This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
8 Natural Treatments for Cholestasis
November 9, 2023

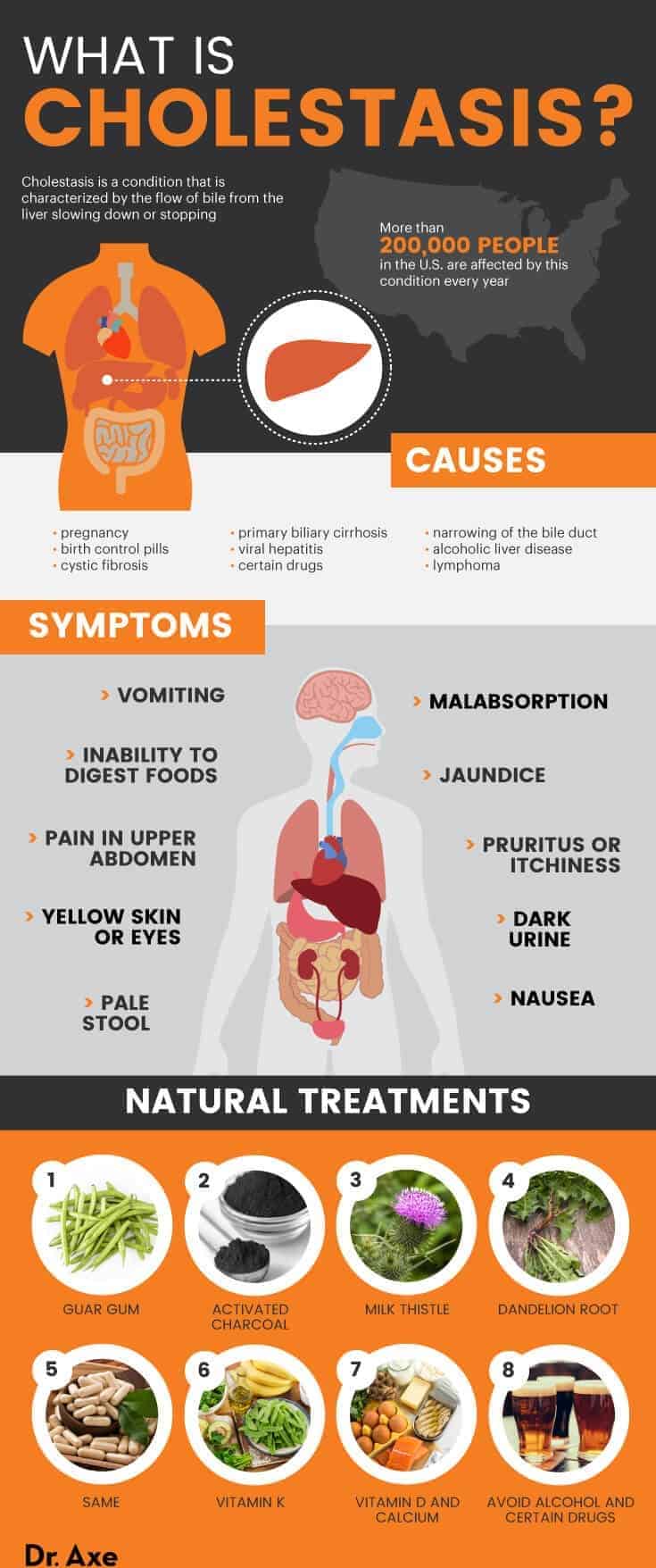
Cholestasis is a condition that’s characterized by the flow of bile from the liver slowing down or stopping, which can be caused by disorders of the liver, bile duct or pancreas. Up to 200,000 people in the United States are affected by this condition every year, and it can lead to serious health conditions if it’s not treated properly.
There are measures you can take to reduce your chances of developing cholestasis, and for people who are already suffering from this condition, there are natural remedies that you can depend on to help relieve the symptoms.
What Is Cholestasis?
Cholestasis is a condition in which the flow of bile is impaired at some point between the liver cells and the small intestine. Bile is the digestive fluid that’s produced by the liver. When bile flow is stopped, the pigment bilirubin, a waste product that’s formed when old or damaged red blood cells are broken down, escapes into the bloodstream and accumulates.
Normally, bilirubin binds with bile in the liver and moves through the bile ducts into the digestive tract, where it’s eliminated in stool, but for people with cholestasis, substances that are normally excreted into bile are retained.
There are several types of cholestasis, each with its own causes and characteristics. Here are some common types of cholestasis:
- Intrahepatic Cholestasis: Intrahepatic cholestasis occurs within the liver and is often related to liver diseases, such as primary biliary cholangitis (formerly known as primary biliary cirrhosis), primary sclerosing cholangitis or certain drug-induced liver injuries. It can also occur during pregnancy, a condition known as intrahepatic cholestasis of pregnancy (ICP).
- Extrahepatic Cholestasis: Extrahepatic cholestasis involves a blockage or obstruction in the bile ducts outside the liver. This can be caused by gallstones, tumors or strictures (narrowing) of the bile ducts. Extrahepatic cholestasis can lead to the backup of bile and can be painful.
- Neonatal Cholestasis: Neonatal cholestasis is a type of cholestasis that affects newborns. It can be due to various causes, including biliary atresia (a congenital condition where the bile ducts are absent or blocked), infections or metabolic disorders. It is important to diagnose and treat neonatal cholestasis promptly to prevent complications.
- Drug-Induced Cholestasis: Certain medications and drugs can cause cholestasis as a side effect. This type of cholestasis is reversible when the offending drug is discontinued. Common culprits include some antibiotics, anabolic steroids and certain herbal supplements.
- Benign Recurrent Intrahepatic Cholestasis (BRIC): BRIC is a rare genetic disorder characterized by recurrent episodes of intrahepatic cholestasis. There are two subtypes: BRIC1 and BRIC2, which are caused by mutations in specific genes. Symptoms can vary in severity and may include jaundice, itching and abdominal pain.
- Progressive Familial Intrahepatic Cholestasis (PFIC): PFIC is a group of rare genetic disorders that cause severe, progressive intrahepatic cholestasis in children. It can lead to liver damage and may require a liver transplant in severe cases. There are different subtypes of PFIC, each caused by mutations in specific genes.
- Alcoholic Cholestasis: Prolonged heavy alcohol consumption can lead to liver damage, including cholestasis. This is referred to as alcoholic cholestasis and can contribute to alcoholic liver disease.
Signs and Symptoms
Symptoms of cholestasis include:
- excessive itching
- jaundice
- nausea
- fatigue
- dark urine (perhaps cloudy urine, too)
- light-colored stool
- abdominal pain
The most common symptom of cholestasis is pruritus, or itchiness, which is thought to be due to interactions of serum bile acids with opioidergic nerves.
According to a report published in Gastroenterology and Hepatology, some studies report pruritus in up to 70 percent of patients with cholestatic liver disease, although more recent studies have reported lower rates of 20 percent to 30 percent. Pruritus is most common in patients with primary biliary cirrhosis, primary sclerosing cholangitis (scars within the bile ducts) and intrahepatic cholestasis of pregnancy, but pruritus is also fairly common in patients with chronic viral hepatitis, especially hepatitis C virus infection.
Jaundice is a common symptom of obstructive cholestasis, but it isn’t common in metabolic cholestasis. A person with cholestasis may also experience pale stool, which is associated with obstructive cholestasis, dark urine, nausea or vomiting, an inability to digest certain foods, pain in the right upper part of the abdomen, and yellow skin or eyes.
Cholestasis can lead to the improper digestion of lipids and fat-soluble vitamin malabsorption. It also can lead to reproduction and spread of bacteria to the lymph nodes, which may lead to endotoxemia and result in shock.
Causes
There are two basic causes of cholestasis. With obstructive cholestasis, there is mechanical blockage in the bile duct that occurs from gallstones and malignant tumors. With metabolic types of cholestasis, there is a disturbance in bile formation that occurs because of genetic defects or is acquired as a side effect of many medications.
Some other potential causes include:
- pregnancy
- birth control pills
- cystic fibrosis (an inherited disease that disrupts the functions of epithelial cells)
- narrowing of the bile duct
- alcoholic liver disease
- lymphoma (a form of cancer that affects the immune system)
- primary biliary cirrhosis (a disease in which the bile ducts in the liver are slowly destroyed)
- viral hepatitis
- drugs
- antibiotics (such as ampicillin and other penicillins)
- flucloxacillin
- erythromycin
- anabolic steroids
- nitrofurantoin
- gold salts
- statins
- estrogen
- cimetidine
- chlorpromazine
- prochlorperazine
Drugs continue to be a primary cause of cholestasis. Cholestatic injury is one of the most severe manifestations of drug-induced liver disease and accounts for close to half of all hepatic drug toxicity.
There is increasing evidence that drugs that are excreted by the liver into bile are prime candidates for producing cholestatic liver disease in susceptible patients, and prompt recognition and withdrawal of the offending drug are the primary goals in the management of drug-induced cholestasis.
Cholestasis of Pregnancy
Cholestasis of pregnancy can occur in late pregnancy, and it triggers intensely uncomfortable itching, usually on the hands and feet, but often on many other parts of the body. Cholestasis of pregnancy, also known as obstetric cholestasis, is a liver disease of pregnancy associated with raised serum bile acids and increased rates of adverse fetal outcomes.
The most common presenting symptom is pruritus — an unpleasant sensation that evokes the desire to itch. Pruritus typically becomes progressively more severe as the pregnancy advances and then resolves within 48 hours of delivery. Many women report that the itching worsens at night and may become so extreme that it causes insomnia.
According to research published in the World Journal of Gastroenterology, approximately 80 percent of affected women present symptoms of cholestasis after 30 weeks of pregnancy, but cholestasis of pregnancy has been reported as early as eight weeks.
Cholestasis of pregnancy creates serious risks for both the mother and infant. Elevated levels of serum bile acids increase the incidence of meconium passage into the amniotic fluid, which increases the risk of reduction of umbilical flow and sudden stillbirth.
Because mothers with cholestasis have a reduced ability to absorb fat-soluble vitamins — like vitamins A, D and K — properly, they’re at risk for developing a vitamin K deficiency, which can lead to intra-cranial hemorrhage in the infant and postpartum maternal bleeding for the mother. Spontaneous premature labor is also associated with cholestasis of pregnancy, and earlier presentations of cholestasis seem to carry an even greater risk of preterm labor.
According to a 2007 study published in the Orphanet Journal of Rare Diseases, ICP increases the risk of preterm delivery by 19 percent to 60 percent.
Conventional Treatment
Ursodeoxycholic acid (UCDA) is increasingly used for the treatment of cholestasis. UCDA is used to treat gallstones non-surgically and relieve itching in pregnancy for women who suffer from obstetric cholestasis. It’s a natural bile acid composition that improves liver function by replacing more toxic bile acids in the bloodstream.
UCDA works by modifying the bile acid pool, decreasing levels of endogenous, hydrophobic bile acids (bile that fails to mix with water), while increasing the proportion of nontoxic hydrophilic bile acids (bile acids that do mix and dissolve in water).
Management of Pruritus
According to Dr. Cynthia Levy, an associate professor at the University of Miami, the appropriate management of pruritus is very important because it can be distressing for patients and lead to a decrease in quality of life due to impaired sleep and depression.
Cholestyramine is recommended as the first-line therapy for management of pruritus. It works by increasing the removal of bile acids from the body.
Cholestyramine is associated with gastrointestinal side effects, including nausea, bloating and constipation, which often makes the drug difficult to tolerate.
Other commonly prescribed medications for pruritus include rifampicin, opiate antagonists (such as naloxone and naltrexone) and the serotonin reuptake inhibitor sertraline. Unfortunately, there have been few rigorous studies that confirm the efficacy of these treatments.
Natural Treatments
1. Guar Gum
Guar gum is a fiber from the seed of the guar plant. It’s commonly used as a laxative, for reducing cholesterol, and preventing diabetes and obesity. Guar gum works as a binding and stabilizing agent, which is why it may be useful in relieving symptoms of cholestasis.
A study published in the European Journal of Clinical Investigation investigated whether intestinal binding of bile by guar gum relieves cholestasis and pruritus in intrahepatic cholestasis of pregnancy. Forty-eight pregnant women with cholestasis and pruritus were given either guar gum or placebo until the time of delivery, and 20 healthy pregnant women were used as control subjects. Researchers found that the increase in serum bile acids and worsening of pruritus were prevented by guar gum in relation to placebo.
2. Activated Charcoal
Studies show that activated charcoal may be considered an alternative therapy in the treatment of intrahepatic cholestasis of pregnancy. Activated charcoal is a potent natural treatment that’s used to trap toxins and chemicals in the body, allowing them to be flushed out before they’re absorbed. The porous surface of activated charcoal has a negative electric charge that causes positive charged toxins and gas to bond with it.
A 1994 study found that after eight days of treatment, activated charcoal (at 30 grams, three times per day) was able to lower total bile acid concentrations in patients with ICP.
3. Milk Thistle
Milk thistle is a natural herb that’s commonly used to detoxify the body, especially the liver. It’s able to promote healthy digestive function by increasing bile production and decreasing inflammation.
Several studies indicate that milk thistle is effective in a variety of liver diseases, including cholestasis. It’s also safe to use during pregnancy and while breastfeeding.
4. Dandelion Root
Dandelion root and dandelion tea are safe natural remedies for cholestasis of pregnancy and have been proven to strengthen and benefit the liver. Dandelion root is used for gallstones, and it increases urine production and serves as a natural laxative.
Research shows that the vitamins and nutrients present in dandelions help cleanse the liver and keep it working properly. Dandelions aid the digestive system by maintaining the proper flow of bile, and they promote mineral absorption.
5. SAM-e
SAM-e, or S-adenosyl-L-methionine, is a molecule that’s formed naturally in the body and also made in the laboratory to help the body form, activate and break down chemicals in the body.
A study published in Drugs involving 639 patients with cholestasis due to acute or chronic liver disease found that SAM-e may act by promoting transsulfuration pathway reactions, which means that it helps metabolic pathways function properly and consequently improves the detoxifying capacity of the metabolic system. Researchers report that SAM-e appears to be the first safe and effective approach to the treatment of this syndrome, and it also protects against the adverse effects of small doses of estrogen in patients with a history of ICP.
6. Vitamin K
Vitamin K can be taken to improve blood clotting, unless your liver is severely damaged. It’s a suggested course of treatment for mothers with ICP because it reduces the absorption of fat-soluble vitamins that can lead to a vitamin K deficiency.
For women who are pregnant, a vitamin K deficiency can lead to serious complications for the mother and infant, including ICP.
7. Vitamin D and Calcium
Research shows that metabolic bone disease is common in patients with cholestatic liver disease. Researchers measured intestinal calcium absorption in relation to vitamin D status in 14 patients with chronic cholestatic liver disease, including 11 with primary biliary cirrhosis. They found that 57 percent of patients had a decreased calcium absorption compared to controls, and a significant correlation was observed between serum vitamin D levels and calcium absorption.
Treatment with oral vitamin D3 helped correct low vitamin D levels, which thereby improved calcium absorption.
8. Avoid Alcohol and Certain Drugs
People with cholestasis are advised to avoid or stop using any substance that’s toxic to the liver, including alcohol and certain drugs.
According to research conducted at the University of Sydney in Australia, agents known for many years to cause cholestasis include estrogens and anabolic steroids, chlorpromazine, erythromycin, and oxypenicillins. Contemporary drugs linked to cholestastic liver injury include ticlopidine, terfenadine, terbinafine, nimesulide, irbesartan, fluoroquinolones and cholesterol-lowering statins.
Offending drugs should be withdrawn immediately in order to treat drug-induced cholestasis.
While there is increasing evidence of a genetic predisposition to cholestatic drug reactions, there are currently no pretreatment tests to predict drug safety. Therefore, prevention of severe reactions relies on early detection of liver injury and prompt drug withdrawal.
Risks and Side Effects
Women with ICP should be sure to take herbal supplements only under the care of their health care providers in order to ensure that they’re safe during pregnancy.
People with chronic cholestasis can strongly impair uptake of dietary fat and fat-soluble vitamins, resulting in a variety of nutritional deficiencies. For this reason, it’s important that people with this disorder get a critical evaluation of nutrient deficiencies and adequate treatment strategies in order to improve their quality of life.
Final Thoughts
- Cholestasis in a condition in which the flow of bile is impaired at some point between the liver cells and the small intestine.
- There are two basic causes: With obstructive cholestasis, there is mechanical blockage in the bile duct, and with metabolic types of cholestasis, there is a disturbance in bile formation.
- The most common symptom is pruritus, or intense itchiness.
- There are herbs and supplements that can be used to relieve the symptoms of cholestasis, including milk thistle, guar gum, activated charcoal, SAM-e, vitamin K, vitamin D and calcium. It’s also important to avoid alcohol and medications that can trigger this condition.








