This Dr. Axe content is medically reviewed or fact checked to ensure factually accurate information.
With strict editorial sourcing guidelines, we only link to academic research institutions, reputable media sites and, when research is available, medically peer-reviewed studies. Note that the numbers in parentheses (1, 2, etc.) are clickable links to these studies.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
This article is based on scientific evidence, written by experts and fact checked by our trained editorial staff. Note that the numbers in parentheses (1, 2, etc.) are clickable links to medically peer-reviewed studies.
Our team includes licensed nutritionists and dietitians, certified health education specialists, as well as certified strength and conditioning specialists, personal trainers and corrective exercise specialists. Our team aims to be not only thorough with its research, but also objective and unbiased.
The information in our articles is NOT intended to replace a one-on-one relationship with a qualified health care professional and is not intended as medical advice.
6 Natural Alternatives to Psychiatric Drugs
February 17, 2018

Do you or a loved one take any so-called psychotropic drugs? It’s certainly no longer uncommon, as roughly 17 percent of American adults currently take at least one psychotropic drug. (1) These drugs are used in order to alter how the brain functions, usually in an effort to treat a mental illness of some sort. (Illegal psychotropic drugs are usually taken for recreational purposes.)
Unfortunately, after looking at the research, I believe that the benefits of these psychotropic/psychoactive/psychiatric drugs (or psychopharmaceuticals) do not outweigh the risks. Whether one takes an antidepressant, an anti-anxiety medication, a mood stabilizer, a hypnotic or some other brain-altering drug, the dangers of these psychoactive drugs are usually not fully understood before usage.
These dangers may include significant side effects (as in literally hundred of potential side effects), suicide risks, heart problems, even increased mental illness. Therefore, at no time is it more important to consider natural alternatives to psychiatric drugs — including natural remedies for depression and other mental illnesses — than now.
Natural Alternatives to Psychiatric Drugs
1. Eat a Healthy, Well-Balanced Diet
It may sound too simplistic to be true, but one of the best ways to combat mental illness is to eat better. For example, research shows that sticking to a diet rich in whole foods like vegetables and fruit, as well as a lot of fish, is associated with a lower risk of depression over time. (2)
Eating a great deal of organic fruits, vegetables, high-quality proteins and healthy fats will serve your body (and brain) well in staying in peak health.
In addition, probiotics benefit your body by maximizing the function of your gut-brain connection. Consuming foods and drinks with good bacteria, such as kombucha, may help protect you against leaky gut, which has been linked to both anxiety and depression. (3, 4)
Many people struggle to get enough probiotics via foods, as these products may be difficult to find in some areas. In that case, many people add probiotics in supplement form to their daily regimen to support the gut.
2. Exercise
In individuals with depression, the benefits of exercise may be just as or more beneficial than psychotropic drugs, particularly in the long-term. (5) One study found that, in older patients, antidepressant treatment result in a faster response in exercise, but that the results were equal in exercise versus medication after just 16 weeks. (6) The bonus being, of course, that exercise generally doesn’t cause side effects like the ones antidepressants do.
A meta-analysis of exercise or depression trials found encouraging results — in nine of the 16 included studies, exercise treatment groups were classified as “recovered,” with a remaining five study groups marked “improved.” In each trial, exercise significantly outperformed placebo at reducing symptoms of depression. (7)
Exercise may also benefit people suffering from anxiety, but not always as markedly. A meta-analysis of eight studies found that exercise significantly improved anxiety symptoms but was considered less effective than treatment with antidepressants.
However, patients suffering social phobia seem to benefit most from cognitive behavioral therapy (CBT) combined with exercise. The authors were unhappy with the overall quality of the randomized, controlled trials available for review, so the results should be reviewed with caution. (8)
3. Therapy
Many studies have examined the impact of therapy versus medication (or in conjunction) to help treat psychological illnesses. In a large grouping of meta-analyses, researchers from four universities in the U.S. made the following discoveries: (9)
- For depression, anxiety disorder, panic disorder (with or without agoraphobia), social phobia, posttraumatic stress disorder (PTSD), childhood depressive disorder and childhood anxiety disorders, cognitive behavioral therapy produced “large effect sizes” across the board.
- In the cases of adult depression, cognitive behavioral therapy performed “somewhat superior to antidepressants.”
- Cognitive behavioral therapy was equal to psychoactive drugs when treating adult depression accompanied by OCD.
- Individuals with bulimia and schizophrenia seemed to benefit greatly from cognitive behavioral therapy, but these experiments were generally “uncontrolled” and therefore should be interpreted with caution.
Some studies have reported an increased effect of using antidepressants along with cognitive behavioral therapy, greater than the effect of either one alone, namely fluoxetine and imipramine. (10, 11)
Other common types of therapy that seem to be effective when treating mental illness may include EFT (emotional freedom techniques) and ACT (acceptance and commitment therapy). (12, 13, 14)
Related: Lucid Dreams: When They Occur and How to Have Them
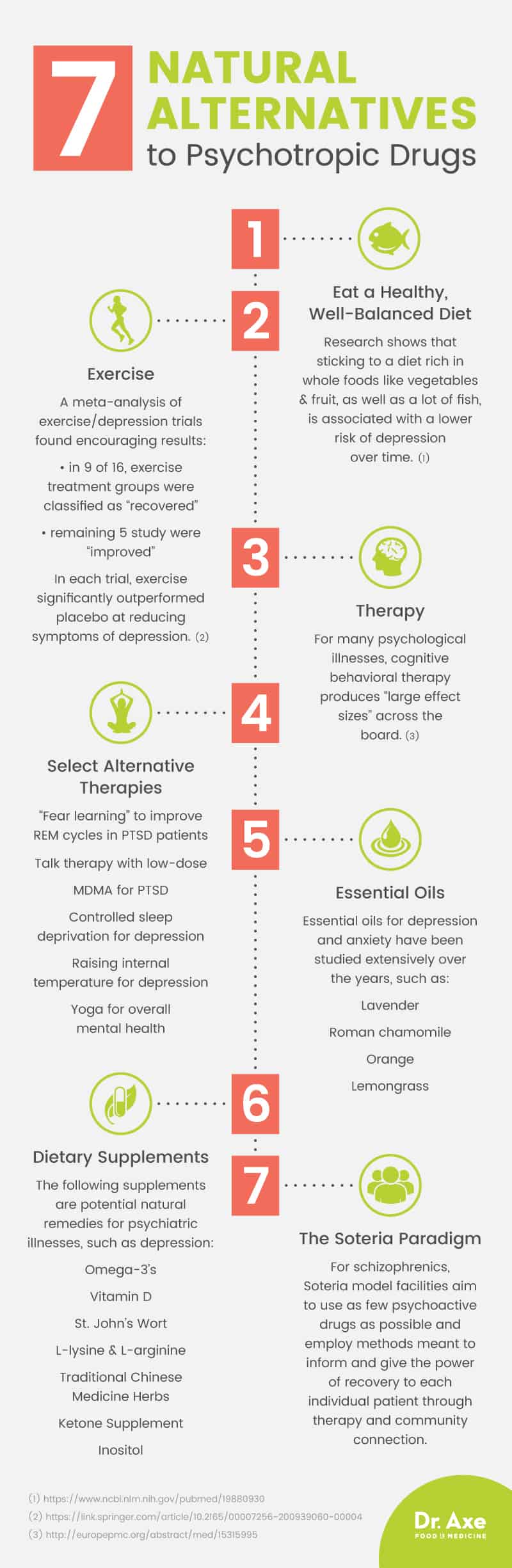
4. The Soteria Paradigm
The perceived necessity of psychotropic drugs is particularly high when it comes to psychoses like schizophrenia. However, as Whitaker describes, neuroleptics (antipsychotic medications) are often associated with a worse long-term outcome than other treatment methods. Neuroleptics also have an infamous reputation for poor patient adherence — so infamous, in fact, that schizophrenics “off their meds” appear frequently in modern entertainment.
Fortunately, other options do exist for in-patient treatment models. While many reports find that patients do not respond well to traditional psychiatric hospitals, the Soteria Paradigm was developed to combat that issue while giving patients an empowering, drug-free option when faced with serious psychiatric diagnoses. Essentially, Soteria model facilities aim to use as few psychoactive drugs as possible and employ methods meant to inform and give the power of recovery to each individual patient through therapy and community connection.
In a number of reviews comparing the Soteria Paradigm to traditional psychiatric hospitalization (in which drugs are the first line of treatment), Soteria model facilities are just as or more successful in helping to reduce psychotic symptoms in as little as six weeks for patients with schizophrenia, all while using little to no medication. In fact, these facilities operate at a considerably lower cost than their conventional counterparts!
One of the reviews confirmed that 85–90 percent of both acute and long-term clients in need of immediate hospitalization for their mental illness were able to return to their community without ever taking psychoactive drugs at all. (15, 16)
Why does it work? To quote a 2004 review of the method, “Soteria acts like a neuroleptic drug, but without its unfavorable side effects.” (17)
As long ago as 1977, scientists began to recognize that using no drugs “during an acute psychotic episode does not necessarily result in a disadvantageous course and outcome, and it may have some advantages.” When comparing conventional treatment methods to a community-based method similar to the Soteria Paradigm, these researchers discovered that patients in the no-drug settings said such a place enhanced their lives and that the information they were given was gratifying and empowering. On the other hand, drug-treated patients experienced more frustration and a feeling of “being frozen in the psychosis.” (18)
5. Dietary Supplements
Omega-3’s
If you can, you should be consuming a ton of omega-3’s in the foods you eat each day. Most sources suggest about 500 milligrams each day of EPA/DHA, which can be found in oily fish. However, if you aren’t able to consistently reach that goal, you may find a high-quality omega-3 supplement can help.
Can this dietary supplement actually do anything? Well, the science seems to shout a resounding, “YES!” In clinical trials (many of them “gold-standard” RCTs involving human subjects), omega-3 supplementation has had positive benefits treating:
- Depression and/or anxiety (19, 20, 21, 22, 23, 24)
- ADHD (25, 26, 27, 28, 29, 30)
- Schizophrenia, especially early-stage (31)
- Bipolar disorder (32)
- Antisocial behavior (33)
- Borderline personality disorder (34)
- Alzheimer’s and age-related cognitive decline (35, 36, 37)
Vitamin D
Most people know they feel better when they get some vitamin D from the sun, but some researchers have noticed that it could have deeper-reaching effects. One review found a “statistically significant improvement in depression with vitamin D supplements” in well-designed studies. (38)
There is also a hypothesis suggesting vitamin D impacts the risk of schizophrenia and/or may be able to be used as part of a treatment plan for the disorder. For example, supplementing with vitamin D during the first year of life seems to decrease the risk of schizophrenia in males, who are already overwhelmingly more likely to develop this mental illness. (39)
Dr. John McGrath, director of the Queensland Centre for Mental Health Research and professor at the Queensland Brain Institute, is a leading researcher in the field of vitamin D and serious mental illness, particularly schizophrenia. He states in a 2010 review he conducted that he believes it is time to examine vitamin D as a potential treatment for schizophrenia. In McGrath’s view, the results will likely be most significant for dark-skinned people who migrated to colder climates (not born there). These individuals are much more susceptible to psychosis, probably related to the connection between sun exposure and vitamin D. (40)
St. John’s Wort
A popular natural remedy for depression is St. John’s Wort, although the scientific results are somewhat mixed. Some research indicates it may have significant impact on symptoms of depression, potentially more than some SSRIs, with less adverse events. (41, 42)
Other trials report less positive results, or at least discourage clinicians from “prescribing” it as a treatment for depression, as the observed effects are sometimes small or inconsistent, and many studies of this antidepressant supplement are small. (43, 44)
Herbs in Traditional Chinese Medicine
Many herbs found in Traditional Chinese medicine (TCM) have been reported to improve depression and anxiety symptoms. Some of them include include:
- Chai hu (45)
- Ginkgo biloba
- Suan zao ren
- Passion flower (46)
- Kava root (47)
L-lysine and L-arginine
Both L-lysine and L-arginine are amino acids available in supplement form. In rats, L-lysine seems to decrease stress-induced anxiety symptoms, such as diarrhea. (48) The same result has been found in humans as well, focusing on communities with high cereal-based diets. Such communities don’t often eat foods containing much L-lysine and may be deficient. (49)
Research has also begun regarding whether or not L-lysine could impact symptoms of schizophrenia. There is not a consensus yet on dosages or long treatment periods, but the initial results are promising. (50)
Ketone Supplement
An innovative study released in 2017 tested the effect of a ketone supplement in rats fed a standard diet (not a keto diet). Fascinatingly, the rats experienced reduced symptoms of anxiety and anxiety-related behavior. (51) This is just an initial result and has not been duplicated or tested in human subjects, so interpret with caution.
Inositol
Commonly used by patients with PCOS, inositol is a compound found in particular fruits such as cantaloupe and oranges. It is also available in supplement form, and thus far has exhibited “modest effects in patients with panic disorder or obsessive-compulsive disorder” in current research. (52)
Probiotics
The gut-brain connection is a serious part of the development of psychiatric disorders. Replenishing your gut with healthy bacteria in probiotics may help with some of the symptoms of autism, anxiety, depression and manic depression. (53, 54, 55, 56)
6. Essential Oils
You more than likely have some “oily” friends who tell you all about how great essential oils are for their health — and they have a point. Essential oils for depression and anxiety have been studied extensively over the years, and several of them have impressive benefits, such as:
In fact, a 2014 human study revealed that Silexan (or lavender oil preparation) is a comparable treatment option to lorazepam in its starting dose for people with generalized anxiety disorder (GAD). (62) Those who reported that they received this treatment option highlighted that there were no withdrawal symptoms after taking the oral treatment. (63) It is also important to note that there are no reported adverse effects from ingesting lavender oil, except for minor gastrointestinal discomfort. (62)
7. Alternative Therapies
Other cutting-edge research in the mental illness field includes several exciting, breakthrough studies. Keep in mind that these are not generally conclusive results and are currently new, innovative ideas that have promising initial results.
- “Fear learning” to improve REM cycles in PTSD patients (63)
- Talk therapy with low-dose MDMA for PTSD (64)
- Controlled sleep deprivation for depression (65)
- Raising internal temperature for depression (66, 67)
- Yoga for overall mental health (68)
- A “rapid-gain” therapeutic treatment model for panic disorder, social anxiety, phobias and OCD (69)
Read Next: Antidepressant Withdrawal Symptoms — Worse Than You Think











