This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
Menopause Symptoms to Watch For and Ways to Relieve Them
July 17, 2024

Menopause is a fact of life for all women, like it or not. No matter who you are or where you’re from, if you’re a woman then at one point in your life you’ll have to deal with the menopause symptoms.
It helps to view menopause as a natural part of the aging process — not a medical illness or problematic condition, as some think of it.
When it comes to finding relief from menopause symptoms, the hardest part is often trying to overcome the emotional and physical side effects it brings along. Transitioning through menopause can mean dealing with unwelcome symptoms, such as weight gain, low energy, low sex drive and changes in your mood.
One of the most common ways to ease the sometimes-hard-to-deal-with side effects of menopause is to use hormone replacement therapy drugs. This generally involves taking estrogen and/or progestin replacement drugs or using hormonal creams.
However, the risk to a woman’s health from taking hormone replacement drugs has become a serious concern.
The good news is this: While the side effects of going through menopause can range from bothersome to debilitating, there are ways to handle it naturally without increasing your risk for certain diseases.
What Is Menopause?
Let’s take a look at exactly what menopause is all about — and what it’s not.
The Women’s Health Research Institute at Northwestern University explains that there are three stages of menopause:
- Perimenopause (before menopause)
- Menopause
- Postmenopause (after menopause)
Unlike what many think (or how it might feel), menopause doesn’t last forever, and your body does become accustomed to the new changes with time. How long it takes depends on each individual woman, her own body and her state of overall health.
Menopause is the permanent end of a woman’s menstrual cycle and therefore her years of fertility.
Technically, menopause is considered to start one year following a woman’s last period (meaning she’s been experiencing “amenorrhea,” or no menstrual cycle, for one year). This means that 12 months after your very last period, you’re officially “in” menopause and likely already starting to experience some common menopause symptoms.
This time period signifies the end of reproductive ovarian functioning and a transition through various hormonal changes.
Menopause symptoms can first appear around the ages of 35–45, when your ovaries get smaller and stop producing the hormones estrogen and progesterone that control the menstrual cycle.
Typically, however, a woman doesn’t officially enter menopause until sometime between 45–55, though some women may be menopausal a little earlier or later than this. It really is individual for each woman.
Common Menopause Symptoms
The rate at which various reproductive hormones adjust during menopause varies widely from woman to woman, so symptoms of menopause can be very different for each person and also very unpredictable.
Hormones tend not to drop in a fast, linear fashion — rather they can spike back up at times, which helps explain why a woman’s period might still come and go during the transition through menopause.
What’s feared the most during menopause is not missing the monthly menstrual periods, but facing the side effects caused from a decrease in reproductive hormones in the body. The decrease of estrogen particularly seems to impact the hypothalamus, a part of the brain that’s often refereed to as “the thermostat of the body,” as it regulates body temperature, sleep patterns, sex hormones, moods and appetite.
What kinds of menopause symptoms can you expect to experience? Again, this depends on your unique hormonal makeup.
Studies have found that menopause symptoms range considerably in terms of how long they last and how intense they can become, because even women of the same age can have hormone levels that are very different at any given time.
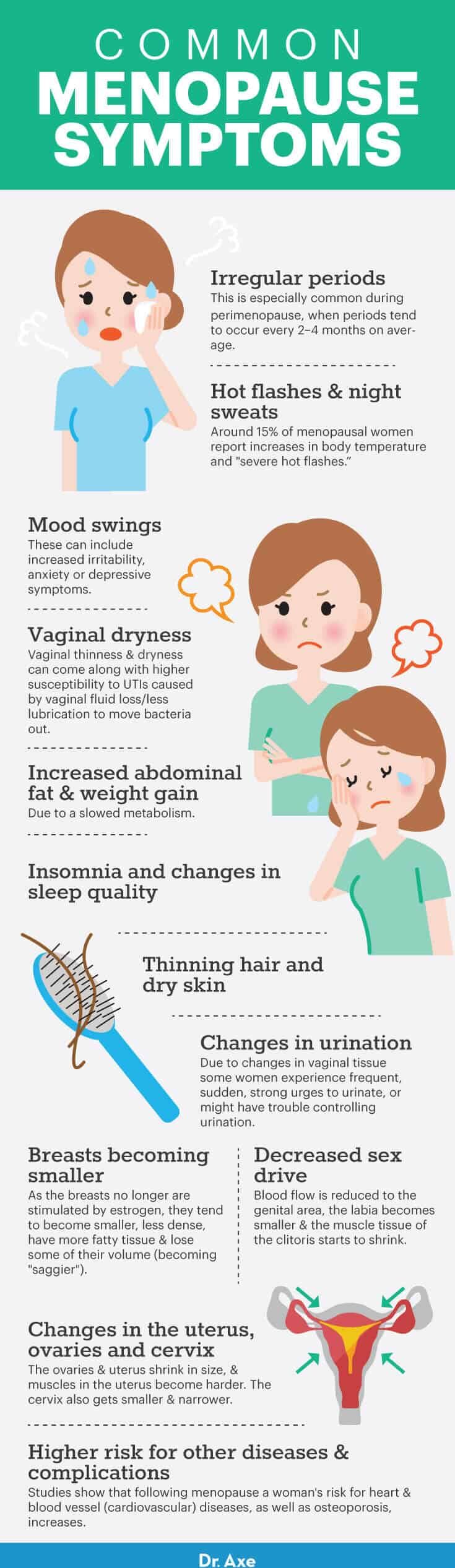
Some of the most common menopause symptoms include:
- Irregular periods: This is especially common during perimenopause, when periods tend to occur every two to four months on average. Periods can come and go, plus get heavier or lighter at times.
- Hot flashes and night sweats: John Hopkin’s University reports that about 75 percent of all menopausal women experience hot flashes (sudden, brief, periodic increases in body temperature), 80 percent of which occur for two years or less. Some menopausal women report having “severe hot flashes” caused by hormonal changes that affect hypothalamus, which controls body temperature.
- Mood swings: These can include increased irritability, anxiety or depressive symptoms.
- Vaginal dryness: The vagina technically shortens and loses elasticity (called vaginal atrophy). Vaginal thinness and dryness can come along with higher susceptibility to urinary tract infections caused by vaginal fluid loss/less lubrication to move bacteria out.
- Increased abdominal fat and weight gain: Due to a slowed metabolism.
- Insomnia and changes in sleep quality
- Thinning hair and dry skin
- Changes in urination: Due to changes in vaginal tissue some women experience frequent, sudden, strong urges to urinate or might have trouble controlling urination.
- Breasts becoming smaller: As the breasts no longer are stimulated by estrogen, they tend to become smaller, less dense, have more fatty tissue and lose some of their volume (becoming “saggier”).
- Decreased sex drive: Blood flow is reduced to the genital area, the labia becomes smaller and the muscle tissue of the clitoris starts to shrink.
- Changes in the uterus, ovaries and cervix: Although you likely can’t feel this taking place, the ovaries and uterus shrink in size, and muscles in the uterus become harder (fibrotic). The cervix also gets smaller and narrower.
- Higher risk for other diseases and complications: Studies show that following menopause a woman’s risk for heart and blood vessel (cardiovascular) diseases, as well as osteoporosis, increases. This is due to a decline in estrogen levels, which changes fat accumulation and also contributes to loss of bone density, weak bones and increased risk of fractures.
In addition to the common menopause symptoms listed above, the end of a woman’s period and fertility can often signify an emotional change in her life. Moving from a young, life-giving, fertile woman to an older woman can sometimes wreak havoc on the woman psychologically and emotionally.
However, that’s only the case if you let it be this way. If you work on understanding menopause, welcome and embrace it, and use appropriate therapies that don’t put your health at risk to deal with menopause symptoms, then this might even be one of the best, most meaningful times of your life.
How long does menopause last?
Most women transition through these changes for five to 10 years. For most, it’s closer to about five years, but symptoms might come and go for other women for much longer.
Causes
Menopause involves many natural changes to a woman’s entire reproductive system, including her internal organs, external genitalia, breast tissue (which is capable of secreting hormones), and various reproductive and non-reproductive hormones.
Around the time of your mid-30s, your ovaries start to produce less estrogen and progesterone, and therefore fertility starts to decline.
The hormones primarily involved in a woman’s reproductive system, and therefore menopause, include:
- Gonadotropin-releasing hormone (GnRH)
- Follicle-stimulating hormone (FSH)
- Luteinizing hormone (LH)
- Estrogen (three types including estrone, estradiol and estriol)
- Progesterone
- Testosterone
Prior to menopause during the reproductive years, estradiol is the major form of estrogen, which is released primarily from the ovaries. After menopause, estrone becomes the most abundant type of estrogen produced, which is mostly released from a woman’s fat cells and adrenal glands.
Estrogen works by attaching to receptors on cells within tissues, including those in the uterus and the breasts, and also the kidneys, heart, blood vessels and other tissues to a lesser degree.
There is isn’t one sole cause of menopause since it’s a very complex process. However, the most significant changes taking place in a woman’s body during this transition are that there’s increasing loss of ovarian follicles (called follicular atresia) and therefore a decreasing amount of estrogen being produced.
Mature follicles secrete estrogen, so as the rate of follicular loss keeps accelerating, less estrogen is produced. Estrogen levels start to drop six to 12 months before menopause (during perimenopause) and continue throughout the process.
Another thing to keep in mind is that every adult, whether going through menopause or not, experiences some signs of aging. As Harvard Medical School puts it, “it is often hard to say which changes are a direct result of a drop in hormone levels and which are natural consequences of aging. Some of the symptoms overlap or have a cascade effect.”
Conventional Treatment
Treatments including chemotherapy, radiation, surgery to remove the ovaries or hormone therapies can all interfere with hormone levels. This is one reason why women who’ve taken these medications/undergone treatments in the past tend to go through menopause at an earlier age compared to those who have not.
Studies show that taking hormone replacement therapies can increase a woman’s risk for several serious diseases, including:
- Breast cancer
- Heart disease
- Stroke
- Blood clots
- Urinary incontinence
- Dementia and memory loss
In fact, in one of the largest studies — the Women’s Health Initiative Hormone Program sponsored by the National Heart, Lung, and Blood Institute, the National Cancer Institute and parts of the National Institutes of Health — it was found that women on estrogen replacement drugs were more likely to develop breast cancer compared to women taking no hormone therapy medications at all.
Here’s more on the findings:
- The study followed two groups of women: one taking only estrogen replacement drugs and the other taking both estrogen and progestin drugs. The study began in 1991 and was abruptly stopped for the group using both estrogen and progestin in 2002 because the researchers found that the risks of using both drugs far outweighed the benefits. The study was stopped among the estrogen-only group for the same reasons in 2004.
- Other studies have found that in women taking hormone medications, breast cancer is more likely to be severe, deadly and spread to other body parts. There’s also evidence that both combination and estrogen-alone hormone use can cause mammography exams to be less effective for the early detection of breast cancer.
- Other than breast cancer, research shows a link between the use of hormone replacement therapy and diseases/conditions including stroke, blood clots, heart attack, urinary incontinence, dementia and possibly other types of cancer, including lung or colon cancer.
- The use of estrogen plus progestin has been found to double the risk of developing dementia among postmenopausal women age 65 and older, and either combined hormone therapy or estrogen alone has been shown to significantly increase risk of stroke, blood clots and heart attack while taking medications.
This isn’t a pretty picture, especially considering menopause is a normal part of the aging process that won’t last forever. Many of the common side effects associated with menopause can be effectively handled with safe and effective all-natural remedies.

Natural Remedies for Menopause Symptoms
1. Exercise
One of the best ways to combat many of the uncomfortable symptoms associated with menopause is to make exercise a regular part of your daily routine. Exercise works wonders for menopausal women, and you shouldn’t underestimate the power of it.
Exercising not only boosts serotonin levels, thereby improving your mood, your appetite and helping you sleep, but the benefits of exercise have been shown to do even more.
A study published in the Endocrine Society’s Journal of Clinical Endocrinology & Metabolism in October 2018 found that midlife women transitioning to menopause may be able to lower their risk of developing heart disease and type 2 diabetes by focusing on exercise and eating a lower calorie diet.
“Previous studies have largely focused on cardiovascular disease and type 2 diabetes in postmenopausal women. This study is unique because it focuses on an earlier stage in women’s lives, the menopausal transition in midlife, to potentially prevent such diseases from occurring,” said lead study author Jennifer S. Lee, M.D., Ph.D., associate professor of medicine at the Stanford Medical Center.
Engage in 10–30 minutes of aerobic activity in the form of burst training, and practice weight training several times a week. Weight training increases your self-esteem and helps naturally balance hormones — plus it helps you maintain muscle mass, which is important for preventing weight gain.
It also strengthens your bones to combat osteoporosis, another condition that often comes along with menopause.
2. Herbal preparations
Many menopause supplements, herbs and foods contain natural hormones (such as phytoestrogens) or hormone-balancing properties that can help you ease in to this transition period.
While there are a number of options for treating menopause symptoms with herbal remedies, some seem to be more effective than others. It’s wise to consult with a naturopathic doctor first, especially if you have other medical conditions and take medications.
Some of the most commonly used herbal remedies to treat menopause symptoms include:
- Ginseng
- Evening primrose oil
- Licorice root
- Black cohosh
- Wild yams
- Red raspberry leaves
- St. John’s wort
- Chaste tree (vitex)
- Sarsaparilla
- Red clover
- Dong quai
- Maca root
- Pollen extract
Each one of the above herbs has a specific symptom (or sometimes symptoms) that it’s able to help treat.
It’s important to note which of your menopause symptoms are most bothersome and start by treating those first, then work your way down the list.
This is where the knowledge of a trained naturopath doctor can be helpful. A doctor has extensive knowledge of which herb to use to treat your exact symptoms, which dosages are safest and advice about which herbs can be safely used simultaneously.
3. Healthy diet to help balance hormones
Eating a healthy diet is an often overlooked way to decrease troublesome symptoms of menopause, as well as to lower your risk for many other age-related illnesses.
Be sure that during this changing time you give your body all that it needs to adjust. Tips for eating a healthy diet to help balance hormones include:
- Eat plenty of fresh, organic fruits and vegetables every day. Not only during menopause (or any of the menopause stages), but throughout your entire life, it’s wise to eat fresh, locally grown organic foods that have undergone the least processing possible.
- Keep in mind that you might need to consume fewer calories overall in order to maintain your weight. Limit “empty calories” by reducing your intake of packaged or processed foods, added sugar, refined carbohydrates, sugary drinks, alcohol and refined oils.
- Fill up on high-fiber foods to help control your appetite, boost digestive health and benefit your heart.
- Drink plenty of pure, fresh water.
As close to nature as you can get a food (an apple picked fresh off the tree) is the best way to eat the majority of your foods. You’ll be amazed at how much better you feel in body, mind and soul when you indulge in these life-giving foods.
Plus, you’ll struggle less with controlling your weight.
Precautions
As with all treatments, natural or not, what works for one may or may not work for another. Our bodies are all unique, so it makes sense that different treatments work for different women.
There are no guarantees that natural remedies will help decrease all of your menopause symptoms, so it helps to be realistic about your expectations.
Some studies show that a few of the natural options described above are effective for a high percentage of women, while other studies show they don’t work well other women. This means that you may have to do a little research, try out a few different natural remedies and then decide what works best to combat your menopause side effects.
This does take some time and a bit of research, but it sure beats increasing your chances of getting debilitating diseases from using risky hormonal drugs.
Regarding use of herbal medicines for treating menopause symptoms, keep in mind that it’s important to buy high-quality, pure products and to use them in proper amounts. Compared to pharmaceutical or hormonal drugs, less is known about the potential side effects of herbs because studies are usually shorter-term and have smaller sample sizes.
The National Center for Complementary and Alternative Medicine is increasing funding for long-term studies into the effectiveness and safety of natural herbs/botanicals for menopause, but until we know more, look out for any signs of adverse side effects, including digestive complaints, bleeding, dizziness or fainting, allergies, and drops in blood pressure.
Final Thoughts
- Many women experience various menopause symptoms during their 40s and 50s, both due to natural changes in hormone levels and also as a side effect of aging.
- Some of the most common menopause symptoms include weight gain, trouble sleeping, abnormal uterine bleeding, hot flashes, decrease in sex drive and vaginal changes.
- Menopause symptoms can vary a lot in terms of their duration and intensity. More than 35 different menopause symptoms are considered “normal” and common — however, not every menopausal women experiences symptoms that cause a decrease in quality of life.
- Although menopause might feel inconvenient and hard, taking hormone replacement drugs can cause many side effects. A wiser option is to naturally manage symptoms through a healthy diet, exercise, stress reduction and sometimes using natural herbs.







