This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
What Is a Goiter? Symptoms, Causes & Remedies
November 2, 2022
Have you ever had a goiter (or goitre) or known someone who has? If you aren’t sure, the most noticeable sign of a goiter is a bulging in the bottom of the neck.
Small to moderate-sized goiters are actually relatively common in the U.S., and they can happen to people of all ages. For some people, they may even be present at birth. However, if you’re a woman or over 40, your chances are unfortunately even higher.
In general, thyroid conditions like goiters are becoming a more common health issue. Sometimes a goiter is just a temporary issue that goes away without any medical treatment. But other times, it can be an obvious sign that a more serious thyroid disease or disorder (also more broadly called an endocrine disorder) is present and needs to be dealt with right away.
Iodine deficiency is the most common cause of a goiter. Getting enough iodine from your diet on a regular basis is just one of the natural ways you can avoid a goiter. Let’s look at exactly what is a goiter, how can goiters be caused by or lead to other thyroid problems, and what is the best way to prevent and heal a thyroid goiter.
What Is a Goiter?
You might be familiar with a goiter as a bulge in the neck, but what exactly is a goiter? There are a few types of goiters (euthyroid goiter, simple goiter, sporadic goiter, endemic goiter, etc.) with various causes, but in general, a goiter is a swelling in the neck due to an enlarged thyroid gland. The size of the lump in the neck can be anywhere from one small nodule to a large, visible, multinodular goiter in the neck.
Goiters can arise when the thyroid gland doesn’t produce enough thyroid hormone (hypothyroidism) or when it produces an excessive amount of thyroid hormone (hyperthyroidism), but they can also occur when there is no malfunction of the gland (often called a “euthyroid goiter”).
Sometimes, though rarely, it is the result of the pituitary gland overstimulating the thyroid gland. Interestingly, many patients with Cushing’s syndrome, a disease commonly caused by the pituitary gland, often show a high prevalence of thyroid disorders as well.
No matter what, though, the presence of a goiter always means that there’s some condition present leading to abnormal enlargement of the thyroid gland.
What is the thyroid gland? The thyroid gland is a small, butterfly-shaped gland located in the neck, right below the Adam’s apple (which tends to be more prominent in men, but women have one as well). It’s an essential hormonal gland that produces two types of hormones, called triiodothyronine (T3) and thyroxine (T4), which help regulate blood circulation and metabolism, among other essential bodily functions.
Goiters may also occur with thyroid nodules, which are small lumps that can form on the thyroid gland. They may be solid or filled with fluid. Most of the time they are harmless, but sometimes they can cause hyperthyroidism or be malignant (cancerous). A goiter with several thyroid nodules is called a multinodular goiter.
Sometimes endocrine surgery is recommended to remove the thyroid gland if a thyroid nodule is causing hyperthyroidism, restricting breathing or swallowing, or if it is malignant.
Symptoms
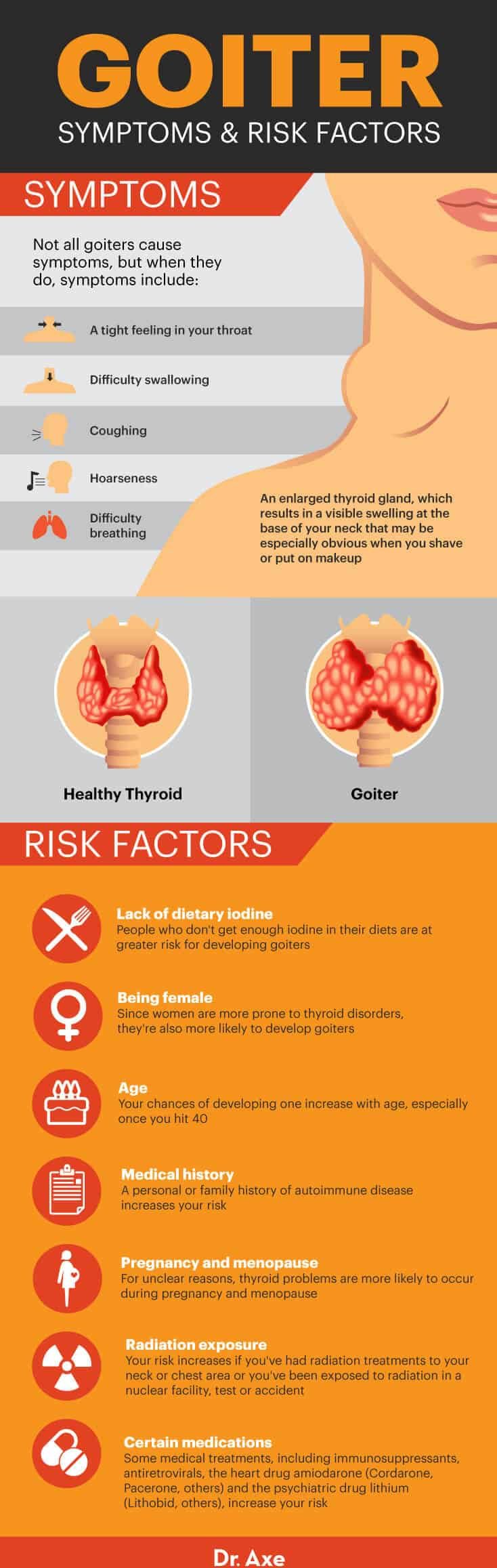
Thyromegaly, more commonly known as a goiter, is an enlarged thyroid, but what are enlarged thyroid symptoms exactly? First off, not every goiter causes symptoms. When symptoms do occur, they can include:
- An enlarged thyroid gland, which results in a visible swelling at the base of your neck that may be especially obvious when you shave or put on makeup
- A tight feeling in your throat
- Difficulty swallowing
- Coughing
- Hoarseness
- Difficulty breathing
In rare cases, a large goiter can put pressure on the windpipe (trachea) and food tube (esophagus). When a goiter is this large, it can become particularly hard to breathe when lying flat on one’s back. Swallowing can also be especially difficult with solid food, and there might even be pain the thyroid area.
A large goiter can also cause neck vein distention and dizziness when the arms are raised above the head.
Risk Factors
Some of the most common goiter risk factors are:
- Lack of dietary iodine — People who don’t get enough iodine in their diets are at greater risk for developing goiters.
- Being female — Since women are more prone to thyroid disorders, they’re also more likely to develop goiters.
- Age — Your chances of developing one increase with age, especially once you hit 40.
- Medical history — A personal or family history of autoimmune disease increases your risk.
- Pregnancy and menopause — For unclear reasons, thyroid problems are more likely to occur during pregnancy and menopause.
- Certain medications — Some medical treatments, including immunosuppressants, antiretrovirals, the heart drug amiodarone (Cordarone, Pacerone, others) and the psychiatric drug lithium (Lithobid, others), increase your risk.
- Radiation exposure — Your risk increases if you’ve had radiation treatments to your neck or chest area or you’ve been exposed to radiation in a nuclear facility, test or accident.
Causes
The causes of goiters differ between the three different types. With a simple goiter, the thyroid gland does not produce enough of the appropriate hormones to meet the needs of the body. Due to this shortage of hormones, the thyroid gland tries to compensate for this deficit by growing larger, resulting in a simple goiter.
An endemic goiter is caused by an an iodine deficiency. When iodine intake becomes severely low, the thyroid compensates for the decreased levels by developing a swollen thyroid gland, known as a goiter, in order to absorb as much available iodine. Iodine has been added to table salt (in the form of potassium iodide) since 1924. Originally, iodization of salt was adopted to reduce goiter occurrence.
Conventional medicine often says that sporadic goiters usually have no known cause. But for some people, certain drugs can lead to sporadic goiters. Lithium, which is used to treat certain mental health conditions and other medical conditions, is an example of a drug that can cause this type of goiter.
It’s also believed that eating really enormous amounts of goiter-promoting foods can cause a sporadic goiter. These foods include soybeans, rutabagas, cabbage, peaches, peanuts and spinach. The reason large amounts of these foods can be problematic to thyroid health is their ability to suppress the production of thyroid hormone by interfering with the thyroid’s ability to process iodide.
Other health conditions and diseases that have been linked to the development of goiters include Graves disease, Hashimoto’s thyroiditis, other forms of thyroiditis and pregnancy. Exposure to radiation can also contribute to goiter formation.
Conventional Treatment
The conventional treatment for a thyroid goiter depends upon the symptoms, size and underlying cause of the goiter. Sometimes a doctor suggests simply keeping an eye on a goiter if the patient has a normally functioning thyroid otherwise and the goiter is small in size and not causing any other issues. This is the “watchful waiting” approach.
Thyroid hormone replacement therapy is a common treatment for goiters that are caused by an underactive thyroid (hypothyroidism) or overactive thyroid (hyperthyroidism). Levothyroxine (Levothroid®, Synthroid®) is often prescribed in cases of hypothyroidism while methimazole (Tapazole®) and propylthiouracil are commonly used for hyperthyroidism. If the doctor believes there is an inflammatory cause of your goiter, aspirin or a corticosteroid might be recommended.
Radioactive iodine is another conventional treatment that’s used for goiters when they involve an overactive thyroid gland. The way it works is that you actually take the radioactive iodine by mouth, and when it reaches your thyroid gland via the bloodstream, it destroys thyroid cells, which can make the goiter smaller in size. The problem with this line of treatment is that it can lead to the other side of the spectrum — an underactive thyroid gland and hypothyroidism.
Surgically removing all or part of your thyroid gland (total or partial thyroidectomy) may be the recommended treatment if your goiter is very large to the point of being uncomfortable or it causes difficulty breathing or swallowing. Surgery may also be recommended for a nodular goiter that causes hyperthyroidism.
Depending on how much of the thyroid is surgically removed, ongoing thyroid hormone replacement drugs like levothyroxine might be needed after surgery and likely for the rest of your life.
For a large multinodular goiter, a biopsy may be needed to rule out cancer.
Natural Remedies
1. Iodine
Nearly 74 percent of normal, “healthy” adults may not be consuming enough iodine. In the developed world, iodine deficiency is said to be four times greater than it was 40 years ago.
An iodine deficiency can result in an enlarged thyroid gland or goiter because the thyroid tries to trap as many iodine molecules as possible. If the cause of your goiter is an iodine deficiency, increasing your intake of iodine-rich foods can help. The FDA currently has set recommended daily allowance for iodine at 150 micrograms, which is efficient enough to eliminate goiters that are prevalent in iodine-deficient areas. Foods high in iodine include seaweed, yogurt, baked potatoes and cranberries.
You can also look into iodine supplements. Studies show that even small amounts of supplementary iodine (250 micrograms) cause slight but significant changes in thyroid hormone function in predisposed individuals.
On the other hand, excess iodine not being absorbed by the body can also cause a goiter on the thyroid. It’s uncommon, but if getting too much iodine is causing your goiter, you can also tweak your diet to help get your iodine levels back in a healthy place. Excess iodine might be the problem if you’re eating too much shellfish. You should also avoid salt fortified with iodine, seaweed and supplements containing iodine.
2. Address Nutritional Deficiencies
In addition to iodine, some other nutrient deficiencies have been linked to goiter development. Specifically, deficiencies in zinc, manganese and vitamin A, along with severe protein malnutrition, may contribute to an inability for your body to properly utilize the iodine you take in and therefore can also lead to goiter formation.
3. If Hypothyroidism Caused the Goiter, Make Dietary Changes
An underactive thyroid, or hypothyroidism, is when the thyroid gland doesn’t produce enough thyroid hormone. Hypothyroidism is more common than hyperthyroidism. It can be found in about 5 percent of Americans while roughly 1 percent has hyperthyroidism.
If hypothyroidism is at the root of your goiter, there’s a lot you can do in terms of your diet and habits to treat your goiter and your underactive thyroid.
Some of the best foods to eat to improve an underactive thyroid include:
- Wild-caught fish like salmon and sardines
- Coconut oil
- Seaweeds like kelp, nori and dulse
- Probiotic-rich foods like kefir
- Clean water
- High-fiber foods
- Bone broth
- Fruits and vegetables
Foods to avoid to improve an underactive thyroid include:
- Goitrogen foods
- Tap water
- Conventional dairy
- Gluten
- Sugar
- Refined flour products
- Unfermented soy products like tofu and seitan
In terms of goitrogen foods, eating vegetables is generally very health-promoting, but when you have thyroid issues you should avoid large amounts of raw Brassica vegetables like broccoli, cauliflower, cabbage, kale and Brussels sprouts.
Why? Because they can negatively impact thyroid function due to their goitrogens, which are molecules that impair thyroid peroxidase. When consuming these cruciferous vegetables, it’s best to steam them well before consuming and keep portions moderate in size. This is an especially helpful tip for people who have iodine deficiencies.
4. If Hyperthyrodism Is at the Root of Your Goiter,
If an overactive thyroid is at the root of your goiter, examine natural ways to treat hyperthyroidism alongside common medical approaches. You should embark on a whole foods–based diet free of processed foods and avoid common food allergens like gluten and A1 casein (and getting tested for food allergies if you haven’t already).
There is some overlap between what to do and what not to do for both underactive and overactive thyroids, but it’s essential to know which one you are dealing with so you can use the proper natural treatment.
5. Consider Your Tea Intake
If you’re a lover of tea, you might want to consider cutting back if you have thyroid concerns. There are a lot of proven health benefits to black and green tea, but if you have thyroid issues, these teas’, especially green, high catechin content might possibly cause you trouble in very high amounts.
According to animal research, green tea extracts might have the potential to decrease thyroid hormones (T3 and T4) but increase thyroid-stimulating hormone. These are hormone effects that can contribute to or make hypothyroidism worse.
While moderate amounts of green tea might be OK, taking green tea supplements with a goiter and hypothyroidism might be particularly concerning. Speak with your doctor about your green tea intake, especially if you’re taking thyroid medication.
Complications and Precautions
In some cases, a toxic nodular goiter can develop from a simple goiter. This is mainly a disease of older adults. Risk factors for this toxic goiter include being female and over 55 years old. The majority of people who develop this have had a goiter with nodules for a number of years.
A goiter can also lead to hypothyroidism or hyperthyroidism if it’s not already being caused by one of these conditions. Hyperthyroidism can sometimes be caused by a nodular goiter, which causes the thyroid to produce excessive amounts of thyroid hormones.
You should always seek medical attention if you have any swelling in the front of your neck or if you experience any other symptoms. Sudden enlargement of a thyroid gland may indicate internal bleeding or the presence of an immune disorder, which requires immediate medical attention.
Progressive thyroid enlargement or the development of hardened nodules may indicate thyroid malignancy (cancer). If there is a single, dominant nodule or if a nodule is enlarging, a fine needle biopsy should be performed to rule out cancer. Be sure to consult with an endocrinologist, a doctor that specializes in endocrinology, or the study of the endocrine system.
Final Thoughts
- If you have a goiter (or goitre), it’s important to evaluate the health of your thyroid to get to the root of what’s causing your symptoms.
- No matter what, though, the presence of a goiter always means that there’s some condition present that’s leading to abnormal enlargement of the thyroid gland.
- A goiter can be a visual display of a more serious underlying thyroid issue, like hypothyroidism or hyperthyroidism.
- Iodine is nutrient that is absolutely critical to healthy thyroid function.
- Through a healthy and complete diet that addresses any nutritional deficiencies, you can help to naturally improve your thyroid health.
- Since women are more prone to thyroid conditions, they are also more prone to goiters.
- Goiters can happen to anyone, but if you’re over the age of 40 then you’re even more at risk.
- Balancing your hormones is an excellent way to ward off thyroid problems, including goiters.
- Even though goiters are typically painless, don’t just ignore one and miss the opportunity for it to possibly reveal more about your current physical state and give you a chance to improve your thyroid as well as your overall health.









