reasons, primarily due to high amounts of blood loss, dehydration (which affects electrolyte levels), reactions from taking certain medications/ingesting toxins, or due to a blockage developing in the channels leading to and from the kidneys.
Risk factors for experiencing kidney failure include:
- Having a history of diabetes, anemia, high blood pressure, heart disease or heart failure. These can all affect blood flow to the kidneys and contribute to inflammation.
- Suffering from any other form of kidney damage or disease, including having chronic kidney disease, kidney stones (which are very common) or sepsis, an infection that slows down blood reaching the kidneys. Chronic kidney disease is a general term for heterogeneous disorders affecting kidney structure and function, which when left untreated can contribute to failure.
- Consuming an unhealthy diet or being very overweight or obese. A poor diet can result in electrolyte imbalances, nutrient deficiencies, higher levels of inflammation and changes in blood pressure, just to name a few of the related negative effects.
- Being an older adult. Increasing age raises your risk for various kidney problems.
- Having a history of prostate disease (an enlarged prostate), liver damage or liver disease. This affects how the body dispels waste and processes toxins, drugs, hormones and/or chemicals.
- Experiencing trauma or an injury to the kidneys that causes sudden blood loss.
- Having low immune function due to another illness, such as a virus that causes changes in electrolyte levels. High amounts of emotional stress, frequent infections or fatigue can also lower immunity.
- Being treated in a hospital or intensive care unit, such as having surgery or undergoing an organ/bone marrow transplant.
- Taking medications that can sometimes lead to kidney problems, such as antibiotics, painkillers, blood pressure drugs or ACE inhibitors.
Conventional Treatment
While your doctor might suspect you have damaged kidneys or kidney failure based on discussing your symptoms, medical history and risk factors with you, tests like blood tests and urine sample tests are used to confirm a diagnosis.
Sometimes ultrasounds are also needed to look for signs of swelling and inflammation in the kidneys and digestive organs. Ultimately, doctors are able to know someone is experiencing kidney failure by measuring their electrolyte levels, especially levels of sodium/salt, potassium and calcium.
Management of kidney disease or failed kidneys varies according to stages of disease severity. Once a diagnosis is made, kidney failure is typically treated in several ways:
- Restoring electrolyte levels and treating dehydration. Sometimes intravenous fluids are given to restore hydration, or diuretics are used if fluid retention and swelling is a problem.
- Altering medications that may be causing the problem
- If a blockage in the urinary tract is causing symptoms by not allowing the patient to urinate, then removing the blockage
- Treating any infection that’s related to symptoms, such as sepsis or an infection affecting other digestive organs
- Starting a program on dialysis if necessary
- Possibly prescribing medications to control levels of potassium, calcium, glucose or sodium. Medications can include Kayexalate and Kionex, which prevent the accumulation of high levels of potassium in your blood.
Prevention and Natural Remedies
1. Consume a Kidney-Healing Diet
Kidney disease alters metabolism of protein, water, salt, potassium and phosphorous, and kidney failure makes all of this even more complicated. A healthy diet is absolutely key for managing kidney disease or helping someone with kidney failure to have the best possible outcome.
Many patients with kidney failure visit a dietician to help analyze their current eating habits, nutrient levels and needs in order to come up with a treatment plan. That’s because there’s now strong evidence to suggest that a poor pre-dialysis nutritional status increases patient morbidity and mortality, even after initiation of kidney therapies. A poor diet stresses weak or damaged kidneys and contributes to various complications like anemia, cholesterol changes, heart damage and bone metabolism dysfunction.
The diet that’s best-suited to help you depends on the current health of your kidneys. Typically, you want to consume unprocessed foods that are nutrient-dense, such as high-antioxidant foods and foods loaded with electrolytes. Following this type of kidney cleanse diet is great for anybody with kidney stone symptoms or other risk factors. Specific foods to focus on include cranberries, blueberries, celery, burdock, leafy greens, fresh-squeezed vegetable juice, beets, cherries, sea vegetables like seaweed, spinach, avocado, bananas and citrus fruits like lemon.
It’s also important to prevent dehydration, since not drinking enough fluids can put you at risk for kidney complications (especially if you exercise a lot, live in a hot climate, drink diuretic beverages and sweat a lot). Drinking enough water and other hydrating fluids should become a regular habit, including herbal tea, sparkling water or fruit-infused water.
Experts recommend that anyone with kidney problems strongly monitor and limit certain electrolytes, including intake of sodium, potassium and phosphorus:
- Your doctor may recommend avoiding certain foods depending on your current nutrient levels, especially ones like dairy, processed meats, caffeine or alcohol, too much protein, and foods high in oxalic acid (spinach, rhubarb, tomatoes, collards, eggplant, beets, celery, summer squash, sweet potatoes, peanuts, almonds, blueberries, blackberries, strawberries, parsley and cocoa).
- To monitor intake of potassium, focus on eating whole foods like apples, cabbage, green beans, grapes and strawberries.
- Reduce your intake of high-sodium foods (salt) by avoiding packaged foods, frozen dinners, canned soups, fried foods, fast foods, and processed meats or cheeses.
- You can cut down on your intake of phosphorus by decreasing dairy (milk) consumption, legumes or beans, and nuts (especially peanuts).
2. Discuss Your Medications with Your Healthcare Professional
Certain medications or even vitamin supplements may make your kidney problems worse and may need to be discontinued altogether if they cause your problems. You can talk to your healthcare professional about the potential need to change blood pressure, cholesterol, painkiller, calcium or other medications since these are processed differently once the kidneys stop working properly.
To help prevent kidney damage from occurring in the first place, it’s also recommended that you limit use of over-the-counter pain medications (like Tylenol, prescription meds, Advil, Motrin IB and others), alcohol and tobacco products.
3. Prevent Kidney Damage with Herbs and Supplements
For anyone who has already suffered from kidney failure, you shouldn’t plan to take any supplements without consulting with your healthcare professional first. Because herbs and nutrients are metabolized differently once the kidneys fail, some may actually make matters worse.
However, for those who are looking to prevent further kidney damage, some of the following natural supplements may be helpful in keeping the kidneys and other digestive organs (like the liver) healthy. Just remember to get a professional opinion if you’ve already been diagnosed with chronic damage/disease/failure:
- Magnesium: Magnesium helps prevents the formation of kidney stones.
- Vitamin B6: Vitamin B6 may help reduce calcium-oxalate levels.
- Vitamin E: Beneficial for lowering calcium-oxalate levels.
- Cranberry extract: May reduce urinary calcium levels.
- Aloe vera: Helps reduce urinary crystals.
- Lemon essential oil and helichrysum essential oil: May reduce the risk of kidney stones by supporting the kidneys and liver in detoxification. Put two drops of citrus oils like lemon, lime, wild orange or grapefruit in your water twice daily. With helichrysum oil, rub topically over lower abdomen twice daily.
4. If Needed, Dialysis or Other Ongoing Treatments
Some patients need to receive dialysis treatments to remove waste, potassium and toxins in their blood. Temporary hemodialysis is sometimes only needed, but other times it needs to be continued for many years. Dialysis works by pumping and cleaning blood through a machine that acts just like an artificial kidney (called a dialyzer). Once cleaned, the blood is then returned into the patient’s body free from harmful waste. Both types of dialysis use cleansing fluids that either flow through a tube (catheter) into part of the patient’s abdomen to filter out waste or a system that flushes the patient’s blood through a special cleansing machine.
The two types of dialysis treatments used by most kidney failure patients are peritoneal dialysis and hemodialysis. The major difference is that peritoneal dialysis occurs within the patient’s body, not an external dialyzer machine. Both treatments may be performed at home with proper training from your physician (from a few weeks to a few months long) after the minor surgery required to insert a catheter specific to the type of dialysis you’ve chosen. Conventional home hemodialysis is usually done three times per week for about four hours at a time, while peritoneal dialysis treatment is typically done more frequently, about four to seven times per week at home.
Your doctor will need to discuss specific dialysis treatments with you so that you can make an informed decision, particularly because there any several variations within either type of dialysis and the best option will depend on your specific condition, lifestyle and needs. Some patients prefer peritoneal dialysis because it makes traveling easier. On the other hand, there are some reports that suggest home hemodialysis in “short daily” or “nocturnal” schedules may mean less medications for complications of dialysis, improvements in neuropathy and restless leg syndrome, more energy, better sleep, less hospital stays, better quality of life and even a larger lifespan.
In some cases, kidney transplants are also chosen as a treatment option, which have a high success rate in general. The kidney can come from someone who died, a living donor, a relative, friend or anyone who legally donates a kidney to someone in need.
Precautions
Because chronic kidney disease and kidney failure are potentially life-threatening illnesses, always be sure to get your healthcare professional’s opinion before treating these conditions. The information in this article is NOT intended to replace a one-on-one relationship with a qualified healthcare professional and is not intended as personal medical advice.
Final Thoughts
- Kidney failure occurs when the kidneys aren’t able to filter the blood, leaving behind wastes and excess fluid.
- Risk factors include a history of kidney problems, being obese, eating an unhealthy diet, or having diabetes, heart disease, anemia and bone metabolism problems.
- Prevention and treatments for kidney failure or kidney disease include eating a healthy diet (which varies from patient to patient but controls electrolyte levels), avoiding exposure to certain drugs or toxins, limiting heart disease or diabetes risk factors, and using herbs or supplements. In some cases, dialysis is used to replace the kidneys, since they’re no longer able to remove enough wastes and fluid from the blood.
